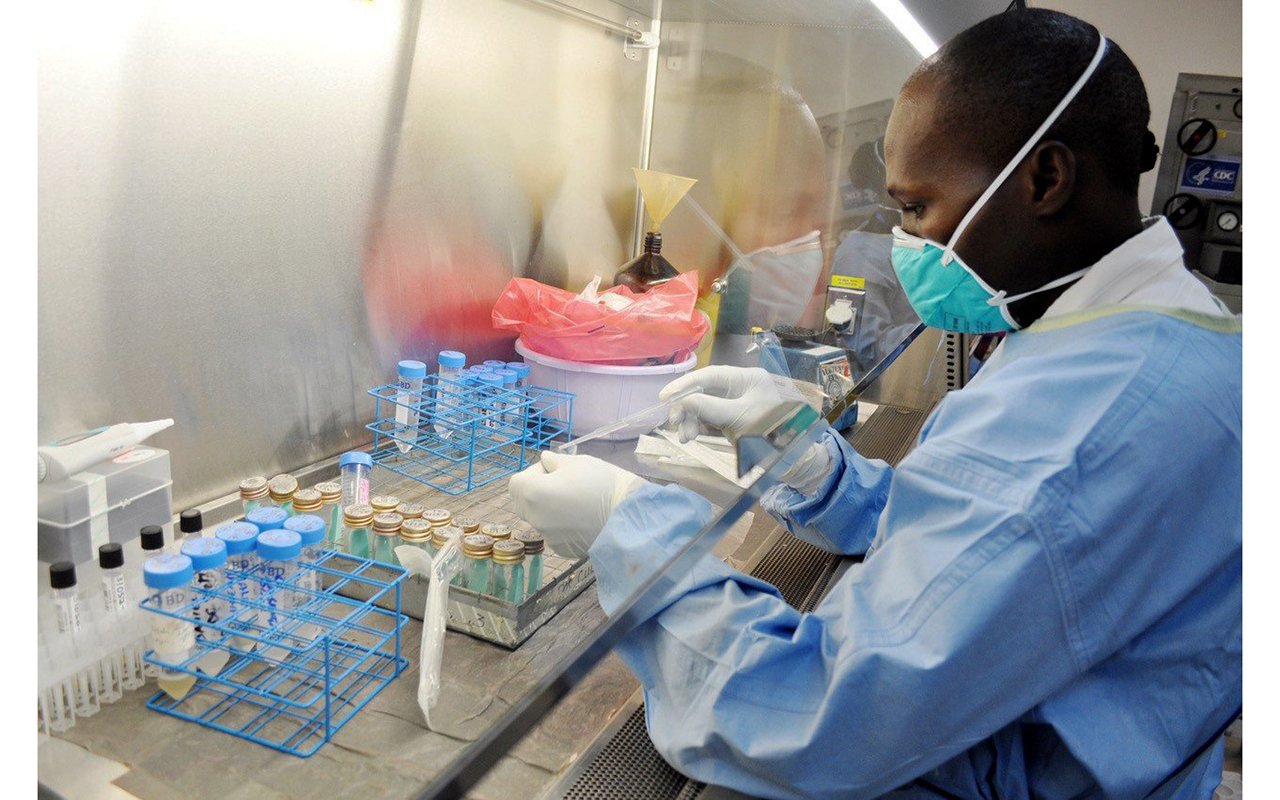
How safe is the blood you are getting?
Mr Gilbert Abwooli shows the machine, Architect i2000sr, at Nakasero Blood Bank that is used to test blood for HIV, and Hepatitis B and C viruses. PHOTO/FILE
While millions of Ugandans have donated or received this blood, it is always tough for either a patient or their relatives to accept it from a stranger even after it has gone through thorough routine blood screening. This is because questions are always posed regarding its safety. Most patients worry that the blood they are given may be infected by disease.
In the early years of the HIV epidemic, blood transfusions were risky and would transmit HIV infection, until the HIV test was availed where all the collected blood was subjected to methodical screening.
Even with assurances and reminders from the doctors and other medical personnel regarding the safety of the donated blood, questions are still asked as to whether this blood is 100 per cent safe from HIV, syphilis, Hepatitis B, Hepatitis C and other infectious viruses.
Some patients that are not in critical condition ask doctors for other blood supplement options.
Side effects
The blood transfusion process itself according to authorities attracts side effects for some patients. Some develop fever during or a day after blood transfusion which is explained as one’s body responding to white blood cells in the donated blood. Also, matching a donor’s blood type and that of a patient is key. If not properly matched, the patient may have a severe haemolytic reaction (a serious complication where red blood cells that were given in the transfusion are destroyed by the patient’s immune system).
Speaking about the safety of the donated blood, Dr Dorothy Kyeyune, the director at the Uganda Blood Transfusion Services Nakasero, explains that the entire process of guaranteeing blood safety begins in the field through proper selection of the donors.
“We usually target low risk communities like schools. Students have lower risk for transmission of HIV and regular donors like churches and mosques. People go through the donor screening process,” says Kyeyune.
This, she reasons helps to reduce the discard rate.
Blood is also tested through the use of the latest testing method of antigen-antibody combination assay which can detect HIV/Aids after some period of time.
The antigen-antibody combination helps in closing the window period (the time between HIV infection and appearance of antibodies to HIV) as HIV antigen is present in the blood before antibodies to HIV can be detected.
“We test the blood using the latest testing kit called antigen antibody test which can detect HIV in the blood. We test blood for HIV, Hepatitis B and C and syphilis; that makes it 100 per cent safe. The blood then goes to the laboratory before it is issued out,” Kyeyune states.
She says that before one’s blood is transfused, the donor is required to complete a health assessment questionnaire on the day of donation which is a personal statement of one’s medical and social history. On the questionnaire, a number of questions are paused to ascertain whether one is in good health to donate blood.
Various tests done
“It is our policy that blood has to undergo numerous tests. In hospitals, they are supposed to re-group this blood and cross match it. This eliminates any human error,” she says.
Dr Steven Aisu, the director and head of Central Public Health Laboratories however explains that this donated blood is not 100 per cent but 99.999 per cent safe.
He says that when screening for blood, health personnel screen for antibodies in which case if one is HIV positive and bleeds another, the problem may not be detected immediately since it is a very expensive process to detect one’s status in a few days.
“Medically you only give blood to cases that really need it,” he said, adding that blood should only be given as the last option and in emergency cases.
Available information indicates that a person is tested for HIV within the first three months after possible exposure for accurate results as most HIV tests are antibody tests which measure the antibodies a body makes against HIV. Also it takes some time (window period) for the immune system to produce enough antibodies for the anti-body test to detect. Detectable antibodies are seen within two to eight weeks hence the recommended routine testing even three months after the exposure.
Ninety seven percent of those infected develop antibodies in the first three months following the time of their infection and in rare cases, six months.
The team is usually cautious of the people that donate blood. Asked why they get blood from all categories of people before they are tested for HIV and other diseases, Dr Kyeyune says if you test before getting the blood, this may discourage potential blood donors from testing.
What then happens to the blood that expires or that that is found unsafe?
According to medical experts, blood has a short life span and expires every after 35 days, after which it is disposed of. Dr Kyeyune says such blood is autoclaved (heated up) and taken for incineration at the Mulago incinerator.
BEFORE YOU DONATE
Risk factors. Donors are questioned about whether they have any signs and symptoms of HIV or HIV risk factors.
One becomes a blood donor if they are 17 to 60 years old, weigh at least 45kg, have a haemoglobin level of at least 12.5g/dl, do not have any symptoms of infection within the last week, and have not had dental works within the last 24 hours.
THE RISKS FACED
Data from the National Heart, Lung and blood institute indicates that only about 1 in 2 million donations might carry and transmit HIV if given to a patient. Also, the risk of having a donation that carries Hepatitis B is about 1 in 200,000 to 1 in 360,000.