INVESTIGATION: High hospital bills cost mother her premature baby

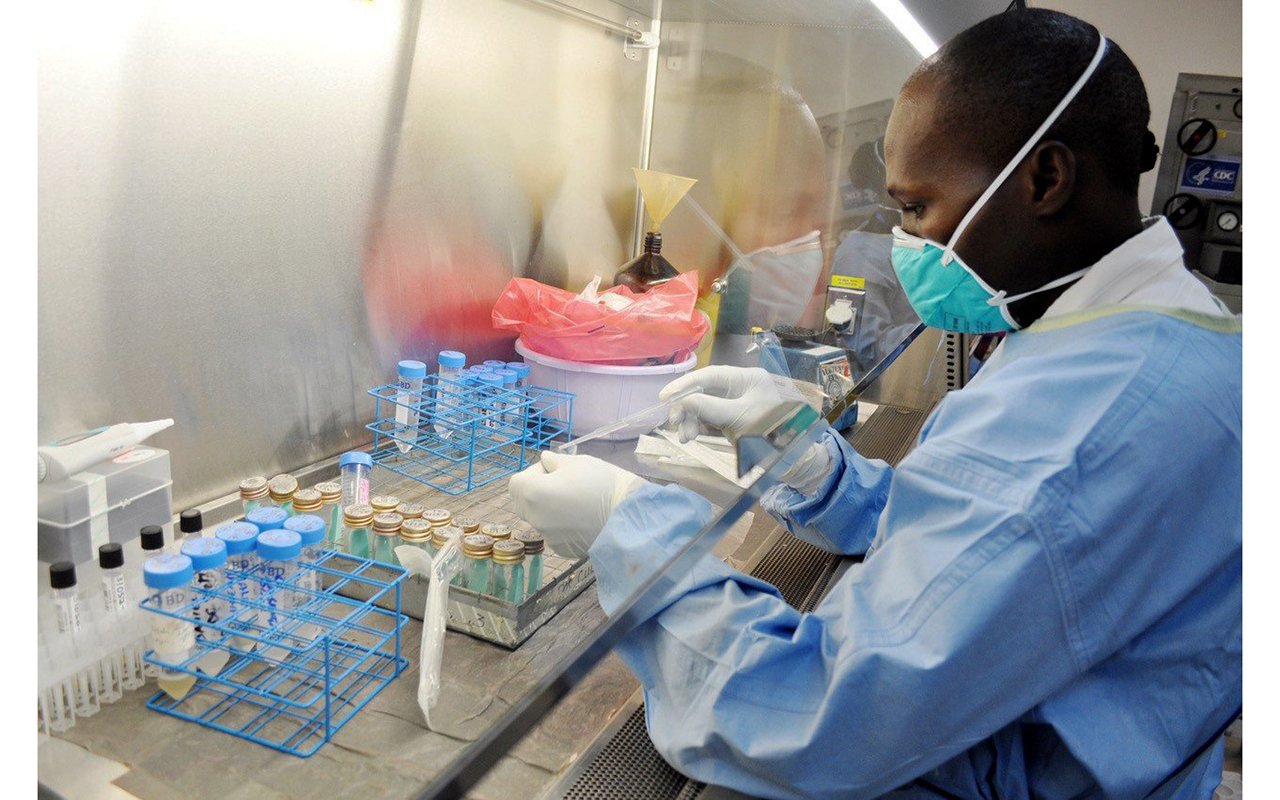
Monitoring. Premature babies receive specialised care at Kiruddu Hospital in Kampala. Services for premature babies are normally inadequate in public hospitals, forcing mothers to go to the expensive private facilities. PHOTO BY ERIC DOMINIC BUKENYA
What you need to know:
Experience. Ms Jane Atukunda lived a normal life until she conceived and gave birth to a premature baby five months after. Today, he is a healthy five-year-old boy. Five years later, Ms Atukunda had another preterm birth. During treatment at a private hospital, she accumulated a Shs35 million bill. But when she failed to pay, the administrators of a hospital, whose identity we cannot reveal, asked her to stake a land title or car logbook as collateral. When she failed to pay, she was expelled with her fragile baby. Atukunda says on the day she left hospital, her baby Alleluia, who had been taken off oxygen, began to writhe in the throes of death, writes Francis Jjingo.
Ms Jane Atukunda, 30, is a resident of Kibuli, Makindye Division, in Kampala. On January 7, Ms Atukunda received early birth pangs. This evoked consternation, anguish and pain as she had a history of giving birth to a premature baby.
Yet her past experience barely prepared her for the travails she was to encounter. Her gynaecologist in a private hospital, who declined to speak to us, later informed her that she needed close monitoring.
Ms Atukunda, who had fibroids, was supposed to have given birth by caesarean section. A fibroid is a benign tumour of muscular and fibrous tissues, typically developing in the wall of the uterus.
“Just when I was going to be operated, I pushed the baby and the doctor was like ‘what you have done is not good, however, it has saved us’,” Ms Atukunda narrates.
When the news of giving birth to another premature started trickling in among family and friends, it did not evoke empathy but ridicule and abuse. Others scornfully said this was a bad omen, reveals Ms Atukunda.
“My sister in-law said I had bad luck and that is why I delivered only premature babies. She said her brother shouldn’t have married me,” she recalls.
Ms Atukunda began experiencing pain. To treat her, medical workers prescribed drugs she could not afford.
“They told us that the bill in intensive care unit [ICU] could be high,” she says.
Because of the agony and stress Ms Ankunda was going through, she did not have enough breast milk for her baby and she was advised to find a donor.
“She called me, asking to get her a donor,” says Ms Juliet Nyandagala, Ms Atukunda’s sister,
“I wondered how this was possible because it had never crossed my mind that someone could donate her breast milk to someone else,” says Ms Nyandagala. Ms Atukunda says her sister introduced her to one Alice Nabukalu, who began providing breast milk.
Ms Atukunda says Ms Nabukalu from then became a donor and was required to go to hospital everyday to provide breast milk.
Two weeks after giving birth to the seven-month premature baby girl, the hospital bill had accumulated to Shs19 million yet Ms Atukunda only earned a paltry Shs400,000 a month.
“They told us to deposit some money so that the baby’s medication could go on. They told us to always check our bill every day. My husband would get the bill and hide it. ‘You don’t want to know what is here’, my husband always told me. The next time he told me to go and pick it myself and it was Shs24 million,” she says.
As the hospital bill increased, she demanded to be referred to an affordable government hospital.
Ms Atukunda reveals that the Health minister, Dr Ruth Aceng, told her to seek a referral from the private hospital so that she could have her baby admitted to Mulago hospital.
“The minister told me that she would ensure that I am not charged any money at Mulago hospital. She told me that they should not even ask for a penny,” she says.
However, the private hospital promised to write the referral only after she had paid the bill that had accumulated to Shs35 million.

My story. Ms Atukunda, who lost her premature baby after failing to pay bills
After Ms Atukunda was discharged, she would often sneak into the hospital to check on her baby whose life precariously hang upon the support of the medical facilitates and expertise.
“I was scared. The most traumatising moment is when I would sneak into the hospital to check on my baby,” she says.
“I think they had people to inform them that I had arrived. Then they would tell me, ‘You need to settle these bills, we are working on your baby but you are not paying anything. Can you deposit some money please?” she adds.
Ms Atukunda says even when Mulago women’s hospital was ready to receive her baby, the private hospital administrators insisted that she paid some money or use her land title as collateral to clear the balance of Shs27.8 million.
“They said I had to deposit some money or a land title or a car logbook so as to be given referral. I told them I had only 2m shillings. They asked me if I had any land title from my relatives. They said I could talk to them and at least give them something tangible,” she adds.
When some well-wishers learnt of Ms Atukunda’s plight, they raised part of the money owed to the hospital.
“They would raise Shs10,000, Shs20,000, Shs30,000. I remember I collected the money and it amounted to around Shhs1.6 million shillings. Sometimes they [billers] would ask for cash to pay part-time doctors,” she recalls.
Ms Atukunda says her impassioned pleas fell on deaf ears as she was told to leave with the baby.
On March 4, she was told to take her baby home after she was taken off oxygen. Ms Atukunda was briefly detained and upon paying Shs2m, she was freed. She signed an agreement, promising to pay the balance of Shs27.8m at a future date. The following night, she left with Baby Alleluia. “My Son Joram, who was also born a premature, did not know that I had brought Baby Alleluia because we returned during the night. He is actually the one who named him Baby Alleluia,” says Ms Atukunda.
“At 4am, I checked on the baby. I woke up, opened the fridge and picked the breast milk to warm it. I realised the baby was not crying yet babies always cry when its time for feeding. When I lifted the baby it was heavy. I did not know that the baby had died,” she says as her voice betrays her emotions.
Even before the solemn dirge could fade in the distant burial grounds where Alleluia was laid to rest, the hospital billers started reminding her to pay the debt.
Ms Atukunda had five years ago given birth to a premature baby boy.
“When I saw him placed in an incubator, I wanted to run away. But then I remembered my wounds are not healing first. But then after three weeks, Joram was already 1.5kgs. The nurses said my baby was feeding well. The next weight was 2.6kgs. I have photos of Joram; you can’t believe that he was a premature.
Today Joram is a promising five-year-old boy. He is so bright in class that his teachers are very proud of him,” she says.
Ms Atukunda avoided self-pity. She joined a group of well-wishers who had provided her with some money. “Even when my child passed on, I would still go to Kawempe Hospital and visit mothers and take them baby diapers. I would see other babies die.”
She hopes to become a change agent. “I am willing to work with Mama Tulia [a Good Samaritan], who has devoted her life helping these mothers.”

Charges. A copy of the hospital bill that was Ms Atukunda had to pay at a private hospital in Kampala. courtesy photo
A senior paediatrician at Mulago hospital, Dr Sabrina Kitaka, explains conditions that could lead to a preterm birth. “There is placental insufficiency and so, not enough oxygen is getting into the placenta and it can easily detach and that can cause recurrent prematurity. But there also infections such as malaria, HIV/Aids, Hepatitis B and also chromosomal abnormalities. If the baby has mutation or chromosomal abnormalities, the body can reject the baby,” she explains.
Dr Kitaka says treatment to preserve the lives of premature babies is expensive. “These babies suffer from micro nutrient deficiencies, low calcium levels. They need to be monitored in an intensive care unit, which is functional,” she adds.
Experts speak out
Premature babies have an incompetent immune system and are prone to infections, and hypothermia kills these babies, says Dr Kitaka.
“Our infant mortality rate has dropped from 62 out of 1,000 births to 41 out of 1,000 births, which is good. However, 40 per cent of the infant mortality cases is as a result of preterm deaths” she says.
Dr Kitaka says premature babies can survive and be responsible people. “I know doctors, engineers, teachers and journalists who were once preterm,” she says.
The State minister for Health in-charge of General Duties, Ms Sarah Opendi, says statistics have been stagnant at 27 premature births for 1,000 births in the last three years. Ms Opendi says preterm deaths can be prevented if mothers give birth in the hands of specialised health care professionals.
“Why should you go to a health facility when you know you do not have the money? Please use our government health facilities. I want to encourage mothers to go for antenatal; we have now recommended [antenatal check-up] eight times instead of four,” she said.
However, Minister Opendi says the costs at Mulago specialised hospital are still high.
“Ordinary Ugandans can’t afford. As a ministry, we are reviewing the rates downwards.”
Nsambya Hospital is also developing a breast milk bank to help premature babies survive. But some of these services at well-equipped hospitals are out of reach for ordinary Ugandans, leaving access to proper medical care exclusively for the rich and privileged.
Statistics on premature births
The State minister for Health in-charge of General Duties, Ms Sarah Opendi, says statistics have been stagnant at 27 premature births for 1,000 births in the last three years. Ms Opendi says preterm deaths can be prevented if mothers give birth in the hands of specialised health care professionals.