Challenges of establishing strong health system
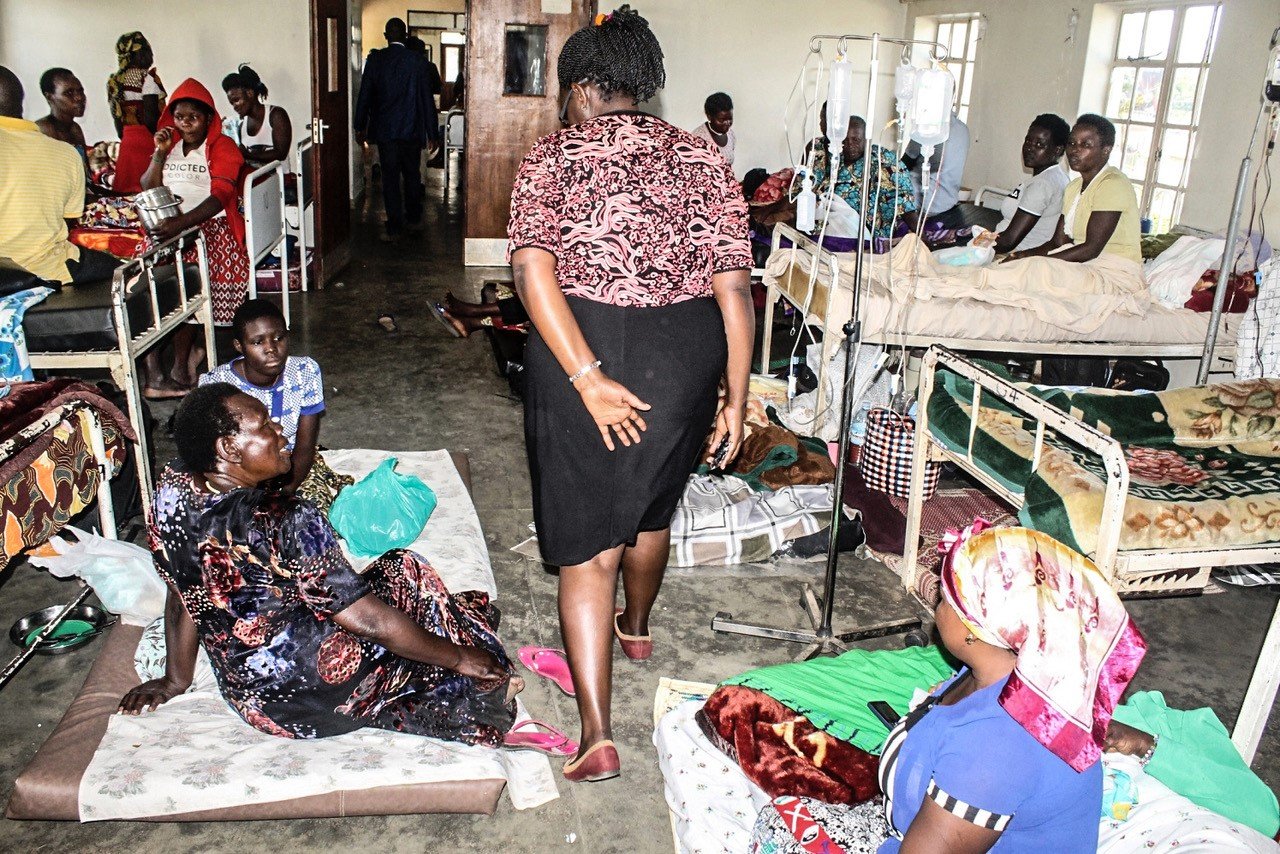
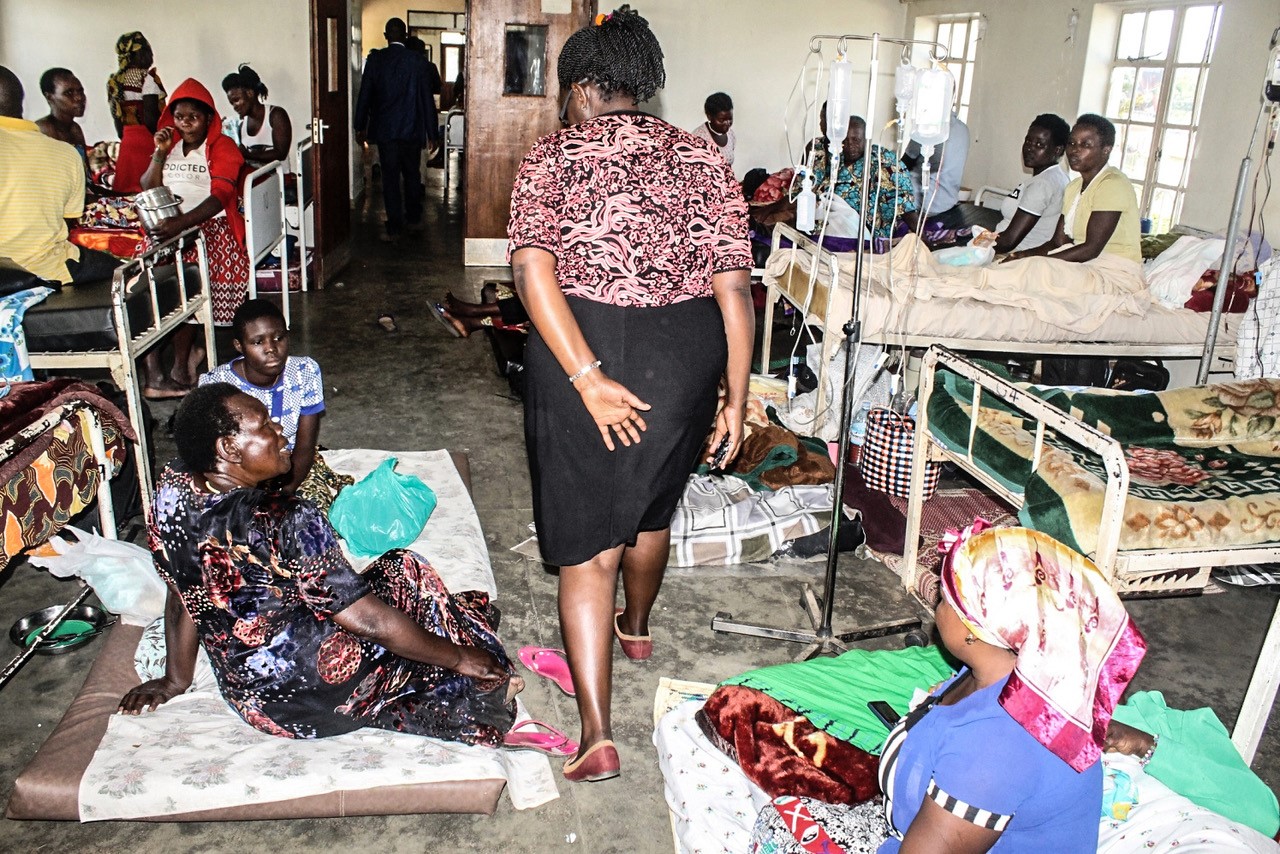
A patients in a ward at Fort Portal Regional Referral Hospital in 2019. PHOTO | FILE
What you need to know:
- Progress towards universal health coverage requires strong health systems and health workers who are educated and empowered to provide the health services that meet population health needs. However, this continuous process does not come easy for any government worldwide.
- The outbreak of the Covid-19 pandemic in late 2019 exacerbated the problem, rapidly more than ever, in several ways including loss of lives of qualified health workers.
- To mitigate this challenge, the World Health Organisation (WHO) called for building the health workforce back better as a commemoration of health worker week this month.
- In this week’s Health focus, Walter Mwesigye explains how the targets can be achieved in developing countries.
The disruption in provision of health services by the Covid-19 pandemic will be felt for much longer due to the effects on global health systems.
The COVID-19 pandemic claimed many health workers and put a huge strain on the global health system and an even greater one on Uganda's already over-burdened health system.
As recovery starts, health experts advise that it is time to rebuild both the workforce and the health system back better and stronger through private-public partnerships.
Ministry of health has for long engaged in such partnerships and as Dr Robert Mutumba explains, some of the essential disrupted services like reproductive health are now being revived due to the partnerships. Dr Mutumba is a Principal Medical Officer in charge of Reproductive and Child Health at the Ministry.
“We are seeing this marriage working out with the various partners, PSI, Path, USAID, they’re coming in first of all to support the commodity supply chain, they’re directly contributing to the procurement of the commodities and not limited to family planning supplies. In the districts they are able to support a number of other systems strengthening aspects in the use of data to provide targeted interventions.
In this regard, the ministry of health has for the last decade worked with Population Services International Uganda to especially extend the reach of high quality and reproductive health services to women of reproductive health across the country. Their focus was on private healthcare providers. Dr Mariam Luyiga is the senior technical advisor at PSI Uganda.
“We were looking at readiness of private health facilities to offer family planning and other sexual reproductive health services and we have done a lot of human resource capacity building to ensure that they can provide high quality services to the women. We have supported them with equipment like IUD insertion sets, autoclaves to ensure that the equipment used to provide services are safe,” he said.
“We have also built their capacity in health information management by training them on how to use the ministry of health data collection tools to ensure that they are collecting high quality data and reporting to the districts and to the national system to ensure that this data is used to plan for resources.”
DON'T MISS: Huge population choking Kampala hospitals
Dr Luyiga says they worked with 250 private clinics over the 10 years.
“But in the past three years, we have focused on improving the capacity of these private clinics for sustainability,” he explained.
One of the beneficiaries is Goretti Nankya who has been practising midwifery since 1986. After a 7-year stint in a public facility, she decided to start her own clinic in 1996.
“They facilitated my facility with the commodities I need, with instruments and they have been supervising me to see that the work we do is of quality. When they give you knowledge and support you, they give you money which helps to reach a bigger catchment”
Minister for health Dr. Jane Ruth Aceng says the partnerships have made it possible for them to boost service provision.
“This is to support government programs especially where funding is a challenge where we go into an agreement with the partners. It has supported the Ministry of Health in many areas especially in the area of infrastructure and commodities. We benefit from these public-private partnerships in many ways to strengthen our programs and to ensure funding is available at any time,” she said.
The COVID-19 pandemic claimed many health workers and put a huge strain on the global health system and an even greater one on Uganda's already over-burdened health system. As recovery goes on, Dr Mutumba says the ever growing population has triggered them to finding new and innovative ways of service provision.
“There is that enhanced focus on capacity blinding, the ministry of health has also adapted the self-care guidelines, self-care is a new concept but it came in at a time when we needed it the most during the Covid-19 pandemic.”
The Country representative of PSI Uganda, Paul Mason says theirs was to push for a skilled and facilitated health workforce.
“we have been helping them by providing training making sure they understand what a quality service and product is, giving them support supervision and making sure they have access to the commodities they need and in many cases extending the range of products they offer. May be things like IUDS and implants,” Mr Paul Mason, Country Representative PSI Uganda.
“They introduced a voucher system where a client buys a voucher at only one thousand uganda shillings and is able to access maternal health programs at that cost. That is including family planning services,” said Dr Wasswa Farouk, Director, Nile Crescent Health Centre.
“It gave chance to these mothers to make a decision on how to give birth, how to plan for their families.”
“And doing cervical cancer screening, we benefited, a lot of clients come in, we make a difference in our community because not all facilities offer the services were are offering,” said Francis Twesige and administrator at St. Francis Domiciliary Clinic.
Shem Mutaza who supervises sexual and reproductive health services in Jinja district says bringing such care and services closer to women will help in mitigating recurrent problems around maternal health.
“Much as we could say we target the women, but the men were as well co-partners with these women because you can’t use a method of family planning in isolation without your spouse knowing. Or even in the event that they were having sexually transmitted infections which was a major focus for this program, they were able to get treatment.”
And, as the PSI Uganda 10-year support winds up, Dr Aceng says the public-private policy and law governing the implementation of such programs ensures sustainability.
The agreements are usually very clear as to when the relationship ends and the amount of work that is required to be done and it is always in such way that when the public-private partnership ends, government has to continue with the activities that were designed before.”
“We know that private sector requires a lot of funding but we have come up with strategies that are linking the private sector to government systems where we feel sustainability can be achieved and government systems we feel are low cost interventions that don’t require a lot of finial input from the sector,” said Dr Mariam
Over the years, pandemics and other natural disasters have proven our imperative need for health workers not only nationally but globally too. The experience of natural disasters has shown inadequacies such as lack of drugs, personnel, and equipment.