Prime
About adverse drug reactions
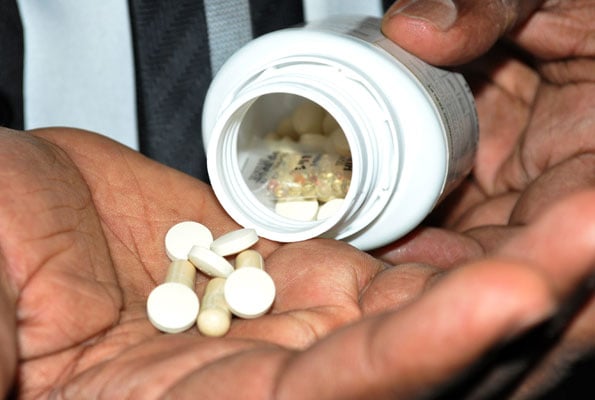
It is dangerous to use drugs for any purpose other than that for which they have been prescribed, as this could lead to health complications. File photo
What you need to know:
- The overall increase in the number of ADR reports is a positive development that we should all embrace and applaud.
- The more ADRs we know about, the better we can improve the quality of care for our patients.
Reference is made to an article titled “NDA lists drugs and vaccines with adverse side effects” that was published on page 2 of the Daily Monitor dated Thursday, May 5, 2022.
The story is timely because recent developments in global public health, such as the massive rollout of Covid-19 vaccination, have ignited an intense public debate on the issue of adverse drug reactions.
In the wake of the current global Infodemic, statistical reports without context only serve as cannon fodder for the conspiracy theorist. I was, therefore, intrigued that the editor may have overlooked the need to anchor this story in a scientific context.
Like all good things, medical interventions may result in unintended consequences that may either be beneficial, harmful, or even neutral in their impact. Adverse drug reactions (ADRs) are the potentially dangerous effects that may occur following the administration of medical treatment. ADRs may or may not be foreseeable or even immediately observable and may present with symptoms that range from mild self-limiting to severe and life-threatening ones.
While most adverse drug events may be observed and documented during randomised clinical trials, healthcare providers occasionally encounter patients presenting with adverse drug events of erstwhile unknown cause (adverse drug reactions).
For that reason, there is an entire branch of science (pharmacovigilance) dedicated to studying the effects of drugs in large populations. The benefits of pharmacovigilance are underpinned by numerous beneficial findings, such as repurposing certain medications like sildenafil (originally licensed for pulmonary hypertension) and the discontinuation of others like stavudine (due to mitochondrial toxicity).
Adverse drug reactions are an issue of public health importance because of their significant contribution to the overall burden of disease and death.
Although the global burden of adverse drug reactions is unknown, a recent study estimated that ADRs contribute to 3.5 percent of hospital admissions and approximately 197,000 deaths in Europe annually (1) while another study conducted in Mbarara regional referral hospital reported that almost half of the hospitalized elderly patients experienced at least one ADR during their hospital stay (2). This underscores the need for significant investment in pharmacovigilance in low- and middle-income countries where the disease burden is significantly higher.
In Uganda, the collaboration between the Ministry of Health and HIV/Aids implementing partners to monitor the adverse effects of antiretroviral and TB treatment is paying off, as evidenced by the increasing number of ADR reports submitted to the National Drug authority (NDA).
The disproportionate contribution of covid 19 vaccines, ARVs, and TB medications to the number of the ADR reports is not surprising because some of the implicated products are either new on the market or are being used at a large scale for the first time. A case in point is the DTG based regimens currently being prescribed for more than 90 percent of the approximately 1.2 million recipients of antiretroviral treatment in Uganda.
By the scale of use, it is only expected that we observe more of the previously undocumented adverse effects.
Although there have been a few reports of ADRs such as hyperglycemia, reduced libido, and insomnia associated with DTG, it is a generally well-tolerated drug in most of the patients and it has proved one of the most efficacious ARVs available today.
On that note, I would like to draw your attention to the role of information overload (such as that experienced during a pandemic or rollout of new treatments) in increasing the likelihood of experiencing undesirable drug effects. There is plenty of scientific evidence of the nocebo effect in patients who receive information about the risk of adverse drug reactions .
Nonetheless, the risk of new-onset hyperglycemia in patients transitioned to DTG based regimens, as reported by Lamorde et al. , has been corroborated by other researchers. This underlines the importance of targeted blood glucose monitoring in patients on this regimen.
In conclusion, I would like to clarify that there was an increase in ADR reports rather than adverse drug reactions. The perceived increase in adverse drug reactions reported in the article is a misreading of the statistics.
The overall increase in the number of ADR reports is a positive development that we should all embrace and applaud. The more ADRs we know about, the better we can improve the quality of care for our patients.
Anthony B. Mutema, Pharmacist, Aids Healthcare Foundation