How reliable is the oral HIV test ?
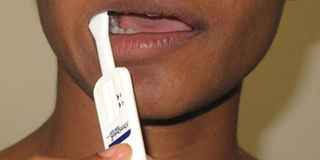
The oral self test must be done carefully to avoid misdiagnosis. Net PHOTO
What you need to know:
We live in a fast world where convenience is key. Methods of HIV testing have also been revised to match the times. You can now go to the pharmacy for an over-the-counter HIV testing kit to be used privately writes Promise Twinamukye.
Hiv is no longer a death sentence, but only if you know your status early enough so that if you test positive, you can start treatment early. Unfortunately, there are people who are infected with HIV but don’t know it because they refuse to get tested. For some, it is simply the need for privacy.
They are not comfortable going to a testing unit, clinic or hospital to get tested.
This is where the OraQuick HIV self-test kit test comes in. It offers the much needed privacy and convenience.
Dr Mark Juko from Masaka Regional Referral Hospital who used the test says,
“I bought a kit at Shs 25,000. At about 8pm, I prepared for the test. While I waited for the recommended 20 minutes to elapse, I was anxious. It was really more about knowing how the kit works since I had already done several tests using blood samples and I already knew my status. The results came out negative and I was convinced that when the instructions are followed, the kit works properly. I liked the experience because it was painless since there was no needles involved,” he narrates.
Who is this for?
According to Dr Geoffrey Taasi, a project officer HTS in the Ministry of Health, this self-test was initially targeting young people between 18 to 24 years who might be too shy to go to testing points.
Partners of lactating mothers who visit hospitals were also targeted.
The test kits are passed on to there partners through them. There are also female sex workers. This is done with the help of peer distribution who distribute the test kits to sex workers and teach them how to use them.
Application
An OraQuick self-testing kit comes with a test device (buffer) and a test tube in two different pouches.
A buffer is placed into the mouth, so that the flat pad is between the cheek and the outer gums, then swabbed across the outer gum line
HIV antibodies from oral fluid are collected through the swab. Once the device is inserted in to the test tube, the oral fluid mixes with the liquid in the test tube and travels up the test stick. The test stick has letters C and T. If the C-Line turns dark, it confirms the test is working properly. If the C-Line does not appear, the test is not working,’’ explains Brian Reid, the vice president of Orasure technologies.
If after 20 minutes only C-Line appears, it means the test is negative. A complete line next to the letter T means that the result is positive, regardless of whether the line is faint or concentrated.
Reid adds that if the test is positive, one may need a second test to confirm your test result. Seeing a healthcare provider to obtain a follow up test would be a great idea in this case.
“After reading the test result, the kit can be disposed of since it works only once.” Reid adds.
How it works
OraQuick works by detecting and collecting antibodies which are the body’s natural defenders against infection.
These antibodies are also found in the saliva in the mouth just as they are found in the blood itself. These anti bodies happen when the body is already facing the HIV virus and the body needs them to fight against it.
This is why it will show negative when you do not have the HIV virus because those antibodies will not be present.
This self-testing kit also works in a time frame of three months from a risk event or a sexual intercourse. This is because if you have recently been exposed to HIV virus, the antibodies may not have been formed yet.
One might wonder if HIV can be transmitted through saliva. The answer is no. OraQuick HIV self-test simply detects antibodies (which are found in the saliva and cannot spread the virus) for HIV and not the virus itself.
False positives/negatives
According to Dr Wilson Nakeba from Uganda Care at Naguru National Referral Hospital, every good thing always comes with some cons.
“The test detects antibodies in the oral fluids. Sometimes it might even be another infection and not HIV. This can cause unnecessary panic will automatically be a negative effect,” he points out
Other causes of misdisgnosis include;
• When the instructions provided for the use of the kits are not followed properly, a misdiagnosis can happen.
•Not waiting 15 minutes after eating or drinking, not waiting for 30 minutes after using oral care products before taking the tests can also lead to misdiagnosis.
•Swiping each gum more than once during oral collection also can also give a false test result.
•When having an HIV vaccine, one is not advisable to use the kit because it will not give you genuine results.
•Also, removing the buffer rom the test tube earlier than 29 minutes or later than 40 minutes may give you manipulated results.
Pre/post testing counselling
Apart from misdiagnosis, there is the disadvantage of lack of pre testing counselling as is the case when one goes to a testing unit.
“Finding out that you are positive on your own can be destructive. Cases of suicide may end up occurring,” Nakeba points out.
Dr Diana Atwiine, the permanent secretary ministry of Health urges the private sector to work with assistant commissioner of police to find a mechanism to strengthen the linkage between the end users of these kits and a healthcare officers who will be there all the time to speak to their clients.
“Every person who is going to sell these test kits must work with someone or organisation who are available 24/7 to pick a phone and provide counselling and assistance.
Cost
OraQuick test kits in the public facilities or government health centres are distributed free of charge . However, according victor Terakola, a business development manager at Orasure technologies, the ones offered by the private sector are up for sale. At wholesale price, the kits go for about Shs 23,000. The retail price for the kits however range from Shs25,000 to Shs30,000 depending on the pharmacy one has gone to.
Reliabilty
In research studies, the OraQuick test is as accurate (99.9% of the time) at identifying HIV-negative results as blood-based testing done in a lab by trained professionals.5 OraQuick is 91.7 per cent accurate at identifying HIV-positive test results. This means that almost 10 per cent of people who are HIV positive may be incorrectly identified as HIV negative using the OraQuick test. Oraquick is not as accurate as blood-based testing in a lab, which has been shown to be 99.7 per cent accurate at identifying positive test results.
False-negative results – when the test comes back negative but a person is actually HIV positive – can occur with OraQuick if a risk event (unprotected sex or borrowing injection equipment, for example) occurs within the three-month window period (as with the standard blood HIV antibody test).
This happens because the test relies on the detection of antibodies in the saliva, which may take up to three months to develop. Clients considering self-testing need to be counselled about the window period.
False-negative results may also occur if the user does not swab the gum line; or is wearing a dental product, such as dentures that cover their gums.
Compiled from www.catie.ca/en/pif/spring-20




