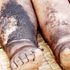
Some of the people with elephantiasis disease in Kamwenge. PHOTO/ALEX ASHABA
|Special Reports
Prime
Elephantiasis plants sting of death in Kamwenge community
What you need to know:
- Nearly nine years since Lymphatic Filariasis, commonly known as Elephantiasis, was first flagged in Kamwenge District at the edge of Kibale National Park by a team of experts from the Health Ministry, World Health Organisation and US’ Centers for Disease Control and Prevention.
- Comfort for the hundreds of victims—patients and those who have lost loved ones—remains a far cry. The ravaged villages have turned into a magnet for researchers and epidemiologists who camp here in droves amid despair and dejection, but without offering solutions, writes Frederic Musisi.
Death is an unavoidable part of the cycle of life. But does one need to think about it? For many Elephantiasis patients this frightening thought lingers like an apparition.
When a neighbour succumbs to this debilitating disease, this casts a pall over the community. The despair is further compounded by patients who self-medicate as they fear to walk to a nearby health facility as they grapple with perpetual isolation and stigma.
Husbands have abandoned their wives. Husbands with the disease feel inadequate, while children are treated as outcasts and sent to far-flung places to live with their relatives. As a result, many drop out of school.
Fifty-five year old Christopher Bernard Rubagyire died on July 29. His death momentarily shook his community of Mukiraara Village in Busiriba Sub-county in Kamwenge. He had contracted Elephantiasis five years earlier, during which period he advocated for other patients not to be seen as outcasts.
“He went through a lot of pain, and struggles,” Rubagyire’s daughter, Smollen Alihimbise recounted two days after burial. “We were in and out of hospital, but even getting medical assistance was not the easiest experience.”
Two weeks before, a documentary filming team working on a story on the plight of Elephantiasis patients had spoken to Rubagyire. In the video, he seemed upbeat and offered counsel to his community.
The bearer of the bad news arrived at the village a day before I and my cameraman, William Kintu, travelled to the community to document this story. The deceased had been recommended to us among the resourceful people to talk to.
According Alihimbise, for the most part, the deceased and like many other ailing patients, unable to live productive lives, survived on handouts from Non-govermental Organisations (NGOs).
“There was an organisation that used to give him soap to wash his legs but we did not get any help from our local leaders or even government,” she lamented.
Soap and detergents are among the most essential, yet basic, items needed by Elephantiasis patients to treat their wounds.
The recent rise in prices of household items, including soap which prohibitively costs between Shs7,000 and Shs10,000, pushed many patients to the brink.
Constant cleansing and covering the wounds, Vincent Mwesigye, a principal laboratory technologist at Mbarara University, told this newspaper, is a vital aspect of the patients’ survival.
“More efforts are needed in education and promotion of WASH—water, sanitation and hygiene—around the affected villages,” Mr Mwesigye, who in 2019 conducted research on the antigen prevalence and risk factors for Podoconiosis under a research grant to Makerere and Mbarara Universities, said.
“And if more financial support is there, we can support them with protective gear and most importantly integrating access to health care for the disease in nearby health centres.”
The illness
The main characteristics of the Elephantiasis is disfiguring—rugged swelling— of both the lower and upper limbs (legs and hands). It also attacks breasts, and sometimes internal organs. The swelling is irreversible and with exposure to other opportunistic infections that weaken the immune system, the inevitable result is death.
The Kamwenge District Woman MP, Ms Sylvia Bahireira Tumwekwase, put the death toll to more than 200 since the disease ravaged this community.
“We don’t have clear budgets for help, and yet people are dying silently. Because of stigma, when some patients die family members bury quietly and fast so it is hard to keep track,” Ms Tumwekwase said.
“The patients we have between 700 to 1,000 but they are also hard to keep track of,” she said.
The World Health Organisation (WHO) describes Elephantiasis or Lymphatic filariasis, as a painful and profoundly disfiguring disease, caused by infection with parasites classified as nematodes (roundworms) of the family Filariodidea that are transmitted through the bites of infected mosquitos.
Mosquito-transmitted larvae are deposited on the skin from where they can enter the body. The larvae then migrate to the lymphatic vessels where they develop into adult worms, thus continuing a cycle of transmission.
In communities where Filariasis is transmitted, all ages are affected. While the infection may be acquired during childhood, its visible manifestations such as limbs oedema may occur later in life, causing temporary or permanent disability.
In endemic countries, lymphatic filariasis has a major social and economic impact. Elephantiasis, according to the WHO, affects more than 120 million people in 72 countries throughout the tropics and sub-tropics of Asia, Africa, the Western Pacific, and parts of the Caribbean and South America.

Some of the patients with elephantiasis. The disease causes pain leading to unproductivity. PHOTO/ALEX ASHABA
When the disease was first flagged in 2014, a team of experts from the Ministry of Health, World Health Organisation and US’ Centre for Disease Control and Prevention camped in the area to undertake investigations.
It was established that the Kamwenge strain was different from others.
The Kamwenge strain, which researchers call Podoconiosis—non-filarial—nonworm transmitted— Elephantiasis, it was established, is caused by long term contact with soils sullied with alkaline volcanic rock minerals such as silicon and aluminium.
In summary, according to a 2015 study by Dr Christine Kihembo, the then Ministry of Health senior epidemiologist and now working with the African Field Epidemiology Network, people go farming bare-footed where the mineral particles penetrate the skin, which are absorbed by macro phages—a type of white blood cell that surrounds and kills microorganisms and stimulates the action of other immune system cells—into the lymphatic system—which is part of a human body’s immune system, then inflammation begins which means predisposition leading to lymphatic fibrosis—a soft and fatty growing swelling—and eventually lymphedema, swelling of tissues caused by an accumulation of protein-rich fluid that is usually drained through the body and lymphatic system.
The possible factors, the study noted, is because farmers hardly wear shoes while tending to their gardens nor do they wash their feet.
“Prolonged foot exposure to volcanic soils is a risk factor for Podoconiosis,” the study concluded.
However, because the affected village shares boundaries with a wildlife sanctuary, there is a myth that elephant dung mixed with the soils is perhaps the cause of this strange strain.
As such, many individuals continue to disregard advice of wearing protective gear such as boots while tending to the gardens.
Far from comfort
Barely after President Museveni had campaigned in the area, last September, Prime Minister Robinah Nabbanja, accompanied by a team from the Health ministry went to the affected villages, after the District Woman MP raised the matter on the floor of Parliament. They distributed relief items, which were barely enough to cater for the community.
Mr Everest Beyanga, the Busiriba Village chairperson and volunteer, said everyone concerned in the country is aware of the problem.
“People continue losing lives. Men and women are widowed. Children are orphaned, but no one outside seems to care. Most times we just bury the dead because health workers don’t want to conduct postmortems,” Mr Beyanga said, adding: “The patients are advised to wash their limbs at least three times a day but many are poor to afford soap.”
While the cause of the disease is now known, Mr Mwesigye revealed that more studies ought to be conducted, especially on genetic mapping.
“You find in a family that farms the same garden when one person has the disease and others don’t, so we need to further study that,” he said during an interview at Mbarara University.
“Other than that, I think we need more education on primary health-care, on footwear when people are going to gardens and also the entire community on stigmatising patients; in some homesteads, people with the disease hide in their houses as early as 2pm because they are laughed at or feel unwanted.”

Like Alex Giita, a patient, said, perhaps it is high time government came to the rescue of the community.
“Everyone who comes here sympathises with us, gives us money to buy soap but they don’t talk about the real problem and the end to it. This side, people keep dying even if not in many numbers,” he said.
One of the solutions could be relocating all residents to other parts and de-gazette the affected villages as part of the national park.
Patients narrate pain
Thirty-year old Medius Tugumisirize, a resident of Busiriba Village, has battled Elephantiasis for 15 years. Two of her four children died because of lack of proper care. She can’t suppress the fear of dying.
“My husband also had this disease and he died. I have suffered so much, the pain at times it is unbearable. I used to go hospital and they would tell me that I have no disease. Sometimes, my children are forced to fend for themselves food. I need help,” Tugumisirize lamented.
Like all other Elephantiasis patients, she is often frustrated that at Busiriba Health Centre II as they are not given attention and are often referred to private health clinics in far areas.
Ms Kevina Tumuhairwe, a resident of Mukiraara Village, shares her pain and anguish.
“Our legs are swollen so we look funny. When it’s too hot the skin peels off. We are told to always wash them with warm water and soap and smear with vaseline, but the pain is sometimes unbearable,” she says.
When she contracted the disease, Tumuhairwe said her husband and children avoided her.
“He does not want to walk with me and even for wedding ceremonies, he leaves me behind. Even the children look down on me, imagine. This makes me feel so uncomfortably bad of myself,” she noted. “We need help from the government because our husbands don’t take care of us. We can’t take care of our gardens anymore. The planting season is coming but we can’t do anything because the pain is too much.”
Christine Atwikirize, a resident of Kyakatoma Cell- Kamwenge and mother of four, has battled Elephantiasis for close to 20 years. She heeded the doctor’s advice of persistent hygiene but as she grows older, she can barely take care of herself.
“I cannot do anything on my own. I cannot dig. My children are suffering without any food to feed them. I am in great pain; my prayer is if someone could come to my rescue. I need a decent house of my own,” she revealed.
Fifteen-year-old Lovina AKasasira, a resident of Kahondo Cell, Kirumba Parish, dropped out of school due to the stigma and embarrassment from fellow students.
Her mother, Gloria Atuhaire, a teacher often went to school to attend to her daughter when her feet cracked.
About kamwenge
The district was created in 2000 by an Act of Parliament. Prior to then, it was part of Kabarole District.
The district covers an area of approximately 2,439 km² and 2.6 percent is covered by open water.
It is predominantly a rural district with some of the worst poverty levels in the country.
The district has one hospital-Rukunyu in Kahunge Sub-county on Kamwenge-Fortportal road.
The national population census and household survey of August 27, 2014 enumerated the population of the district at 414,454 inhabitants.