In East Africa, a cancer diagnosis means a death sentence
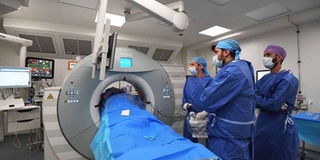
A radiologist and his assistants stand next to a cancer patient undergoing a scan after being injected with Argon at -120° around his tumour. AFP PHOTO
What you need to know:
- Statistics from the World Health Organisation show that the disease killed 7,662 Rwandans in 2018 and 10,700 new cancer cases were diagnosed. Breast cancer is the most prevalent, followed by prostate, cervical, liver and colorectum.
- Dr Sabin Nsanzimana, head of Rwanda Biomedical Centre, told The EastAfrican that health officials are concerned about the growing number of cancer cases.
At just 20 per cent, Uganda has one of the lowest cancer survival rates in the world, according to statistics from the Ugandan Cancer Institute. But, as the burden of the disease continues to grow in East Africa, experts say that addressing challenges of late diagnosis, a poor understanding of the disease and inadequate health infrastructure, including human resources, should be a key focus for governments.
Dr Peter Eriki from the African Centre for Global Health and Social Transformation in Uganda, said that ageing, social and economic determinants — including where and how people live, what they eat, urbanisation and industrialisation — have all contributed to the problem of cancer, and therefore, the approach, should aim at ensuring these risk factors are reduced.
He advocates the approach on Ebola: “We should tackle cancer the way we tackle Ebola: Present the message to the people in a language that they understand. We need to show them how the disease presents so that when people experience any abnormal symptoms, they are able to get care on time. What is happening now is that many people still cannot tell when they develop symptoms.”
Promoting routine screening for prostate cancer for men over 40 years would also go a long way in diagnosing the disease early enough and therefore being able to manage it. Women on the other hand should also be screened regularly for breast and cervical cancers.
“Now we have the technology to test. So if we catch the disease early, when it is still localised in one place, we are able to manage it,” said Dr Eriki.
He added that East Africa needs to develop common policies and messages on cancer and other communicable diseases. This way, experts across the region can help in drawing a common roadmap and campaign on managing the disease.
“The Uganda Cancer Institute was designated as a centre of excellence for cancer care in the region. We could use this status to work together and come up with the best way we want to tackle the disease,” he said.
According to Dr Samuel Guma, the vice-chairperson of the Uganda Cancer Society, a big part of Uganda’s cancer problem can be easily addressed by ensuring routine and regular screening because most of the common cancers are caused by viruses — which also mean that they are easily preventable and treatable.
Kenya
In Kenya, cancer (all types) is the third leading cause of death, accounting for seven per cent of the overall national mortality. Cancer of the oesophagus has overtaken cervical, breast, stomach and prostate cancers to become the leading killer, according to recent data from the National Cancer Control Programme. In 2017, breast cancer was the leading killer, followed by cervical, prostate and oesophagus cancer with experts blaming this on late diagnosis.
Dr Anne Ng’ang’a, head of Kenya's National Cancer Control Programme, says that in 2018, 4,351 deaths resulted from oesophagus cancer, followed by cervix uteri cancer at 3,286, breast cancer at 2,553, stomach (2,068), prostate (1,663), colorectal (1,463) and liver cancer (1,331).
Data shows that more Kenyan women than men die of cancer. The International Agency for Research on Cancers Globocan 2018 data shows that the disease claimed 18,772 women, compared with 14,215 men in 2018.
Dr Sitna Mwanzi, chair of Kenya Society of Haematology and Oncology, however, also said that more women go for screening than men, and thus lead in new cancer cases, with breast and cervix uteri cancers.
“Most women are not breadwinners and their husbands control the finances, so they may be sick but not have money to go to the hospital early. Also because these cancers affect private body parts, most women are still shy to seek treatment,’’ she explained.
Among men, prostate cancer is the leading killer, followed by oesophagus and colorectum cancers.
Among children aged zero to 19, leukaemia is leading at 16 per cent, followed by non-Hodgkin’s lymphoma at 15 per cent, kidney 6.4 per cent and others at 44 per cent.
In the next five years, Globocan data projects the incidence of cancer in Kenya will increase twice as fast in women as in men.
Tanzania
In Tanzania, 50,000 women are diagnosed with cervical cancer annually, with statistics from the Ocean Road Cancer Institute (ORCI) showing that there has been an increase in cancer patients year on year: In 2015 there were 5,764; 6,338 in 2016; 7,091 in 2017, and 7,649 recorded in 2018.
According to the Health Ministry, cervical cancer accounts for 36 per cent of all cases, followed by breast cancer (12.9 per cent), cancer of the oesophagus (9.8 per cent) and Kaposi Sarcoma (9.3 per cent).
Dr Crispin Kahesa, director of cancer prevention services at ORCI, says that around 52,000 people are diagnosed with cancer annually, and 70 per cent of them visit the hospital when the cancer is at advanced stage.
Dr Kahesa said cervical cancer is the leading killer in women, followed by breast cancer, while Kaposi sarcoma leads among men, followed by cancer of the oesophagus.
Tanzania’s Minister for Health Ummy Mwalimu said the ministry is focusing on awareness campaigns to have more people go for screening. Tanzania plans to launch the National Cancer Treatment Guidelines this year, to guide cancer testing and treatment services.
The government will also establish centres at the Mbeya Zonal Referral Hospital in Mbeya region and at the Benjamin Mkapa Hospital in Dodoma to supplement the work already being done in Kilimanjaro Christian Medical Centre and at the Bugando Medical Centre in Mwanza.
Tanzanian offers free cancer care, including screening, hospitalisation and treatment.
Statistics from the World Health Organisation show that the disease killed 7,662 Rwandans in 2018 and 10,700 new cancer cases were diagnosed. Breast cancer is the most prevalent, followed by prostate, cervical, liver and colorectum.
Dr Sabin Nsanzimana, head of Rwanda Biomedical Centre, told The EastAfrican that health officials are concerned about the growing number of cancer cases.




