Prime
Why maternal deaths are still high
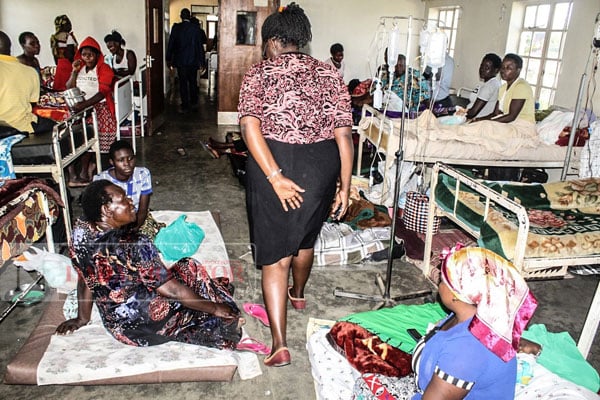
A congested patient ward at Fort Portal Regional Referral Hospital in 2019. PHOTO/FILE
What you need to know:
- Health officials cite government’s reluctance to address shortage of blood and supplies of essential commodities.
Deaths due to pregnancy-related complications have increased despite the heavy investment to improve health infrastructure and quality of care for women, government statistics indicate.
A total of 1,228 cases of maternal deaths were reported in hospitals last year, which is 11 percent higher than the 1,102 deaths reported in 2020, according to the Health ministry.
The increased deaths were as a result of heavy bleeding after birth, hypertensive disorders of pregnancy, malaria and other underlying conditions such as HIV/Aids, anaemia, and abortion complications.
However, health experts told Daily Monitor yesterday that the government’s reluctance to address the shortage of blood and gaps in transfusion services, limited personnel in facilities and supply of essential commodities are to blame for the increase.
Dr Herbert Luswata, the secretary-general of Uganda Medical Association, asked government to urgently address gaps in medical supplies and improve the units where mothers deliver from.
“Most deaths occur during the time of delivery, so access to medical supplies during the time of delivery is very important,” he said.
Dr Mukuzi Muhereza, a specialist at Nakaseke Hospital, said the National Medical Stores (NMS) has not been consistent in delivering essential medical supplies.
“I was crying around November and December [last year] because National Medical Stores was concentrating on supplying Covid-19 vaccines and had forgotten to send us essential medical supplies. Imagine sitting in a hospital and there are no gloves. This has serious effects on surgical patients when they have to buy the commodities which go past Shs400,000 [and yet they are unprepared],” he said.
But NMS admitted then that there was an interruption in supply, but said they would deliver the commodities.
Dr Luswata asked the government to equip facilities with specialists for handling women.
He said many facilities, especially health centre IVs (HCVIs) close at night because of shortage of doctors.
“Our HCIVs are ill-equipped. They don’t have [enough] doctors. In the current structure, HCIVs have only two doctors who can’t do [all the] emergency caesarean section to save mothers. This structure was put in place when the population was under 20 million but we are now at 43m,” Dr Luswata said.
“[In many cases], our HCIVs close at night because the few doctors who are there work tirelessly during day so cannot continue at night. There are many theatres in the country that government has constructed in HCIVs but if you go in the night, they are locked,” he added.
In response, Dr Charles Olaro, the director of clinical services at the Ministry of Health, said they are increasing efforts to ensure the health facilities are functional and mothers get quality care.
“Closing HCIVs in the night has to with supervision. The HCIVs fall under local government and we urge the district leaders to ensure the hospitals are operating,” he said.
Last year, 19 percent of the deliveries occurred in HCIVs while 17 percent were in general hospitals and 8 percent were in referral hospitals. But many of the deaths (42 percent) were in the bigger referral hospitals, 38 percent were in general hospitals and 14 percent were in HCIVs. The remaining 5 percent were in HCIIIs and HCIIs, which always refer women with complications to higher facilities.
“For HCIIIs, the plan is to have doctors there and this means there are going to be theatres. We will first address issues in HCIVs and start handling HCIIIs where the distance to HCIV is long,” Dr Olaro said.
Dr Luswata said many HCIVs do major operations and yet they don’t have fridges and blood.
Challenges
“Ideally, any health facility that does an operation should have blood available at the facility. Sometimes they have to drive to pick blood from the regional referral hospitals but by the time you are back, the mother has already died. Sometimes they also refer the woman to higher health facilities and the woman ends up dying.
Every hospital that does major operations should have robust blood and transfusion services,” he said.
But Dr Olaro said this is being addressed. He appealed to Ugandans to donate blood.
“The [construction of] Soroti blood bank is ongoing and we are constructing another one in Hoima and Arua. The blood distribution point in Nebbi and Kabale is already ongoing. We are also going to set up another one in Moroto,” he said.
According to the 2020/2021 health sector performance report, maternal death rate has stagnated in the country at 92 per 100,000.
But the report states that in the last five years, the institutional maternal mortality ratio has reduced from 108 to 92 per 100,000 deliveries.
Recommendations
Dr Charles Olaro calls for family planning, which involves empowerment of women so that they make an informed decision on when they should have children. “We have been trying to increase access to family planning services and commodities.
We have launched a 2030 commitment where the government intends to increase modern contraceptive prevalence for all women from 30.4 percent in 2020 to 39.6 percent and reduce the unmet need,” he said.
Dr Mukuzi Muhereza said: “Educating a girl child is a way of family planning. An educated girl tends to have children much later in life and can decide whether to become pregnant or not,” he said.