We must embrace patient-centred care in maternity units
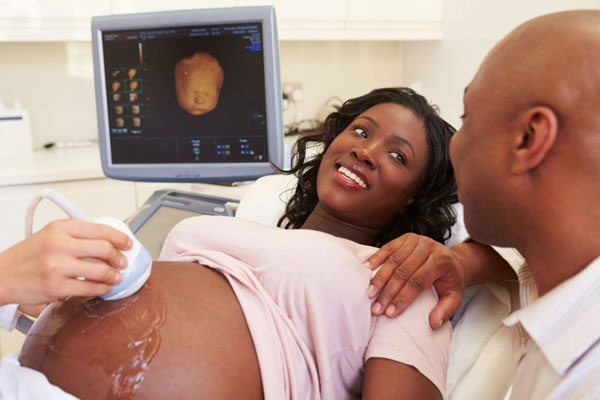
Maintaining a relationship with a single provider can give you the help and support that you need. PHOTO/HEALTHLINE.COM
What you need to know:
- The safety of a mother and her child is and will always be a priority for any health service provider.
- This is why it is important for all parties involved to ensure that both mother and child are taken care of during their stay in hospital and follow up done when they leave to go home.
There is nothing more fascinating than maternity ward stories. Now that social media has provided a platform for mothers to share their stories, more and more women are coming out and sharing their experiences during the most dramatic moments of their lives.
Reading these stories opens the door into a glimpse of what it takes women to bring forth the future generation, a task they did not bargain for but continue to execute with sterling commitment. Some take me back to my experiences on the other side of the divide and remind me just how much practising obstetrics is akin to riding a roller-coaster.
I remember Atieno*, who strode into our maternity unit during the mid-morning hours with a swanky backpack on her shoulders, exuding the confidence of a runway model. She assured me she would be done in a few hours since she was very fit.
She woke up at five every morning and walked to Gikomba, the largest open air market in Kenya, to buy stock for her second-hand shop in the city centre. By eight, she was back in her shop, having covered nine kilometres.
I examined Atieno and found she was already in active labour. I broke her waters and gave her approximately four hours before her baby arrived. By the time I was done with my reviews, all I heard were screams and wails from mothers all around the ward. My eyes popped out when I looked into Atieno’s cubicle. She was standing on top of her bed, hanging onto the curtain rail above her, screaming expletives in her native language. There was no trace of the regal woman who had sashayed into our unit.
Jebet* was even more dramatic. She lay stark naked in her bed, save for her brasserie, on a freezing cold night. The rain outside was drenching the earth at an alarming rate. Storm drains around the solid colonial building were roaring with gallons of rain water headed to the trenches. Jebet’s screams rose and fell in perfect crescendo-decrescendo with each contraction.
With all the running around we were doing that night, we all failed to register the precise moment Jebet’s screaming stopped. This was until Jebet was escorted back into the ward by four security officers. At the height of it all, Jebet had tossed off her bedsheet and made a run for it. She did not count on the gate being locked, curtailing her effort to leave the madness behind.
It was quite a spectacle to watch the serious-looking officers forming a wall around her while facing away, as they walked her back. She was naked and soaked like a ragdoll, in atmospheric temperatures of 120C. The nurses had to wipe her down and cover her in blankets, with a heater beside her bed, to stop the violent shivers. An hour later, she delivered the most adorable baby girl.
The challenges
While these experiences generate a lot of humour, they point to challenges in our systems that we need to address in order to boast of a truly patient-centred approach to the care we provide our patients. The maternity units provide a great insight into our responsiveness. This is because the pregnancy and childbirth journey provides a great opportunity to adopt Picker’s “Eight Principles of Patient-Centred Care”.
First is respect for patients’ values, preferences and expressed needs. For us to effectively do so, we have to involve patients in decision-making by upholding their values and preferences. This assures that each patient is treated with respect, dignity, and appreciation of their autonomy. If her cultural practices consider labouring a community experience, how do we make room for her kin within the unit during her labour?
Integration
The second principle speaks to coordination and integration of care so as to minimise the vulnerability of patients in the course of seeking care. It does not matter if one has an amazing facility yet patients keep getting lost trying to find their way from one service to another. It makes the facility intimidating.
The third principle addresses the need for information and education on their medical condition and the process by which the care is provided. This empowers the patient to effectively participate in their own care, something our healthcare systems sorely lack.
The fourth one should be everyone’s favourite principle; physical comfort. We all want creature comforts in our spaces. Having a comfortable, homely, and clean environment is even more important in ill health. Further, no one deserves to be in pain. Alleviating pain should never be viewed as a privilege but rather be upheld as a patient’s right.
Emotional support
Right after physical comfort is emotional support and alleviation of fear and anxiety. Healthcare providers must at all times remember that the hospital is an unfamiliar environment and thus elicits a lot of anxiety for both the patient and her family members.
There is need for appropriate support for patient concerns regarding diagnosis, treatment and expected outcomes. Further, we must always remember that patients are not prisoners and the hospitals must, at all times, aspire to minimise the isolation they cause by not accommodating relatives.
The seventh principle addresses continuity of care and transition. Is the new mother being discharged home ready to go? Has she learnt how to breastfeed or bathe the baby? Does she know how to contact the hospital in the event of complications once she is home?
Access to care
The final principle speaks to access to care. Does the discharged mother know where the child welfare clinic is located or will she walk around for hours when she brings baby for immunisation?
Does her appointment for review consider a suitable time for a new mother?