Prime
What you need to know about jaundice
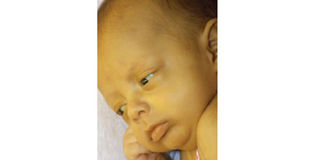
What you need to know:
Infection. Perhaps your baby has suffered from jaundice or you have seen a baby skin turning yellow. Beatrice Nakibuuka shares symptoms and treatment of the infection among infants.
Lilian Namatovu delivered her 1.8kg baby normally and was discharged from Mengo Hospital 24 hours later. After three days, her baby was very weak, its skin started turning pale yellow and was vomiting. Although she was advised by women in her neighbourhood to give the baby herbs, she did not buy their advice.
“My neighbours told me that the condition is called Kamuli and that it was curable with herbs. Each day, the baby grew paler and yellowish. Despite the fact that my baby was fragile, I could not administer any medicine. I visited a paediatrician at the same hospital,” she recalls.
When a blood sample was taken, the baby was diagnosed with neonatal jaundice, although the doctor said it was mild case. “The doctor advised me to expose the baby to light for 10 minutes daily and after a week, the baby was normal again,” Namatovu says.
According to Dr Sabrina Kitaka, a consultant paeditrician at Mulago National Referral Hospital, neonatal jaundice is a common condition among preterm babies because their liver is not fully formed. Other risky conditions include an infection in the baby’s blood sepsis, internal bleeding as a result of difficult delivery, when the baby has a liver malfunction, enzyme deficiency, especially for babies who lack the substance that metabolises milk, bacterial or viral infections and an incompatibility between the mother’s blood and that of the baby.
Dr Kitaka advises mothers to look out for jaundice symptoms such as irritability and yellowing of the the skin and the sclera (white area and make an effort to see a paediatrician.
Causes
About four out of 10 newborn babies develop neonatal jaundice due to the immaturity of the liver excretory function, three days after birth. Fortunately, this jaundice begins to clear on its own towards the end of the first week of the baby’s life.
“While in the womb, the baby’s waste products (bilirubin) are excreted through the placenta. The excretion process must continue even when the baby is born. It takes time for some neonates to be able to excrete wastes which cause a build-up of these wastes in the body. High concentration of waste in the baby’s blood causes yellowing of the skin and eyes,” says Dr Kitaka.
Too much waste in the baby’s blood can also be caused by infections obtained while the baby is in the womb. Infections such as syphilis and herpes can cross into the placenta and affect a new born.
When there is too much waste content in the baby’s blood, if it is untreated it can got to the brain and affect the cells, leading to seizures and mental retardation. Sometimes it can even lead to death.
According to a study conducted by Dr Lillian Wambuzi in 2009 on prevalence, associated factors and immediate outcome of neonatal jaundice in special care unit at Mulago Hospital, majority of the neonates (79 per cent) had hyperbilirubinaemia caused by wastes in the babies blood and 16 per cent died within seven days of jaundice onset.
Treatment
The treatment intervention given to a neonate depends on how much waste is in the baby’s blood and the cause of jaundice.
For example, if a child has physiological jaundice, it disappears normally within seven days. All the mother needs to do is to expose the baby to sunlight.
Dr Kitaka says: “Expose the baby to early morning light for about 10 minutes daily because light helps the baby’s body to convert the bilirubin (wastes) into a substance that can be passed out by the baby.”
When the amount of waste in the baby’s blood is too much after a blood test, a baby is exposed to a fluorescent light called phototherapy, which converts the bilirubin into a form that can be passed out as waste (urine or stool) by the baby.
“If there is a risk of the bilirubin rising to dangerous levels even after phototherapy, blood transfusion should be done,” says Dr Kitaka.




