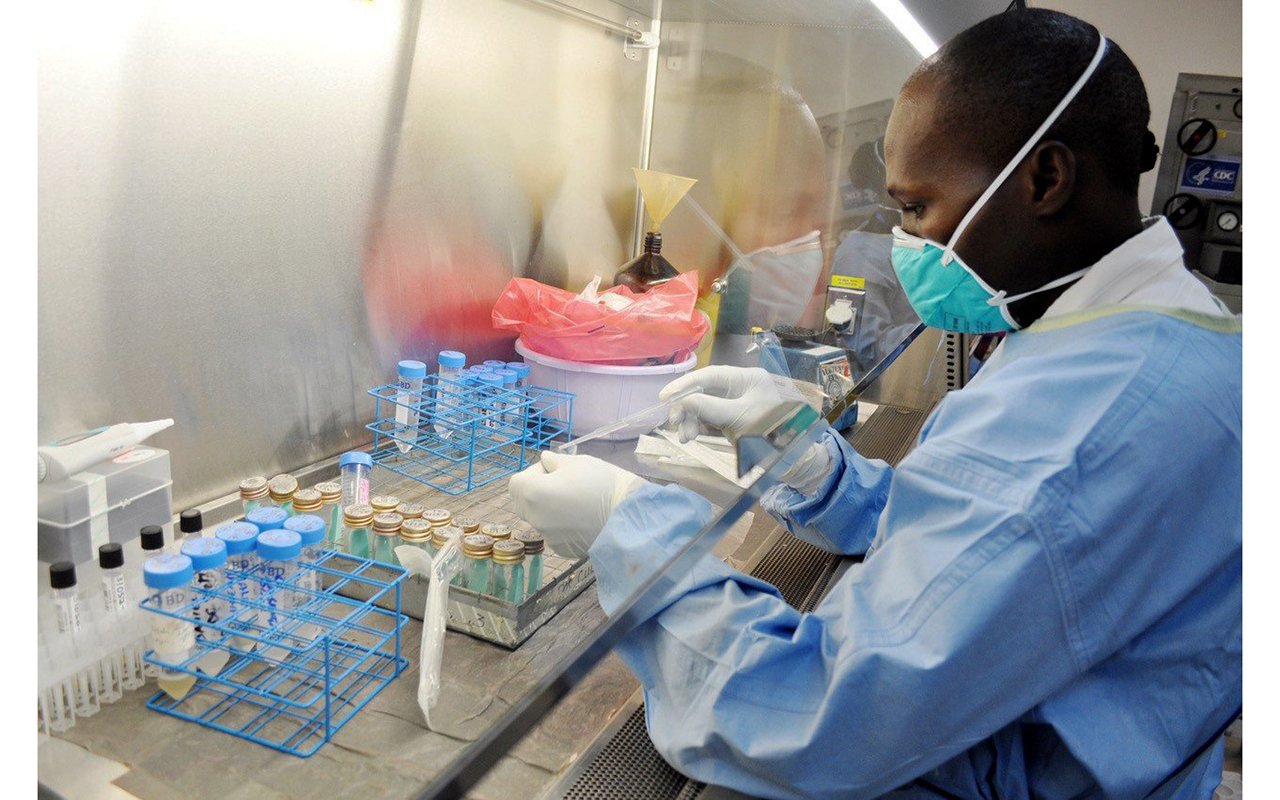
ARVs prolong life but do not cure HIV

Jane Zawedde, 64, sits at the front of her store, where she sells locally brewed liquor. Zawedde is HIV positive and each time she goes in for her refill of ARVs, Namugongo Fund for Special Children gives her three months worth of drugs. This has enabled Zawedde to live a healthy life. PHOTO BY HANNAH BOONE
What you need to know:
Antiretroviral therapy has been one of the biggest successes in the HIV fight. In this series, Hannah Boone, Jordan Canary, Brad Schuman, Bonnie Mailey, Mary Shown, Tae-Gyun Kim and Patience Ahimbisibwe look at how these drugs have bettered the lives of people but also the danger they have posed as many now believe the drugs are the answer and are living reckless lives.
It was 10am on a Friday and Jane Zawedde had already begun to slowly but surely bustle around her dimly lit shop, feeding the fire and boiling a kettle of water as she waited for her day to begin. The sound of cars speeding by and children laughing outside blended together, creating a familiar soundtrack for the businesswoman who has opened the shop day after day. Only four hours before that she had taken her daily dose of Alluvia, 3TC and TDF.
Jane is HIV positive, but you would not know it from just looking at her. Antiretroviral drugs, like the ones Jane takes, are seen as “miracle pills” when it comes to treatment and management of HIV.
Many names like Antiretrovirals (ARVs), Antiretroviral Therapy (ART), Highly Active Antiretroviral Therapy (HAART), HIV drugs and the ‘Lazarus pill’ are commonly used to refer to the drugs that have brought thousands of sick people back to life, but what is it exactly that these medications do?
To fully understand antiretroviral drugs, it is first important to know what a “retrovirus” is.
Dr Baker Lwasampijja, a pharmacist at the Joint Clinical Research Centre headquarters, laid out the basic physiology.
“You begin with DNA as the building block,” he said. “Then, DNA is transcribed into Ribonucleic Acid (RNA), which is the messaging system that makes basically anything that the organism is. Now, the funny thing about the viruses, they are naturally RNA.”
So, it is from this mutated RNA that the virus is able to “reverse transcribe” into DNA. That is where the term ‘retro’ comes from: the replication of the virus going through the reverse of the biological process.
Such a virus was always going to be hard to destroy. Perhaps that is why it took almost 10 years to develop a drug that would be able to curb its progression. According to the UNAIDS 2013 Country Progress Report, Uganda has a prevalence rate of 7.3 per cent, or about 1.5 million people living with HIV.
Approximately 793,928 of those people were enrolled on ART, 570,373 of which were actively taking their treatment. That means that 38 per cent of people who need treatment are actively receiving it.
Dr Alex Muganzi, Head of Mulago Infectious Diseases Institute’s (IDI) Outreach Department, stressed just how important these drugs are for positive individuals.
“It’s an infection you’re going to live with for the rest of your life, as far as we know at this point,” says Muganzi, adding. “If you start any treatments, you are going to take those treatments for the rest of your life.”
How do these drugs work?
HIV’s one battle tactic is replication. By replicating at a faster rate than an infected person’s immune system can, the HIV virus is able to take over the host cell and, eventually, the entire body. Since 1996, doctors have prescribed a three-drug combination regimen commonly referred to as HAART to combat the virus’s rapid copying methods.
People enrolled on HAART are usually prescribed two Nucleoside Reverse Transcriptase Inhibitors (NRTIs) and one Non-nucleoside Reverse Transcriptase Inhibitor (NNRTI).
However, those who have developed a resistance to first line are switched to second line drugs: two NRTIs and one Protease Inhibitor (PI). But, what do these drug classes do? What do these long, scientific names mean? It all begins at the mouth.
Orally taken ARV pills are absorbed through the blood. Once ingested, the pills quickly pass from the oesophagus to the stomach, where the pill is dissolved. Then, in the small intestine, the medication is absorbed into the blood vessels.
From here, the blood carries the ARVs through the circulatory system, sending each pill from each specific drug class on its way to fight the HIV virus.
It is through this highly effective combination of drugs that a positive-person is able to fight back against HIV, to prevent the replication process and stifle its progression.
“We can’t kill the virus, so the best thing that we are left with is to prevent it from multiplying,” said Dr Lwasampijja. “The hope is that when the already existing virus reaches its lifespan, it dies off without leaving new copies behind.”
People like Zawedde have managed to live longer because of these drugs. She goes about her work looking forward to receiving customers.
She is a good example of someone living positively. Yet, even with ARVs, Zawedde knows there is no cure for the virus.
She knows it all too well, in fact, because she is on second line treatment and has been for two years.
Although she feels fine now, Zawedde and others on second line must be extra careful about adhering to their regimens, because if they do not, the virus will attack ferociously. Should There is no cure for HIV and ARVs will only work for a certain time. Resistance is inevitable.
“Now people look at HIV medicines as normal medicines that bring people back to life,” said Dr Muganzi.
“People no longer look at HIV as the dangerous disease that made you lose 80 per cent of your weight, come down with chronic diarrhoea, get TB, meningitis. This is the biggest risk of treatment. Maybe we need to go back and look at what messages we’re putting across.”
Dr baker Lwasampijja: how the medication works once absorbed within the body
NRTIs (Nucleoside Reverse Transcriptase Inhibitors)
NRTIs interfere with a protein found in the HIV virus called reverse transcriptase. That protein is a mutated strand of biological code that pretends to be an immune cell’s DNA.
Without drugs, the CD4 cell would continue to replicate the mutation, leading to the deterioration of one’s immune system.
The DNA messaging system picks up the drug instead of the malfunction, creating nonfunctional products. So, through all of this, it stops the replication of the “replication protein”. Examples include truvada, abacavir and lamivudine.
NNRTIs (Non-nucleoside Reverse Transcriptase Inhibitor)
NNRTIs simply block the reverse transcriptase enzyme. When the virus begins to make copies of itself, there is a sort of unwinding process that happens. The RNA messenger protein normally splits or “unzips” the DNA molecule chain in order to duplicate it. Instead, the drug simply sits and prevents the unwinding, in turn stopping the message from sending and preventing the HIV mutation from spreading to other cells. (Examples: Efavirenz, nevirapine, etravirine)
PIs (Protease Inhibitors)
Protease is a different kind of protein. DNA strands, which are miles long in terms of the size of the CD4 cell, need to be chopped into smaller and smaller bits so that DNA messages can be easily transported.
Protease is the protein responsible for breaking it up, so PI drugs prevent this natural process from occurring. In doing so, the strand’s messages, already infused with HIV’s viral code, are stopped before they are able to spread throughout the immune system. (Examples: Invirase, saquinavir, ritonavir)