How culture has dealt blow to immunisation
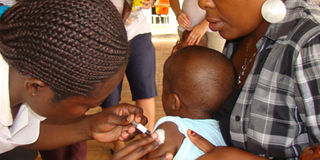
There are many factors affecting the uptake of vaccines in Africa. Among them are cultural perceptions, storage of vaccines as well as senstisation of communities
What you need to know:
Older people’s cultural beliefs influence their likelihood of embracing vaccination campaigns, writes Emmanuel Ainebyoona
Finda Nagobi, 65, a resident of Bukasero A in Mayuge District, claims her grandchildren fall sick whenever vaccinated during immunisation campaigns.
Found cultivating her garden, Nangobi’s home is located a few metres away from Lake Victoria. She says her grandson, Elia Twesigye, three-years-old, has been suffering skin rash since he was immunised during the January polio door-to door campaign.
“When they gave him the polio vaccine, Twesigye developed skin rush around the neck,” Nangobi says.
Not relevant
Sitting together with her grandson on bare ground and after moment of meditation, Nagobi adds: “I do not see the importance of immunisation because we were never immunised in our days.”
Like his mother, Nankora Kizito, 40, Twesigye’s father holds similar sentiments.
“Immunisation is not bad but once our children are vaccinated, they fall sick and it costs a lot of money to treat them,” Kizito says.
On top of falling sick after immunisation, his children also become pale.
However, Isa Samanya, the LCI chairman of Bukasero A, says the family were brainwashed by Njirinkulu, a religious sect they belong to. He says their religion bars parents from immunising their children, taking them to school or even engaging in government programmes, including the national identity card exercise and the National Housing and Population Census.
Measures in place
Samanya says: “Njirinkulu is also referred to as Triple Six. They disassociate themselves with anything that involves numbers because it is evil.”
During the polio campaign, they first kept indoors until the Gombolola Internal Security Officer (GISO) and police got involved to force them have their children immunised.
Valentine Owere, the Village Health Team Member (VHT), who is responsible for sensitising locals on government programmes, says religious sects are difficult to handle.
“They were compelled to participate in the last polio mass immunisation campaign but we are not sure if they will comply in the forthcoming campaigns,” Owere adds.
Uganda National Expanded Programme on Immunisation (UNEPI) attributes low immunisation coverage to various challenges, including: poor social mobilisation, insufficient community participation, inadequate use of evidence in family planning, poor leadership skills and broader health system issues.
Although government plans to involve religious leaders and the media to address the poor social mobilisation and community participation, some religious sects like Njirinkulu upset government plans to eliminate polio by 2018, by telling members not to abide by policy.
Andrew Bakainaga, the World Health Organisation (WHO) country advisor on immunisation and vaccines, argues: “We are not ignorant about the fact that there are naysayers. We are trying our level best by working with their leaders. For instance, in the east, we have seen some positive results.”
Evaluating feedback
“In terms of them (religious sects) claiming that their children get sick after vaccination. I think it is not proven because we have not had any case of any reaction of what we call aversive events of immunisation (AFI),” Bakainaga says.
“In case of any occurrence, we normally follow it up by investigation to find out whether it’s a health worker who administered the vaccine wrongly,” he adds.
Through Knowledge and Practices and Attitude (GAP) surveys, WHO is able to get feedback on the attitudes and perception on immunisation campaigns.
He also attributes negative perceptions to the “big anti vaccination lobby out there”.
He says, “In Busoga, we were told that vaccines are made out of pork and because most people there do not eat pork, vaccination campaigns were shunned.”
Advice
Dr Robert Mayanja, the UNEPI programme manager, says at least every child in Uganda should be immunised five times before their first birthday.
“The child should be immunised: At birth, at one and half months, two and half months, three and half months and at nine months,” says Dr Mayanja.
Immunisation is the most cost-effective intervention for controlling and eliminating preventable diseases during childhood and child bearing age for women.
Other contributing factors
But everything cannot be blamed on perceptions. For instance, the human papilloma vaccination (HPV) campaign that was planned for April was postponed to October due to storage challenges. The vaccine is aimed at protecting women from cancer of the cervix.
Vaccine storage is a major problem affecting immunisation campaigns in the country.
According to Dr Mayanja, some clinics in Kampala had resorted to using home refrigerators to store vaccines contrary to WHO storage recommendations.
That notwithstanding, Dr Mayanja says government is planning to introduce a law on vaccination which will compel parents to take their children for immunisation.
Factors influencing vaccine uptake
Incentives. It was found that financial incentives encouraged prenatal visits and childhood check-ups in France and Austria, and Britain used financial rewards to increase general practitioner vaccination rates.
Risk perception and decision making. Parents’ beliefs influence their acceptance of vaccination, and the perception of risk is subjective. Many non-vaccinating parents believe the risk of disease is low, the risk of vaccine side effects is high, and/or vaccination is ineffective.
Improving uptake. Health providers should listen to parents and treat their concerns seriously. In the past, minor illnesses were accepted as contraindications for vaccination; the change in policy and practice needs to be explained, and parents’ wishes should be respected if they are not convinced that it is in the interests of their children to be vaccinated when they are sick.
Information. Most people’s understanding of vaccines, vaccination and the diseases they prevent is gleaned from the printed media, but published anti-vaccination arguments may unduly influence them.
health.gov.au




