Safe sex practices key to curbing pelvic inflammatory disease

See your doctor you experience severe pain in the lower abdomen and fever, with a temperature higher than 101 F (38.3 C). Photo | Internet
What you need to know:
- If your doctor diagnoses PID, you should tell anyone you have had sex with in the past 60 days about your illness. If it has been longer than 60 days since you have had sex, tell your most recent partner, who should also get treated. Practicing safe sex, however, is the best way to prevent this disease.
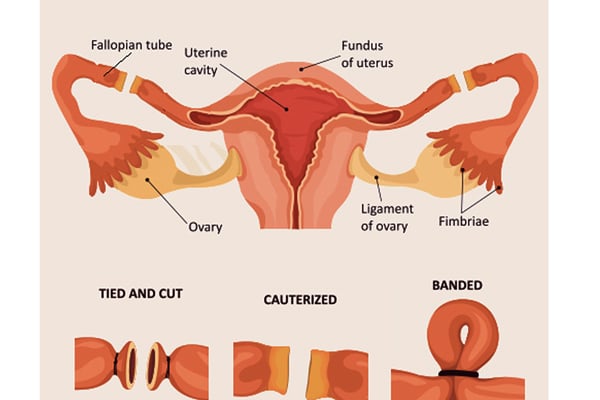
Pelvic Inflammatory Disease (PID) is an infection that causes reddening and swelling of the upper reproductive organs found in the pelvic cavity. These include the cervix, uterus and fallopian tubes. It is typically caused by sexually transmitted diseases such as chlamydia and gonorrhea, ascending from the birth canal upwards to the upper reproductive organs.
Jessica Kirabo experienced a lot of pain, originating from her lower back and ovaries. Most times, she could not walk. A friend recommended some painkillers which she took but after two hours, the pain persisted.
At the hospital, she was given intravenous medication to manage the pain while the doctor also recommended a transvaginal scan that revealed PID as the cause of pain.
The Centres for Disease Control and Prevention (CDC) has estimated that more than one million women experience an episode of PID every year.
Dr John Wanyama, a gynaecologist at Naguru Hospital in Kampala, says the disease affects women of reproductive age (between 15 and 35 years).
Dr Wanyama adds that PIV can be acute or chronic; with acute PID causing sudden inflammation of the uterus, fallopian tubes, ovaries and pelvic area due to infection. Chronic PID is when the inflammation persists for a long time.
Sometimes the bacterial, viral or fungal infections start from the vagina and if not treated, the microorganisms start moving upwards, inflaming the tubes, ovaries and cervix.
Causes and risk factors
Although there are several causes of PID, the most common are bacterial infections that start in the vagina and when not properly managed, ascend to the pelvic cavity.
Anyone can get a PID, especially if you are sexually active. Men are carriers of the disease although they may not show any signs and symptoms. Also, if a woman has multiple sexual partners, they are more susceptible to getting PID.
According to Dr John Sekyanzi, a medical officer at Women’s Hospital International Fertility Centre in Bukoto, Kampala, if one has had an infection, it is a risk that makes them vulnerable to getting PID, especially if it is not well managed.
Poor hygiene of the urinary system, wearing dump underwear, sharing under garments, not changing pads, and use of chemicals and soaps can also increase one’s risk of getting PID. Practices such as douching also interfere with the normal PH of the birth canal.
“Since the birth canal is open, poor hygiene and not changing pads or tampons regularly increases the risk of bacteria going beyond the cervix, causing PID,” Dr Sekyanzi says.
Dr Wanyama remarks that although it is not among the leading causes of PID, using a dirty or contaminated toilet is a risk factor.
“If someone who has PID uses a toilet and leaves pus cells on it, the next user is likely to get the disease if they do not wipe the toilet seat with a detergent,” he says.
People with immune suppression are also likely to suffer from PID since their bodies cannot fight infections.
Wrong use of antibiotics
Irrational use of antibiotics is another challenge according to Dr Sekyanzi. “Many people self-medicate yet they do not know the correct dosage. Since they are non-selective, these medicines in the long run also destroy the good bacteria, creating a chance for inflammation of the upper reproductive organs.”
Women should know that the IUD enables communication between the cervix and the uterus. It is, therefore, easy for the bacteria to ascend up the uterus using this link to the fallopian tubes and ovaries.
“Whereas an IUD per se does not cause PID, it can increase your chances of getting it in the event you are promiscuous,” Dr Wanyama adds.
Symptoms, diagnosis
At the onset of the disease, it may not be easy to differentiate PID from other infections. This is because there is an overlap on some of the signs and symptoms.
According to Dr Wanyama, chronic abdominal pain that lasts more than two weeks, pelvic pain, fever and chills, abnormal discharge from the birth canal are some of the signs. The discharge is usually thick, more than normal and the colour may be yellowish, white, and greenish, depending on the type of microorganism causing the inflammation.
Painful urination, intercourse, pressure on the bladder, abnormal uterine bleeding, unstable periods that may be very light or very heavy are other signs.
The CDC remarks that when present, signs and symptoms of PID are nonspecific, so other reproductive tract illnesses and diseases of both the urinary and the gastrointestinal tracts should be considered when evaluating a sexually active woman with lower abdominal pain.
About 60 percent of the diagnosis for this inflammation depends on taking patient history of the signs and symptoms Dr Sekyanzi says.
“However, this may be inconclusive, so the doctor usually recommends other tests such as laparoscopy, a transvaginal scan, high vaginal swab, hysteroscopy, as well as tissue biopsy to rule out cancer of the cervix and endometrial carcinomas which have similar symptoms like a PID,” he adds.
Treatment
Once diagnosed early, one can be treated and cured with medication, depending on the cause of the inflammation. Only in severe cases does one need hospitalisation but when the disease advances, it can cause development of scar tissues in the uterus, which can lead to total infertility.
Treatment for PID should start as soon as your medication is prescribed depending on the severity of the disease. If you have mild to moderate PID, the doctor will prescribe a course of antibiotics and painkillers.
It is important to inform your doctor about any other medicines you are taking since antibiotics can interfere with the effectiveness of some other medicines.
The treatment course can last two weeks and it is very important to complete your dose even if you get better. Women who complete their course of antibiotics do not get any long-term health or fertility problems.
In complicated cases, one may need surgery to remove the scar tissue that may have formed in the uterus, remove the polyps or cysts or abscess.
For men
Men can be silent carriers of the bacteria that causes PID, the reason a woman's infection can reoccur if their partner does not receive treatment. It is, therefore, important for you to receive treatment together with your partner once one is diagnosed with PID.
Dr Sekyanzi recommends abstaining from sex while on treatment, or use condoms until the infection has cleared.
According to CDC, the decision of whether hospitalisation is necessary should be based on provider judgment and whether the woman has surgical emergencies such as appendicitis that cannot be excluded, tubo-ovarian abscess, pregnancy, severe illness, nausea and vomiting, unable to follow or tolerate an outpatient oral regimen or no clinical response to oral antimicrobial therapy.
Complications
Untreated or recurrent pelvic inflammatory disease has potential complications such as infertility, ectopic pregnancy, and chronic pelvic pain, says Dr John Wanyama, a gynaecologist at Naguru Hospital in Kampala.
“Recurrent miscarriages reveal that the cervix is too weak to hold the baby. This is one of the late stage complications of PID. Some women experience delayed conception or even complete infertility,” he adds.
Some women experience reduced flow of periods while others get very heavy periods, vaginal dryness, uterine polyps, cervical cysts, abscess in the tubes, tubal blockage.
Prevention
The safest ways to reduce the risk of developing PID, include safe sexual practices, regular STI testing, practicing proper hygiene, contacting a professional health worker in treating any vaginal infections.