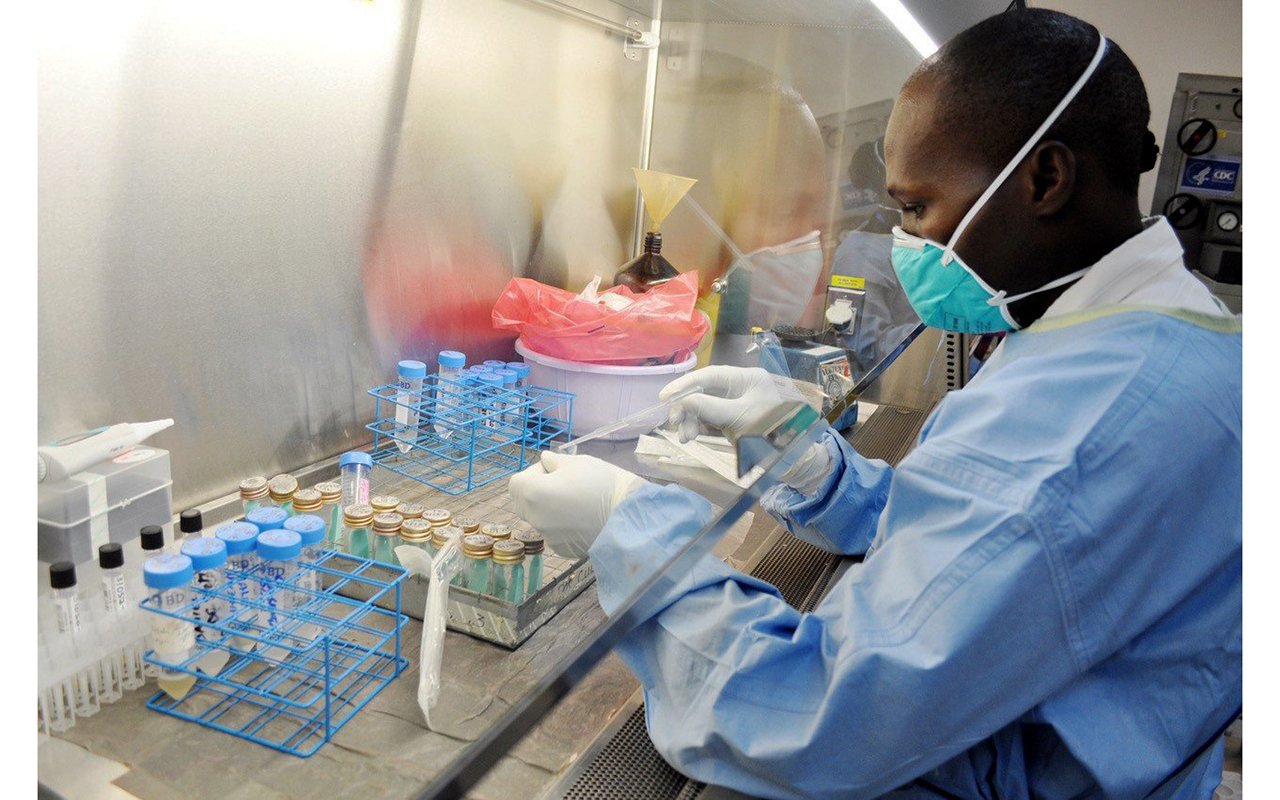
How legal is your medical outlet?

Pharmacy. An attendant looks for medicine at one of the pharmacies in Kampala in May last year. MONITOR PHOTO
What you need to know:
Drug abuse. Class A and much of Class B drugs are not supposed to be dispensed across the counter in pharmacies without prescription, mainly because they stand a possibility of being abused. However, investigations carried out by our reporter show this is not the case.
Quite often, cases of self-medication gone bad have been blamed on the crumbling health system and not the victim.
Access to medicine is easy for anyone who has money since most pharmacies are in the hands of the private sector. Government pharmacies can only be accessed through government hospitals but they are most often not well stocked, leaving the bigger sector to individuals.
There are rules and regulations governing the dispensing of medicine at both the private and government run pharmacies.
Though pharmacies within government hospitals are required to oblige, the private profit oriented pharmacies are registered and supervised by the National Drug Authority (NDA) to ensure all is followed.
The same government agency inspects and approves all types of medicine, be it human or veterinary in the country. All human medicine brought into the country is classified into three categories. “Class ‘A’ class B ‘one’ and B ‘two’ and Class C.
Most of Class A drugs are narcotics and their importation and storage while in the country is tightly monitored, some require special permits and are controlled by an international body which has to approve the importation permit.
“Some drugs in Class A such as codeine require a special permit from NDA, it’s also approved by the International Narcotic Council Board (INCB) which keeps record of the narcotic drugs imported by different countries,” says the authority’s director of enforcement and Inspectorate, Mr David Nahamya.
Class A and much of Class B drugs are not supposed to be dispensed across the counter in pharmacies without prescription, mainly because they stand a possibility of being abused. However, investigations carried out by this paper shows this is not the case.
No pharmacists
Many of the pharmacies Daily Monitor visited did not have a pharmacist present as is required. The attendants have different reasons why the pharmacist was away ranging from having gone for a meeting; he comes in the evening; is on leave; she
is at the head office – as one attendant in a pharmacy with a chain of outlets around the city centre and its suburbs says.
In one incident at a pharmacy in Nsambya, a stone’s throw away from Nsambya hospital, after insisting to see the pharmacist other than the attendant, I walk away only to be followed by a gentleman of Asian origin saying: “My friend first come let’s talk, I can help you. The pharmacist went for prayers,” he says.
The attendant says the pharmacist has gone for a meeting in town.
According to the secretary of Pharmaceutical Society of Uganda (PSU), Mr Samuel Opio, there are a number of reasons why pharmacists are not always in the pharmacies.
“Due to the limited numbers, each pharmacist supervises two pharmacies a day divided into five hours each. Currently there are 1,053 registered pharmacists, with 150 new entrants a year compared to 15 back in 2006,” he says.
However, the 1,053 pharmacists are shared between government, the private sector, those that have gone abroad for greener pastures and others have branched off into private businesses.
Besides their limited numbers some of them registered to supervise private pharmacies are faced with a hostile work environment.
Liberalised economy
Mr Opio says unlike countries such as Kenya, Tanzania, Rwanda and other European countries where the pharmacy business is restricted to pharmacists only, in Uganda anyone with money can open a pharmacy and hire a pharmacist to supervise its day-to-day activities.
“There are cases where pharmacists have come complaining they have been told to go home and wait for their salary at the end of the month but not come to work. Their presence is considered a threat to the profits of the business,” he says.
In their absence, the law requires trained pharmacy auxiliary staff to fill the gap. In most cases, these are supposed to be nurses. But in many cases people with no medical background are employed.
Though it is very easy to buy prescription drugs only without prescription in many of the pharmacies visited, there are those that are very strict. And this is common in places where the pharmacist is present.
In a pharmacy on Dewinton Road, I ask to buy Morphine but the pharmacist insists on a medical report. Despite all the pleading, he refuses to dispense it.
The same happens in Wangedeya when I try to buy Codeine tablets, though I am able to get them across the counter in Nakulabye. In another pharmacy in Wandegeya, I am able to get valium, though I fail to get Tramadol in the same location but I get it on William Street.
One pharmacy in Ntinda is willing to sell Tramadol but not in small quantities I am asking for despite not having prescription.
Both PSU and NDA admit that there is a big problem with classified medicine being sold across the counter but the pharmaceutical society blames patients’ behaviour and the environment the pharmacists operate.
“I must admit that we have a problem of prescription drugs being administered across the counter without prescription. As pharmacists, we are often presented with fake prescription written by unqualified personnel,” he says.
For instance, in 2011 the Ministry of Health closed 70 per cent of the clinics in Kampala for operating illegally or employing unqualified personnel.
“Pharmacies are supposed to receive valid prescriptions from registered healthy facilities with qualified practitioners. But many times patients present prescriptions from unregistered illegal health facilities. Such prescriptions are invalid and they can’t be honoured. But then you see a patient is in pain, by law we are allowed to provide first treatment,” Mr Opio says.
He adds that as PSU, they are not the registering and supervising authority for pharmacies.
“We are responsible for the pharmacists, but not the pharmacy. Our biggest challenge as PSU is that we have a legal framework which somehow makes it impossible to implement certain professional requirements in the pharmacy profession. There is need for urgent intervention in order to solve this problem,” he says.
A case of codeine
Many of the cough syrups sold across the country do contain substance called codeine which is a narcotic. Codeine is a cough suppressant but if not well used it can become addictive. The drug authority says codeine is not yet a threat in the country but they will not hesitate to act if it gets abused.
“We have a mandate, if we find that people are not using the syrup in the right way we can uplift it to another class for it not to be accessed without prescription in order to save the situation. But in doing so we have to balance between denying the masses access to medication and denying those using it as a substance to abuse,” Mr Nahamya says.
Cough syrups with codeine manufactured in Uganda have to import codeine as a raw material. As a legalised but restricted narcotic, Uganda has a quota from the INCB.
Without giving numbers, Mr Opio says as the registering and supervising authority for the pharmacist, they have gone ahead to penalise registered members who flout the rules of conduct.
“If one is found not complying with the code of conduct action depending on the severity of the negligence is taken. We have received some complaints; the problem is that the public is silent on such cases but where the public has come out to point out lapses in the pharmaceutical sector we have taken action,” he says.
LEGALITY
How to tell an authorised pharmacy
By law, a legalised pharmacy must have the following displayed in the view of its customers.
- Certificate of registration.
- Certificate of suitability of premises.
- Practicing certificate of the supervising pharmacists.
- Trading license.
In 2011 the Ministry of Health closed 70 per cent of the clinics in Kampala for operating illegally or employing unqualified personnel.
The Pharmaceutical Society of Uganda say they are responsible for the pharmacists but not the pharmacy.