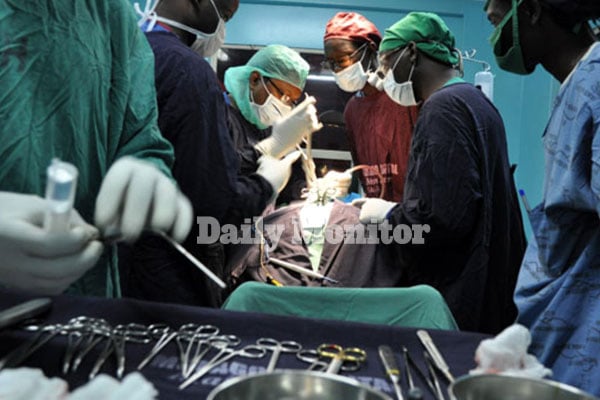
Money motivating doctors to do more C-sections – report
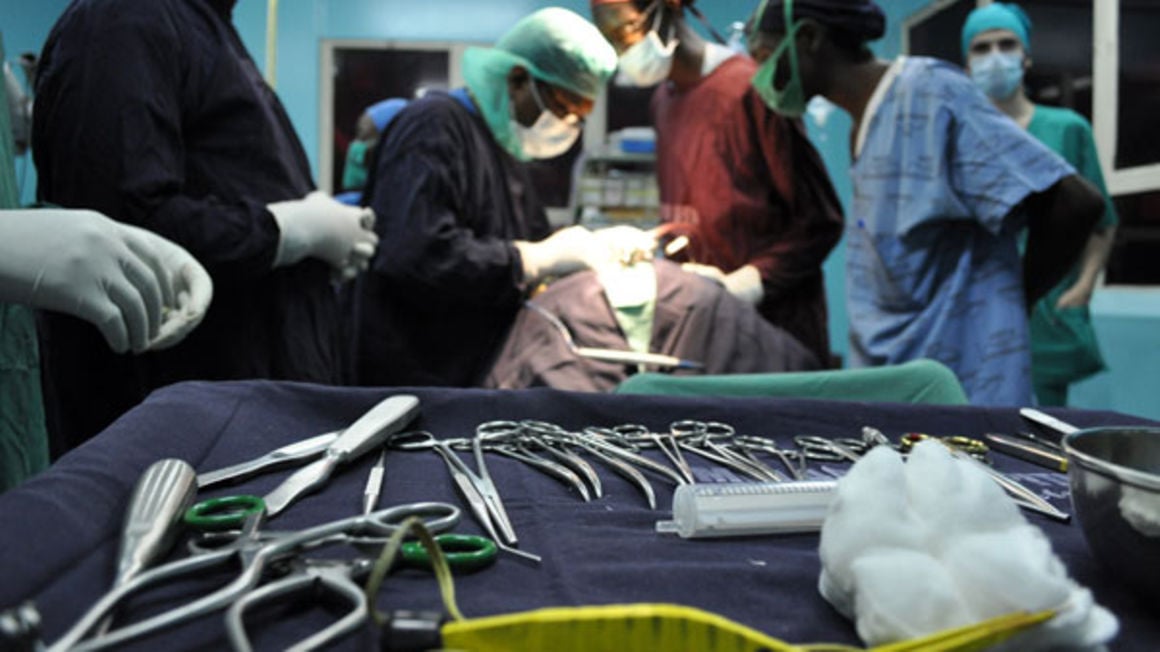
Doctors carry out surgery on a patient recently.Hospitals have registered an increasing number of mothers seeking to undergo caesarean sections rather than normal delivery.photo/file.
What you need to know:
- Medical experts say although caesarean section saves lives, it also poses health risks to a mother and the baby, in addition to increased financial burden due to longer stay in hospital and hefty charges for a C-section.
Many Ugandan doctors are violating ethics to induce demand for caesarean section (C-section) among expectant mothers for monetary gain despite the health risks the procedure presents, a new research report by a Makerere University lecturer indicates.
As high as 98,000 of 1.4 million babies born in Uganda annually are now being delivered through caesarean section, according to government statistics. This represents about seven per cent, which is a sharp increase when compared with 1995 statistics where C-section births accounted for only 2.5 percent of the country’s births.
C-section, a surgical procedure used to deliver a baby through incisions in the abdomen and uterus, is recommended when the safety of the mother or baby is compromised due to pregnancy or labour complications, according to experts.
Medical experts say although caesarean section saves lives, it also poses health risks to a mother and the baby, in addition to increased financial burden due to longer stay in hospital and hefty charges for a C-section, which stands at about Shs1.6 million and beyond in high-end private hospitals.
Natural birth costs just under Shs800,000 in most health facilities, according to doctors.
A copy of the research report titled ‘Physician-induced demand for caesarean section,’ which this newspaper has accessed, indicates that delivery at a private health facility increases the probability of caesarean births.
“This is indicative of physician-induced demand,” the report authored by Dr John Bosco Oryema, an Economics lecturer at the School of Economics, Makerere University, reads in part. He adds that “the finding implies there is need for closer monitoring of private hospitals as well as protection of patients from avoidable procedures.”
“….if the birth takes place at a private health facility, rather than at a government hospital, the probability of CS [C-section] increases by 6.1 percent,” he writes.
Referring to other studies, Dr Oryema said induced demand for caesarean section is feasible “if the cost of CS [C-section] is equivalent to the perceived benefit from expectant mothers’ perspective.” He adds that Microeconomic model prediction shows that physicians in private practice might induce demand for some services in order to meet the profit objective of the hospital.
Dr Oryema says the findings were based on analysis of the 2011 Uganda Demographic and Health Survey (UDHS) dataset, which indicate there has been a significant rise in caesarean births from 2.6 percent in 1995 to 5.1 percent in 2011.
The research was part of Dr Oryema’s PhD (Economics) research thesis, which he completed in 2016 from the University of South Florida, USA.
Another study published in 2019 by Emily Atuheire from Ministry of Health’s Reproductive Health Division on the trend of C-section births between 2012 and 2016 in 3,461 health facilities across the country, also indicated that the rate had increased from 8.5 percent in 2012 to 11 percent in 2016. The report projected the rate of caesarean section to increase by a record-high 36 percent this year 2021.
Ms Harriet Acham, a resident of Kampala, said a doctor in one of the private health facilities tried to induce her daughter into C-section.
“The doctor told my daughter Ritah that it was a matter of life and death for her to deliver by caesarean section because the scan showed that the baby had the code entangled around the neck [and wouldn’t be delivered naturally],” she said.
“Luckily, she [my daughter] told the doctor to talk to me first. From the tone of his voice I knew it was a money issue, so I advised her to get away very fast with the scan [results] and get a second opinion from a government hospital. She is now a mother of a bouncing baby girl born normally [naturally],” she added.
But another woman from Mityana, who identified herself as Ms Phibby Kaka, said women should embrace C-section to minimise death of their children. She said she lost her baby in 2019 due to fetal distress for trying too hard to give birth the natural way.
“Fetal distress is real. If I was strong enough to make that decision early enough [to go for caesarean section], my baby would be one-and-half years now, but she is with the angels,” she said. Fetal distress is a pregnancy and labour complication where a baby experiences oxygen deprivation either due to abnormal presentation or prolonged labour.
Death rate among children in Uganda is still very high at 21 for every 1,000 births while maternal mortality rate is 343 per 100,000 live births, according to statistics from United Nation’s Children Fund (Unicef).
But a number of women, including Shakira Ainembabazi, another Kampala resident, believes that C-section helps them keep their lady parts in good shape, to optimise carnal pleasures with their spouses. Several others also say caesarean section saves them from disorienting labour pain.
Available scientific information says C-section reduces the risk of pain during birth, injury to the lady parts and loss of bladder control.
Experts speak
Dr Mukuzi Muhereza, the secretary general for Uganda Medical Association (UMA), admitted that there are caesarean births that are happening in the country for monetary gains by hospitals. He asked the Ministry of Health to conduct a special audit into C-section births in the country.
“Ideally, in 100 [expectant] mothers, you will get a range of 5 to 15 who will be assisted [to deliver]. Assisted means we use forceps, vacuum or C-section. But some private hospitals [in Kampala] have up to about 80 percent of the deliveries being caesarean, which is higher than the maximum [tolerated limit] of 15 percent,” he said. The 2018/2019 Health Sector Review Report confirms this.
“It could be a pre-selection that mothers with complications often go to the said facility for safe delivery or it is motivated by the need to get more money because clients pay more for assisted delivery through caesarean section,” he said.
Dr Mukuzi added: “We don’t want our mothers cut. For us, as the association, we can always talk to our colleagues to get back to the basics.”
Like Dr Mukuzi, Dr Simon Peter Eyoku, another doctor at Mulago Hospital, also said the quest to make more money could be forcing hospitals to induce demand for C-section, which increases return on investment.
“There are so many reasons for rising caesarean births in the country and money could be one of them, but others like prevention of mother-to-child transmission of HIV could also be one of the reasons why people are going for C-section,” he said.
“I can’t stand here and condemn my colleagues [the doctors for inducing demand for C-section] because they could be making up for the little money they are being paid in this country. They are finding a way of topping up,” he said.
Doctors have perpetually demanded that government should increase their salary.
Mr Brian Mukalazi, the head of Every Child Ministries Uganda, a civil society organisation, said some women in labour are opting for C-section “because they feel humiliated by health workers” who criticise and make fun of the mothers for their cries of pain during labour.
He reasoned that doctors and hospitals prefer C-section because it is time-saving and highly rewarding.
“In addition to being paid more money for a caesarean birth, obstetricians [doctors] generally require a shorter time period to perform it as compared to a normal delivery. Performing a C-section could require maybe an hour or two of work while delivering babies naturally might involve intermittent work spanning over a 24-hour period,” he said.

Mothers at a health facility
But Dr Livingstone Makanga, the assistant commissioner in-charge of reproductive and infant health at the Ministry of Health, when asked about the vice [doctors inducing demand for C-section] yesterday, told this newspaper there no need for alarm because C-section in the country is being done after medical evaluation.
“Caesarean section is done after a medical indication. There are medical conditions that warrant C-section. So if a provider assess a client and sees the need, then he [or she] will do it,” he said, adding that the ministry has standards that must be followed when doing caesarean section for the benefit of both the mother and the baby.
Rich people prefer C-section
Dr Denis Kimalyo, the head of Uganda National Association of Private Hospitals, said there is an increase in the number of deliveries through C-section but that there is no proof that monetary gain by the facilities is the driving factor.
“We also have to look at the type of clients who come to private facilities versus public facilities. A number of women don’t want to push [have normal delivery without C-section],” he said.
According to 2016 UDHS, C-section births are higher among the wealthy with 16 percent of the rich opting for C-section compared to only 3 percent of the poorest. The wealthy are more likely to go to private health facilities while the poor often go to government hospitals for cost reasons.
C-section reduces the risk of pain during birth, injury to the vagina and loss of bladder control, according to available scientific information. Majority of caesarean births in the country is in Kampala (14 percent), according to the UDHS, which is higher than the national average of 7 percent. C-section in urban areas stands at 13 percent while in rural areas it stands at 5 percent.
The UDHS also indicate that 33 percent of women decided to go for C-section before labour had started while 67 made the decision to go for C-section after labour had started.
About c-section
When is CS necessary?
As opposed to going for C-section for lifestyle reasons, experts say caesarean section can be done when there are complications during pregnancy or delivery of the baby.
Dr Mukuzi Muhereza, the secretary general for Uganda Medical Association (UMA), said C-section can be done when there is baby fatigue, a situation where a woman’s labour is not progressing, either too slow or stops. “If there is fetal distress, then we have to remove the baby [through C-section]. Also [C-section is done] if the mother has complications such as hypertension, contracted pelvis or not breathing well,” he added.
READ MORE
Dr Simon Peter Eyoku, a doctor at Mulago Hospital, said that beside preventing mother-to-child transmission of HIV, C-section can also be done when the baby is very large or when a woman has had a caesarean delivery in the past or other surgeries on the uterus or womb.
A number of teenage girls who are getting pregnant in the country are also delivering babies through C-section because of narrow pelvis, according to some experts.
Dangers of C-section to mother and baby
Dr Mukuzi said C-section is generally safe as long as it is done well by a doctor, “unless it is an accidental cutting.”
“I have seen some fracture as you bring out the baby; fracture of the upper hand, but is a small incident,” he said.
Available scientific information indicates that C-section increase risk of womb or wound infection due to the incision, longer stay in hospital after birth and taking long to recover from the birth, blood clots and future pregnancy complications.
The risk to the baby may include cut to the skin during surgery or breathing difficulty for a baby delivered through C-section preterm.
Dr Eyoku said the more C-section a woman has, the greater the risk of future birth or pregnancy complications.
Mr Brian Mukalazi, the head of Every Child Ministries Uganda, said: “In effort to avert this escalating problem of caesarean births, pregnant women should be advised on the effective management of their health while emphasising the risk of C-section births and benefits of natural labour. In turn, incentives or allowances for medical personnel should be raised for successful natural births handled and with extra supervision.”