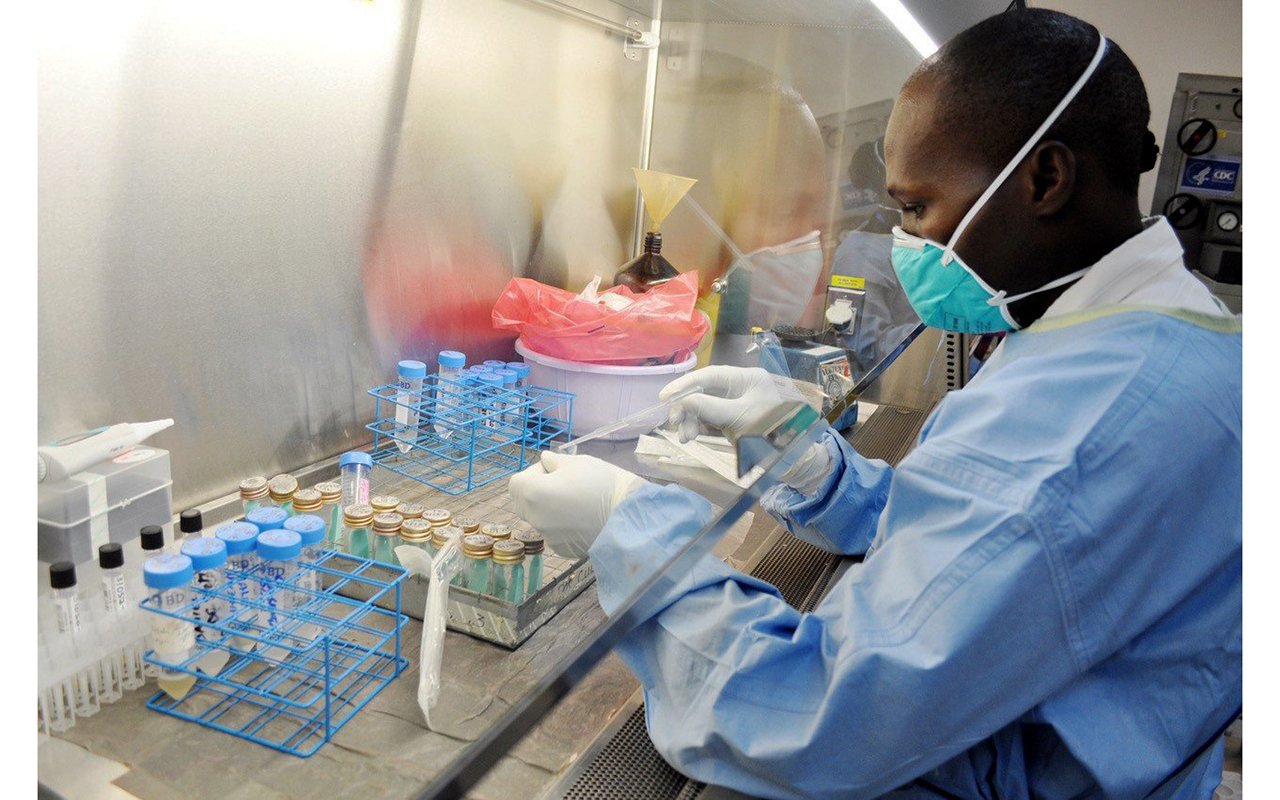
Covid-19 triggers new mental health crisis

Mental health patients at Arua Hospital share the same space with eye, nose, ear and throat patients. PHOTO/IRENE ABALO
What you need to know:
- Covid-19 pandemic has put the lives of mental health patients at risk. Daily Monitor visited Arua Regional Referral Hospital to speak to those directly trying to deal with this crisis.
- The challenges in Arua, however, cast a wider dark picture of the ailing healthcare service for the mentally ill.
In April 2020, Covid-19 breezed across the country and reached the deeper recesses, sending panic across the country’s ailing healthcare system.
To combat the threat, the Health ministry directed hospital directors at 14 regional referral facilities to convert mental health units into Covid-Treatment Units. (CTUs).
At the time this policy shift was introduced, health experts estimated that within a month, the pandemic would have receded and mental health patients would return to their isolation centres. But things took a turn for the worse as the second wave barrelled across the country with a deadly sting and brought the ailing health sector to its knees.
Neglected and left to fend for themselves, mental health patients were also afflicted by the Covid-19 pandemic.
The health workers who have to work within a constrained space, say the risk of virus infection remains high as a result of congestion.
In June 2020, Arua Regional Referral Hospital was thrust into the spotlight when mental health patients escaped from an alternative temporary unit and returned to the old unit where Covid-19 patients were being treated.
Dr Sr Ritha Binduru, a psychiatrist and Head of Department of Mental Health at Arua Hospital, says as part of treatment and healing process, mental health patients require space to interact.
The bed capacity of Arua Hospital by April 2015 stood at 372, according to the then director, Dr Bernard Odu. The hospital admits that some patients spend the night on the concrete slab, or sharing beds. This hospital serves as a referral for Adjumani, Arua, Koboko, Maracha, Moyo, Nebbi, Yumbe, and Zombo.
Elevated into a regional referral facility in 1994, the hospital also receives referrals from the neighbouring volatile states of South Sudan and the DR Congo whose health facilities are in a poor state of affairs. Some of its structures that have barely seen a fresh coat of paint date back to the 1930s when it was constructed.
“The (psychiatric) nurse who is here is in danger. There is no escape route if a patient enters, aggressive and violent, they can harm the nurse because the nurse will not know how to escape. [This is] a very small, narrow space, you cannot take off.
That is the biggest worry here. But thank God it has not yet happened but it was attempted,” Dr. Sr Binduru told Daily Monitor as a psychiatric nurse on duty stares poignantly. This temporary unit has a room, which is extremely narrow and also serves as a changing room for nurses on duty, resting room especially for those on night duty, prescription and dispensing medicines to patients.
Dr Binduru no longer has an office. She often conducts her assignments and attends to patients within free spaces that emerge.
She is scared that if patients are kept in a small space, they shall be at risk of contracting the Covid-19 virus.
The emergency response plan that took effect on April 14, 2020, was meant to be a short term measure but one and a half years, it feels like a lifetime as the extreme conditions take a toll on mental health workers and care-takers.
Daily Monitor visited Arua Regional Referral Hospital last week to speak to those directly who are trying to deal with this crisis.
At the ear, nose and throat section, a large crowd gathered to seek treatment. But one patient stood out from the rest.
Her darting eyes spotted a volatile patient who was moving closer to the crowds. The caretaker noticed that she had slipped from her side and rushed looking around the wards only to find her among patients in the eye clinic queue. She gently helped the mental health patient on her feet and guided her back to a crowded ward.
Dr Binduru says the hospital is always alert to deal with such emergencies. Another challenge health workers are confronted with is how to deal with mental health patients who contract covid-19 and share the same space with other Covid-19 patients and those afflicted by other diseases.
Dr Emmanuel Candia, the regional emergency medical services coordinator for West Nile, who is also the deputy coordinator Arua CTU, says despite this predicament, they have treated 40 patients with both mental health conditions and Covid-19.
“What we know is Covid causes low oxygen levels in the body and that affects how the brain functions. Many people will say the patients are not cooperative, but no, the brain needs oxygen and glucose for normal functioning. If that gets below the level that the body cannot cope, the brain gets a malfunction,” Dr Candia revealed.
He says as a result of the Covid-19, some patients experienced hallucinations and others lost their memory. While some recovered, others are still hospitalised at the mental unit.
Dr Juliet Nakku, the executive director of Butabika National Referral Hospital, says they have treated about 100 patients with mental health conditions and Covid-19, but made referrals for those who need Intensive Care services to other facilities such as the National Referral Hospital in Mulago.
She says as a result of space constraints, the hospital cannot adequately manage Covid-19 patients with mental health conditions.
Nakku argues: “You cannot confine a mental health patient. The condition of delirium comes for many reasons, Covid-19 being one of them, causes one to not be able to understand where they are, what time it might be or year or month, they are disoriented. It may cause them to perceive their environment differently. To see as if certain things are not what they are.

Dr Juliet Nakku, the executive director of Butabika Hospital, says the hospital has treated about 100 patients with mental health conditions and covid-19. PHOTO/WILLIAM KINTU
A belt for example may look like a snake, a pen may look like a knife. It makes people feel very agitated and scared and they may be flying out of windows and running around and feeling as if they are being persecuted. It disrupts their sleep.”
Currently, Butabika National Referral Mental Hospital has about 900 admissions yet the hospital has a 500-bed capacity, according to Dr Nakku, who is also a consultant psychiatrist.
“There is a need to rethink mental health units and Covid management to enable proper management of the two related conditions,” argues Nakku.
Some of the patients who could afford home based-care and treatment stayed away from mental health facilities as they managed both covid-19 and mental health conditions.
Mr Edward Nkurunungi, the executive director of Peer Nation, a Kampala based non-governmental organisation that supports mental health patients and families coping with mental health conditions, is recovering from psychosis. This is a mental disorder peppered by a disconnection from reality. Psychosis may occur as a result of a psychiatric illness such as schizophrenia. In other instances, it may be caused by a health condition, medication or drug use with possible symptoms including delusions, hallucinations, talking incoherently and agitation.
Nkurunungi tested positive for Covid-19 on June 7, during the second wave, his wife too was positive. He chose to isolate at home.
“The illness itself is a very nasty experience. I would not encourage anyone to be in a crowd. I even had to separate beds with my spouse. Fortunately, we have a three bedroomed house so we would only get together at meals, but we were socially distant. We were steaming using different things, she would use a bucket and I would use a basin. But in a crowded place such as Butabika, the bed capacity is 500 and yet there can be close to 1,000 patients. Some sleep on the beds, some on the corridors. It is not decent to be in such a crowded place when you have Covid,” Nkurunungi reveals.
He says more needs to be done for mental health patients to feel safe at health facilities.
“Our colleagues in the countryside are losing out on treatment where they do not have facilities and Covid has made mental illness more serious. It’s a question of priority. Covid has become more prioritised than mental health which we have had for some time. But I think the first lockdown gave government to prepare for conditions that are worse than at that time,” says Mr Nkurunungi.

Experts say anxiety has triggered mental health challenges among people. PHOTO/FILE
Whereas the Health ministry gave a directive to convert mental health units into Covid Treatment Units, some hospitals did not comply.
Gulu Regional Referral Hospital is at the heart of the Acholi Sub-region that was under the clutches of an insurgency. As thousands of its people attempt to shake off the shackles of trauma and other psychological scars, many remain trapped in mental and emotional turmoil.
The hospital management decided to utilise the tuberculosis ward that had fewer patients as the CTU and maintained the mental health unit to provide enough space for recovering patients. Dr Paska Apiyo, the in-charge of CTU Gulu, said:
“Remember our region has suffered a lot (due to war). There is a lot of mental illness; post-traumatic stress disorders, bipolar, and so forth. We noticed that the mental health unit would have so many of these patients and we felt that if we were to change, we would have nowhere to manage them. It would be another problem.”
The facility does not have the capacity to handle more than 50 mental health and covid-19 cases at a go yet the patients cannot also be admitted in the same ward with other covid-19 patients at other designated CTUs like Namboole CTU and Mulago hospital among others.
Whereas the decisions made during the Covid-19 early emergency response periods have remained in place, mental health experts say there is need for a blue-print to deal with the mental health crisis and the establishment of a national mental health task-force.
Dr Sr Binduru says the mental health units should revert to patients ailing with mental health conditions and government should construct CTUs to cater for Covid-19 patients.
Dr Jane Ruth Aceng, the Health minister, recently told Parliament that plans are underway to construct CTUs to decongest mental health units.
By the time, Covid-19 struck, Uganda was already grappling with rising numbers of mental health patients as a result of drug and alcohol abuse largely amongst its youths in a country, which only has 50 trained psychiatrists.
The numbers of those ailing with mental health conditions have surged as a result of the pandemic as families deal with economic distress, domestic violence, alcohol abuse and depression yet government has offered no solution to confront this new health crisis.
Survey
In an interview with this newspaper in June, Mr Moses Karis Oteba, a psychologist at Defend Defenders, an international non-governmental organisation, said things such as loss of a loved one, loss of a job, breakdown of relationships or marriages, poor academic performance, self-image issues, among other problems, can cause one to have a mental health crisis.
He said a notable number of people were not aware of the psychological impact of the first lockdown.
“Most people thought they were strong enough and could handle the effects brought about by the first lockdown. Besides, we did not know exactly what we were dealing with then. This notion has been challenged this time round.
“In the second lockdown, more people have become vulnerable after remembering what they went through in the first lockdown. Also the continuous information, including inaccurate material on Covid-19, making rounds is not making life any easy for people,” he said.
The impact is well illustrated in a June 2021 Sauti zaWananchi survey by Twaweza, a non-governmental organisation. Across Uganda, 51 percent of people said emotional and sexual violence has got worse during the lockdown, which triggered mental issues among many.
Fifty eight percent mentioned increase in problems related to alcohol consumption and drug abuse as causes for mental breakdown.