123 die daily as quality of healthcare declines
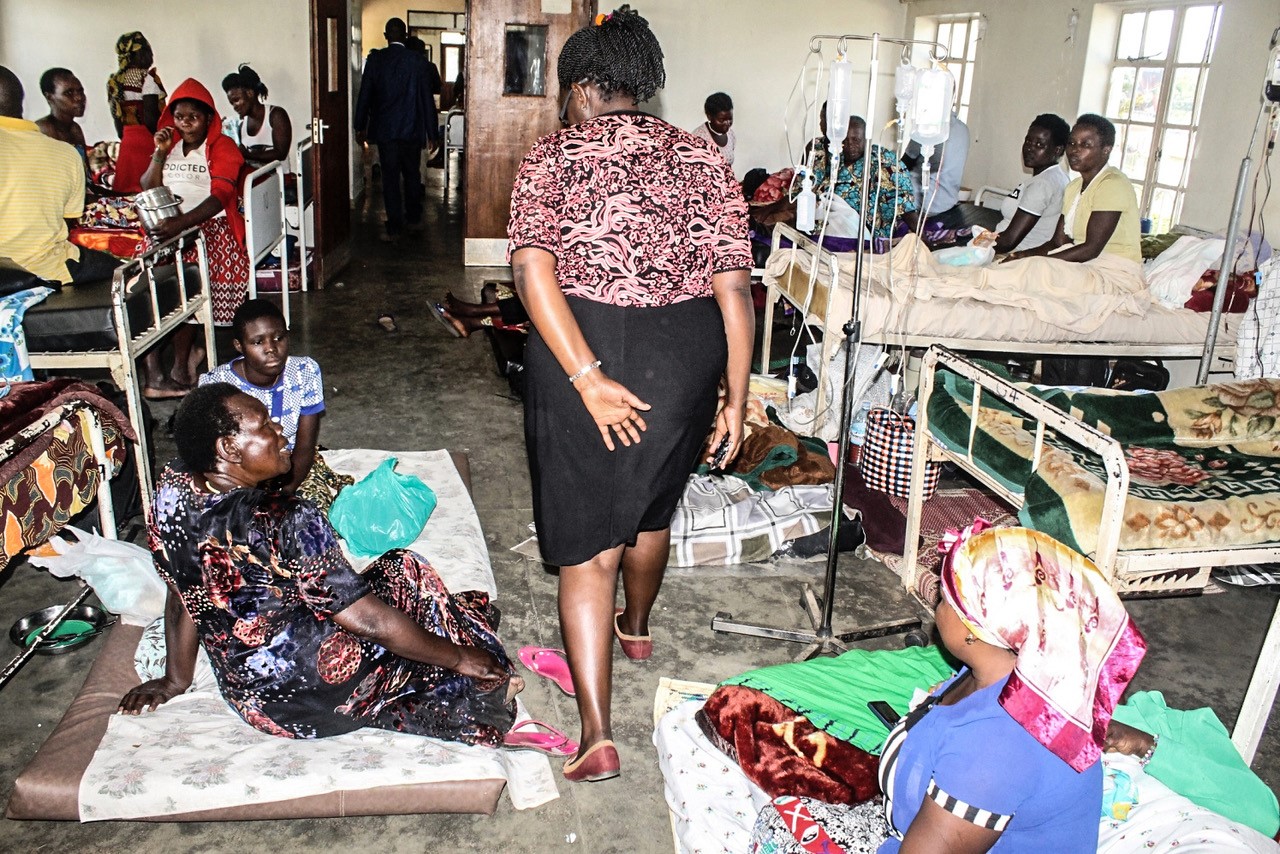
A congested Patient ward at Fort Portal Regional Referral Hospital in 2019. PHOTO | FILE
What you need to know:
- Change. Improvements in performance were made possible by the commitment of health providers and workers in the public and private sector, working under sometimes difficult conditions, especially in the hard-to-reach districts in the country,” Dr Ruth Aceng, Health minister.
- Way-forward. ‘‘In case of premature births, let’s ensure that we provide the right care, at the right time in the right place including referrals of premature, small and sick newborns from communities and lower health facilities,” Dr Charles Olaro, the director of the curative services at the Ministry.
A new report has indicated a significant decline in the quality of healthcare and shortage of essential medicines in hospitals amid the rising burden of diseases.
The 2019/2020 Annual Health Sector Performance Report highlights glaring shortfalls in quality of care, which reflects through the rising deaths in hospitals and other health facilities .
According to the Ministry of Health report, the country registered 45,042 deaths in hospitals in the 2019/2020 Financial Year. This translates to 123 deaths occurring daily.
The reported number is, however, 13 per cent higher than the 34,491 deaths that were reported in the 2018/2019 Financial Year.
Among those aged five years and above, 23,059 died and 21,983 deaths occurred among children below five years.
The deaths were higher among males with 11,764 dying compared to 10,219 females aged five years and above. Among those under five years, it was 13,302 males and 9,757 females.
Killer diseases
“The leading causes of death among all ages were malaria (13.3 per cent), pneumonia (7.4 per cent), anaemia (6.2 per cent), other neonatal conditions (5.1 per cent) and premature baby (3.7 per cent),” the report reads.
In the report, hypertension killed 1,197 people, motorcycle and road traffic accidents killed 775 people whereas injuries from other causes killed 1,022.
“The rate of under-five deaths among 1,000 under-five admissions increased by 4 per cent to 24 per 1,000 admissions compared to 23 per in 2018/2019,” the report further read. The Health Sector Development Plan (HSDP) target of 16 per 1,000 was not achieved.
“Among children under five years, malaria is still the leading cause of death at 18.1 per cent, although neonatal conditions and premature baby combined contributed 18.2 per cent of all under-five deaths,” it reads further.
The report also indicated that 28,174 deaths of newborn babies occurred in the 2019/2020 Financial Year. However, there was a 20 per cent reduction in the number of perinatal deaths from 35,703 in 2015/2016 to 28,174 in 2019/2020 Financial Year.
According to the report, improving neonatal and prematurity care can significantly reduce under-five deaths in Uganda.
The country registered a 7.6 per cent increase in the number of maternal deaths, pushing the death rates to 99 per 100,000, above the 92 per 100,000 in the 2018/2019 Financial Year.
The HSDP for 2015 to 2020 had, however, set a target of reducing maternal deaths in the country to 98 per 100,000. In this regard, the comparison between deaths that were reported between 2015/2016 and 2019/2020, shows a general decline of 17 per cent due to improved access and quality of care. The new health sector performance report however, shows decline in access and quality of care for a period between FY 2018/2019 and FY 2019/2020.
A total of 1,192 maternal deaths were reported through the Ministry’s Health Management Information System (HMIS) compared to 1,083 in 2018/2019. A number of women, however, still deliver from home and maternal deaths in such settings are unreported.
The districts where the highest number of maternal deaths were reported include Kampala, Hoima, Masaka, Kabarole, Mbale, Mbarara, Gulu, Kamuli and Luweero.
The report indicates that majority of the deaths were reported in general hospitals, followed by regional referral hospitals and health centre IVs. The report also directs that strengthening the referral system as well as improving the emergency newborn and obstetric care services at the general hospitals and health centre IVs will reduce maternal deaths.
According to the report, the leading causes of maternal deaths included haemorrhage (42 per cent), infections, anaemia and HIV/Aids (12 per cent), and hypertension (8 per cent), among other complications.
Dr Sabrina Bakeera Kitaka, a paediatrician and lecturer at Makerere University College of Health Sciences, said preterm birth, a major factor in newborn deaths, is still a big challenge.
“As long as we don’t resolve the problem of prematurity, then we are unlikely to resolve the problem of neonatal deaths,” she said.
Dr Kitaka said preventing neonatal deaths starts with a woman knowing that she is pregnant and going for checkup in a recognised health facility. “WHO has recommended that women should go for at least eight antenatal checkups, starting from the time they missed their menstrual period. And if that doesn’t happen, many challenges can occur,” she said.
A 2019 study in Mubende Regional Referral Hospital found that 37 per cent of babies born but are not breathing at the hospital, were not resuscitated.
The report also indicated that care providers lacked sufficient knowledge and skills to initiate breathing and that there were inadequate availability of basic breathing aids for newborn resuscitation.
The equipment needed to resuscitate include penguin sucker, a suction bulb to remove mucus clogging in the infant’s nose and mouth, among others.
The ministry has only achieved five of the 42 HSDP targets. The report indicated that 51 per cent of the facilities did not have sufficient (95 per cent) of essential medicines and health supplies for handling patients.
“The percentage of health facilities having more than 95 per cent availability of key commodities dropped to 46 per cent in 2019/2020 from 53 per cent in 2018/2019,” the report reads. This is below the HSDP target of 75 per cent.
Up to 67 per cent of the facilities did not have adequate antiretroviral drugs (ARVs), 33 per cent had inadequate TB drugs, and 54 per cent lacked laboratory commodities for testing malaria and other diseases.
According to the report, the public health sector staffing level against the approved posts declined to 73 per cent (47,932/65,271) in 2019/2020 FY from 76 per cent in 2018/2019. This is below the HSDP target of 80 per cent.
“Overall, the stock of qualified health professionals available for employment in the health sector increased from 107,284 in FY 2018/2019 to 114,740 in FY 2019/2020. This is attributed to government commitment to attract and retain a competent health workforce in Uganda,” the report reads.
The report found that hospitals admissions reduced to 7.2 per 100 in 2019/2020 from 7.3 per 100 population in 2018/2019. The HSDP target was 10 per 100. According to the report, the admissions were most affected by the Covid-19 lockdown.
“The trends further show that whereas other services picked up after May 2020, the in-patient admissions are still much lower. This maybe because the community may not be comfortable to access the health facilities for fear of Covid-19 exposure or the disease burden requiring admission have significantly reduced,” the report reads.
Sanitation challenges
The Ministry reported significant gaps in sanitation across the country.
For the 3,060 health facilities that were assessed, 63.6 per cent had limited sanitation services. This increases the risks of hospital-acquired infections.
The facilities with sanitary facilities stand at 94.6 per cent as usable and 31 per cent had access to basic sanitation.
In schools, pupil to toilet ratio is 72:1 against the standard of 45:1 for day schools and 25:1 for boarding schools.
“Handwashing coverage in schools was at 57 per cent. Only 21 per cent of schools had facilities to cater for menstrual hygiene,” the report read.
Waste management in most facilities are equally poor. Only 44.2 per cent of health facilities had access to basic service for healthcare waste management.
“Health facilities in Karamoja, Bunyoro and Mt Elgon have the highest basic services for healthcare waste management at 76 per cent, 70 per cent and 64 per cent, respectively. Worst scores are reported in the sub-regions of Busoga and Kigezi,” the report read.
Achievements
“The sector realised an increase in the number of adults and children on anti-retroviral treatment and achieved 89 per cent coverage from 86 per cent,” the report indicated. This is 9 per cent above the HSDP target of 80 per cent.
The percentage of HIV positive pregnant women, who are receiving ARVs to prevent mother-to-child transmission of the virus, increased to 94 per cent (30,113/32,036) from 91 per cent (29,475/32,485) in 2018/2019.
“TB case detection rate increased by 5.1 per cent to 82 per cent in 2019/2020 from 78 per cent. TB treatment success rate increased by 8.3 per cent to 78 percent from 72 per cent in the previous financial year,” according to the report.
The report indicates that investments in health infrastructure has increased and this has allowed for construction of new and rehabilitation of old infrastructure at various levels, procurement and maintenance of medical equipment and hospital furniture across the country.
The infrastructure development projects during 2019/2020 were completion and commissioning of the regional hospital for paediatric surgery in Entebbe and rehabilitation and equipping of Kawolo and Kayunga hospitals.
Up to 124 health centre IIs were upgraded to health centre IIIs and works for upgrading of an additional 62 health centre IIs to health centre IIIs are ongoing.
Officials say
Even in the face of declining quality of health care, Dr Jane Ruth Aceng, the Health minister, said there was improvement in the performance of the sector.
She said the improvement was due to strong partnership and collaboration with the private sector and the community.
“This needs to be sustained for the sector to maintain its gains over the last five years,” Dr Aceng said.
Dr Charles Olaro, the director of the curative services at the Ministry, said they have set up a national newborn steering committee comprising health professionals and development partners to support implementation of high impact interventions.
Dr Olaro said by the end of 2019, the committee had supported the establishment of 19 neonatal care centres around the country.
The ministry has also set up a neonatal intensive care unit equipped with advanced newborn care machines at the Kawempe National Referral Hospital and another neonatal intensive care unit has been set up in Kamuli District.
“We also still have challenges of human resource to work in the newborn care units as majority of the facility managers hardly allocate specific staff to the department,” Dr Olaro said.
“In case of premature births, let’s ensure that we provide the right care, at the right time in the right place including referrals of premature, small and sick newborns from communities and lower health facilities,” she said




