Rabies management in humans still inadequate
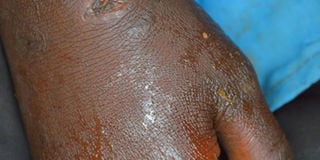
Bulima Muwada was attacked by a dog while chasing a cow from their potato garden above is his right hand healing from a dog bite photos by PAUL MENYA
What you need to know:
Rabies is a fatal disease among humans with survivors being only those who have received vaccines before the onset of the disease
When nine-year-old Bulema Muwada attempted to chase a cow from their potato garden in Bulonda Village in Bugoya Sub-county, Buyende District in eastern Uganda, little did he know that he would end up being bitten by a stray dog.
Muwada shares how his life changed on January 31. “I was at home when I saw a cow eating potato leaves in our garden. I decided to chase it away only to see a dog running after me. It first barked and then went on to bite my hands and back when I fell down,” Muwada recalls.
“I screamed and called out for help. When the people at home came to my rescue, the dog ran away but was later killed in our compound,” Muwada says as his father, Zaidi Muwiri nods in agreement. The Primary Three pupil of Adiswale Primary School, is still nursing injuries that resulted from a rabid dog bite.
Muwada was admitted to Lubaga Mission Hospital, a private facility where he received a rabies vaccine at Shs45,000.
According to hospital authorities, the boy was supposed to have a total of three vaccines but so far he has only got one.
When asked, his father says the family could not afford Shs90,000 for the remaining two shots. Muwada’s father says, “the government offers free rabies vaccines but they are not available in hospitals around here.”
The Ministry of Health defines rabies as a viral disease that is caused by the Rhabdovirus (Rabies Virus) affecting all warm blooded animals. It is a disease common among rural and urban populations of low socio-economic status.
How it is spread
According to the World Health Organisation (WHO), people are usually infected following a deep bite or scratch by an infected animal.
But transmission can also occur when infectious material – especially saliva – comes into direct contact with human mucosa or fresh skin wounds.
Human-to-human transmission by bite is theoretically possible, but has never been confirmed.
WHO reports indicate that rabies occurs in more than 150 countries and territories. More than 55,000 people die of rabies every year mostly in Asia and Africa.
Dogs are the source of most rabies related deaths in humans although 40 per cent of people who are bitten by suspect rabid animals are children under the age of 15.
The incubation period for rabies is typically one to three months, but may vary from one week to one year.
The initial symptoms are fever and often pain or an unusual or unexplained tingling, pricking or burning sensation (paraesthesia) around the site of the wound.
WHO adds that as the virus spreads through the central nervous system, progressive, fatal inflammation of the brain and spinal cord develops.
Risk factors
The Health ministry says about 10–20 individuals die and 5,000 are treated for rabies annually. More than 95 per cent of rabies cases originate from rabid dog bites with most cases being children aged between five and 19.
Experts say children are vulnerable as a result of their inclination to approach animals.
There is poor community awareness due to insufficient funding and inadequate supply of medicine for individuals bitten by rabid animals, leading many people to seek care from traditional healers.
The presence of many free-roaming and unvaccinated pets (dogs and cats) is a major risk factor contributing to the spread of rabies to the human population through bites of rabid dogs and cats.
According to reports from WHO, people living in rural areas are mostly at risk, because human vaccines and immunoglobulin are not readily available or accessible in such areas.
Reports show that the disease exists in two forms. The first form is furious where victims exhibit signs of hyperactivity (This is when more active than is usual or desirable), excited behaviour, hydrophobia (a set of symptoms of the later stages in rabies) and sometimes aerophobia (an abnormal and persistent fear of flying). After a few days, death occurs by cardio-respiratory arrest (the sudden and often unexpected stoppage of effective heart action).
The other, paralytic rabies accounts for about 30 per cent of the total number of human cases.
This form of rabies runs a less dramatic and usually longer course than the furious form. The muscles gradually become paralysed, starting at the site of the bite or scratch.
The patient slips into a coma and eventually death occurs. The paralytic form of rabies is often misdiagnosed, contributing to the under-reporting of the disease.
Expert analysis
According to the president of the Uganda Veterinary Association, Dr Dominic Lali Mundrugo-Ogo, rabies is the only viral disease among the 12 Neglected Tropical Diseases (NTDs) in Uganda, adding that it is not curable.
“Death is rapid once clinical signs including encephalitis (“madness”), abnormal behaviour, difficulties in swallowing, staggering, paralysis, altered vocalisation, and seizures have manifested,” Lali Mundrugo-Ogo observes.
With exception of buruli ulcer, plague and trachoma which are bacterial, the rest (NTDs) are parasitic and run a chronic course.
It is estimated that the population of dogs in Uganda stands at three million while that of cats is about 640,000.
With the poor veterinary care given to these animals, these pets pose a big risk factor in rabies transmission, health officials warn.
They add that the current dog vaccination coverage in Uganda is less than 20 per cent and there is no regular centrally planned mass vaccination programme for dogs and cats countrywide.
Loopholes
The Health ministry says the actual prevalence of both human and animal rabies in Uganda is currently not known because of inadequate surveillance system.
Therefore, there is a need to carry out the surveillance to actually determine the magnitude of the disease in the country.
Interventions in place
The Ministry of Health has put in place a rabies control programme that aims at improving the prevention and control of human rabies in Uganda. This is to be achieved through improvement of rabies surveillance in animals and humans, diagnosis, creation of awareness, regular vaccination of dogs and cats, improvement of animal welfare and treatment of people exposed to the disease.
In the National Master Plan for Neglected Tropical Diseases Programme 2013-2017, this strategy is usually successful if the vaccination of dogs is carried out at least once a year and with vaccination coverage of at least 75 per cent of the dog population.
The Ministry of Health together with health education and community sensitisation on rabies control is responsible for the execution of this mandate.
But already there are hiccups, the health ministry admits, “However, the vaccination of dogs and cats in Uganda and sensitisation programmes are not regularly carried out because of lack of funds to purchase rabies vaccines and other logistics and carry out sustained sensitisation campaigns.”




