Hepatitis: The silent killer overtaking HIV, malaria
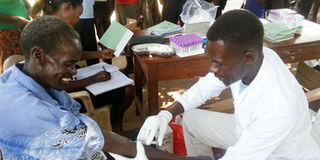
Prevention. A resident undergoes Hepatitis B screening during the launch of the emergency vaccination campaign in Dokolo Town, Dokolo District, in 2018. PHOTO BY BILL OKETCH
What you need to know:
Consequence. Ignorance and poor funding have seen the viral disease continue to wreak havoc on society
At the beginning of March, 20-year-old Jennifer’s longtime dream of moving from the village for a better life in the city came to a dramatic end. In the said month, Jane was hired by a family in Seeta, Mukono District, to work as a maid.
Prior to commencement of her duties, however, the family subjected her to both HIV and Hepatitis B tests. Jennifer’s test results taken at Mukono Church of Uganda Hospital returned HIV negative and Hepatitis B positive.
Cooking and caring for a six-month-old baby would have been Jennifer’s duties but the family declined to hire her after receiving her Hepatitis B positive results, fearing that she could infect them and the baby. Jennifer was thus unfit for work. She was given Shs120,000 to facilitate her movement back home in Kaliro District and also seek treatment.
“I consulted a doctor who told me that Hepatitis B is very contagious. I could not risk my baby like that,” Ms Doreen Nalwanga, who had hired Jennifer, said.
Dr Jackson Amone, the commissioner of clinical health in the Ministry of Health, said in an interview that viral Hepatitis can be transmitted from a mother to their new born child through sex or by pricking oneself with something infected with the virus.
Transfusion of blood infected with Hepatitis B, he says, is also another way through which the viral disease is transmitted.
“And maybe when children are playing and one has the disease, it can be spread to others through saliva. Sometimes when you go to a barber, the disease can also be transmitted through unsterilised machines used to cut hair,” Dr Amone says.
Rising cases
Jane’s case, according to Dr Allan Katamba, the in-charge of health services in Kaliro District, is not unique as many residents in the district have been diagnosed with the disease.
“We had an outbreak in the district just like it was in the whole country,” Dr Katamba said, highlighting the scale of the problem. “But we are now vaccinating people [against hepatitis B] and vaccines are there,” he added.
Hepatitis, according to the World Health Organisation (WHO), is an inflammation of the liver. There are 5 main hepatitis viruses, referred to as A, B, C, D and E. However, the most fatal ones are hepatitis B and C, which normally cause liver cancer.
Mr Kenneth Kabagambe, the executive director of the National Organisation for People Living with Hepatitis B (NOPLHB), says the scale of Hepatitis in the country is not known since a few people have been tested.
Like most developing countries being ravaged by Hepatitis, access to test kits and treatment is not adequate making the disease to thrive. Part of the problem for the inadequacy, Mr Kabagambe says, is underfunding to the health sector.
“Unlike HIV, where many health centre will diagnose it and offer services, Hepatitis is specialised and there are few centres screening it. Most of the rural populations do not have these services,” Mr Kabagambe says.
“We need to create awareness about Hepatitis, increase screening because this is a serious health problem,” he adds.
Ministry of Health records shows that government has been spending at least $3 million (about Shs10.9b) annually since 2015 to offer free hepatitis screening and creating awareness.
Vaccination schedule
Dr Alfred Driwale, the manager at Uganda National Expanded Immunisation programme, says since government has been offering free vaccination against the disease, adults who start on vaccination should take all the three or four shots in six months to guarantee that they are protected against the disease.
“But for children under 17 years, they do not need to go for hepatitis screening or vaccination if they underwent routine immunisation offered at birth. Hepatitis B was incorporated in routine immunisation in 2002,” Dr Driwale says. He adds that all government referral hospitals have hepatitis B vaccines “as it is a policy by government to offer free vaccination and treatment”.
In cases where there are vaccines or medicine for treatment stock out, it is when hospitals ask people to buy, he added.
State minister for Primary HealthCare Joyce Moriku recently said Uganda was registering tremendous progress in the fight against Hepatitis.
She said the disease prevalence had dropped from 10 per cent nationally in 2015, to less than 5 per cent.
“…we have made a big stride in terms of treatment and vaccination. Previously, it [disease prevalence] was 10.3 per cent but the current prevalence is 4.5 per cent,” Dr Moriku said.
To make Hepatitis awareness, testing and treatment affordable, drug manufacturer Gilead waved off its patent rights to different other companies to make generic drugs, which are cheaper for developing countries, including Uganda.
“It is one way of giving back to the community,” Mr Akram Bouchenaki, Gilead Sciences Director of Access Operations and Emerging Markets: North and West Africa, told Daily Monitor in the Egyptian capital Cairo last month.
“We are working on a cure and we are hopeful. We have been able to find a cure for hepatitis C, it is the first time to have a cure for a virus,” said Dr Papa Salif Sow, Gilead Sciences Vice President of Program Development and Management, Access Operations & Emerging Markets: Africa/Geneva.
Global campaign
The pharmaceutical company partnered with the Confederation of African Football (Caf), the organisers of Africa Cup of Nations, to raise awareness about the disease in the just concluded African Cup of Nations tournament held in Egypt.
Countries with highest prevalence are South Sudan at 22.38 per cent, Swaziland with 19 per cent, Liberia at 17.8 per cent and 14.35 per cent for Zimbabwe, according to available data.
“If you have never tested for hepatitis and thus living in the dark, hurry and know your status,” says Mr Kabagambe.
“If you are negative, get vaccinated against the disease, and if you are positive, ask your doctor whether you are you eligible to start on treatment,” he adds.
Mr Kabagambe speaks from a point of experience having been diagnosed with the disease in 2012. And those on treatment, he said they should have hope “as having hepatitis is not the end of your dreams”.
Prevalence rate
Chronic viral Hepatitis, according to WHO, kills more people in Africa annually than Tuberculosis, malaria or HIV. WHO estimates that about 780,000 people die each year due to consequences of hepatitis B such as liver cirrhosis and liver cancer.
A survey by the Ministry of Health in 2016 indicated that Hepatitis B infection among adults stood at 4.3 per cent with the disease prevalence being highest in men at 5.6 per cent. In women, it stood at 3.1 per cent.
Northern Uganda had the highest prevalent at 4.6 per cent and lowest in South West region at 0.8 per cent. The ministry data still indicates that 23 million Ugandans have been screened for Hepatitis, of whom 17.6 million have been vaccinated since 2015.




