Cancer, the growing silent killer among the Ugandan population
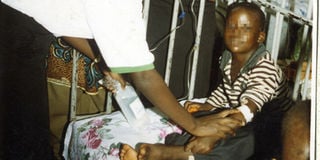
A child with cancer in hospital. Burkitt’s Lymphoma, a cancer that affects children is one of the common ones in Uganda.
What you need to know:
Having dedicated October as a month to focus on cancer, we have been running stories on various types of the disease focusing on the causes, treatment, statistics and methods of prevention. As we wrap up our series, we look at the state of cancer in the country. Over the years, cancer has become more common with one in 500 people suffering from one type or another, a warning that if you have not yet checked or had screening for those types that can be screened, you should.
“The body is made up of small building bricks called cells. The cells have been programmed inherently, that they must grow to a certain age and size and they must die. These cells either by an infection or genetic mutation begin to grow the wrong way. Ultimately, this cell will grow without stopping or dying and continue to accumulate and eventually form into a tumour.” This is the layman definition of cancer by the Specialist Medical Oncologist at the Uganda Cancer Institute (UCI) Abrahams Omoding.
Dr Omoding says that for some cancers like that which affects the skin, it could take up to 10 years for the disease to manifest itself into a tumour, in most cases presenting itself when already in late stages.
For other cancers like Kaposi’s Sarcoma, prostrate, cervical and Burkitt’s lymphoma, much as signs and symptoms may present themselves a bit early, the doctors at the UCI collectively attest that up to 80 per cent of patients come in their late stages of the disease and can hardly get cured, hence eight in 10 patients diagnosed with cancer die of the disease because of late diagnosis.
And this is the disease that is slowly eating up the Ugandan population, with at least one in every 500 people suffering from a cancer, the Head of UCI, Dr Jackson Orem, said. That figure is rather worrying. Statistics, doctors say, have shot up recently due to many factors ranging from an increase in infectious diseases in the region, changing lifestyles and perhaps an increase in awareness among the population who can now report cases at the hospital rather than die unnoticed in shrines and the like.
“Because we are in the tropics, it is an infection epidemic region and majority of the cancers are infection related like Kaposi’s Sarcoma, Burkitts Lymphoma, Cervical cancer and cancer of the liver. Most infections are potentially preventable through vaccination but we do not have a robust vaccination programme.
“We do not have a robust screening programme that rolls out screening. Screening plays a vital role because it enables one to detect the disease early,” explains Dr Omoding.
Burkitt’s lymphoma and Kaposi’s sarcoma are for instance 90 per cent associated with the HIV/Aids virus. Cervical cancer is associated with the Human Papilloma Virus, which is also sexually transmitted. Cancer of the liver has everything to do with Hepatitis B, which is an infectious disease.
Even then, not all cancers are infection-related. Worse still, Dr Omording says, some cancers like prostrate, liver and breast tend to occur at a younger age in blacks and progress faster compared to the whites.
“There are speculations of genetic differences, environmental differences and too many infections. It is possible our immune system is weakened by these infections like malaria so we develop the cancer earlier,” he says.
With all these risk factors, the county’s readiness to combat Non Communicable Diseases (NCDs) or even handle cancer as a serious ailment remains questionable, with the population largely unaware of this growing epidemic, which combined with other NCDs like heart ailments, diabetes and chronic chest diseases constitute 60 per cent of the total deaths in a year.
There is currently no national policy on cancer and its screening like it is with immunisation or malaria and neither are lower health centres and even some district hospitals and their equivalent medical personnel equipped to diagnose the different cancers.
Only the Uganda Cancer Institute is fully equipped to screen for the disease and yet it can only cover part of Kampala in its community screening, leaving the institute stretched beyond capacity with an inflow of patients from all over the country.
In fact, it is not uncommon to find patients camping at the institute for months just to get hold of a doctor and yet when diagnosed, they can hardly pay for subsequent tests of about Shs20,000 each. The minimum cost of treatment is about $500 (about Shs1m), but this could rise to $1,200 (about Shs2.4m) depending on the severity of the cancer diagnosed.
The head of the UCI, Jackson Orem, has time and again decried the little funding to the institute which has left many diagnosed unable to complete their doses because neither the institute nor the patients can afford to pay for the expensive medicine.
Indeed, the Principle Medical Officer for Non-Communicable Diseases at the Ministry of health, James Sekajugo, agrees that NCDs and cancer in particular have not yet been fully attended to by the government as they should.
“We are justifiably alarmed by infectious diseases because they kill people at a very high speed. The NCDs are killing one person or two but very steadily, the people who have died of them are more than HIV/Aids, Malaria, TB and maternal conditions put together,” Dr Sekajugo says, adding that NCDs are responsible for 60 per cent of deaths globally.
“As time goes and as the country develops, the intention is to have screening at all health centre IVs and I think we need to now approach the NCDs through prevention.
“Our biggest challenge remains funding and right now heart and cancer institute is overloaded because lower levels are not doing what they are supposed to do,” he adds.
Thus, with cancer screening as expensive as Shs70,000 in private hospitals, limited awareness of the disease among the population and no government plan to combat the disease, cancer remains at large, slowly but steadily killing more Ugandans.




