She survived breast cancer and gave birth to quintuplets
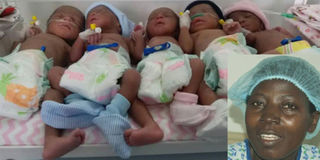
Nakato (inset) while still in hospital after giving birth to her babies on September 9. Courtesy photo
In July 2014, Honoranta Nakato, 44, a secondary teacher in Kayunga, noticed a lump in her left breast but did not think it was dangerous.
“My husband noticed it too and he asked but I did not get concerned because it was not painful and my life continued normally,” she says.
In October, the lump was enlarging and when she went to ask one of her sisters, they all got scared and advised her to go to Uganda Cancer Institute immediately because they suspected it would be cancer.
“My elder sister had breast cancer and completed her treatment in 2002. With this background, they told me to immediately seek proper diagnosis from the cancer institute,” she recalls.
At the UCI, Nakato’s siblings knew about Dr Victoria Walusansa who recommended that she sees an oncologist. She was told to do several tests including a biopsy at a laboratory at Wandegeya but does not remember how much the tests cost her.
After two weeks, the results confirmed that she had breast cancer. This was sad news for her but luckily, it had not spread to the other parts of the body. Her older sister had cancer so it was not shocking news for her but she still feared for her life. The doctors recommended that she starts treatment immediately.
Instead of going to hospital for the strange growth on her body, Nakato went to consult her sisters instead.
She says, “I had gone with my sister for support and I saw the people who were suffering from cancer and with the counselling, I got the courage that it was not only me that was suffering from cancer.”
In some cases, patients with breast cancer are first operated to remove the cancer tumour but she started with chemotherapy because the doctor had said it would help kill some of the cancer cells before they spread to other parts.
The nightmare of getting treatment
“I would get a dose of chemotherapy through the intravenous after every two weeks but while seated on a plastic chair or a bench because of the overwhelming number of patients at the institute,” she says.
She lost her hair, nails and palms turned black, got nausea and her body was weak every time she would get the dose. Sometimes there would be stockouts and would be referred to Friecca Pharmacy in Wandegeya where she bought a dose at Shs400,000.
After three cycles of chemotherapy, Nakato was booked for an operation to remove her breast because if it was not removed, the doctor said, “the cancer cells would spread to the other parts of the body”.
“My third cycle was mid-December and the time I had to be operated on was about Christmas time but Dr Makumbi had said he would not be available at that time so I was booked for January 6, 2015,” she recalls.
She was discharged after the operation and she nursed the wound from home following proper instructions from the doctor for proper hygiene that would prevent her wound from becoming septic. In about three weeks, the wound was almost healed so she had to return to UCI for three more chemotherapy cycles.
She did not receive the last cycle on time because her immune system was weak. Her blood count was very low when she reported to UCI so she had to go home and return after two weeks for the treatment.
After chemotherapy, Nakato started radiotherapy (commonly known as kukalirira in Luganda) immediately. In this type of treatment, a patient is under radiation to help kill more cancer cells and also reduce the chances of the cancer spreading to other parts.
This was the time, however, when the radiotherapy machine at the UCI broke down so she had to wait until October yet she completed the chemotherapy in April 2015.
She says: “The radiotherapy would go daily from Monday to Friday for about 15 minutes each day but the machine kept breaking down so sometimes I would miss out. The doctors, however, would take responsibility and called me whenever the machine was okay. By the end of December, I had completed my radiotherapy treatment and would only go to hospital for review.”
Since Nakato had not had a child, after her treatment, she embarked on means to find a child and when she consulted the doctor on her possibility of giving birth, she was first given tamoxifen to prevent the cancer from spreading to other parts of the body and a six-month review. She first visited Women’s Hospital International and Fertility Centre in Bukoto in February 2016 for a consultation.
“I told her about what was needed but after a long time, I did not see her,” says Dr Ssali Tamale, the director of the hospital who was the lead surgeon during the delivery.
“Since all the trials I had made to conceive had failed, I considered going for an IVF but had to discontinue the tamoxifen because the doctor said it can increase the risk of congenital anomalies in the foetus,” Nakato recalls.
Two years later, she reappeared at the hospital ready for the procedure.
After diagnosis, Dr Ssali realised that Nakato had blocked tubes due to the miscarriage and so her chances of conceiving naturally were very minimal.
He says: “We then got six eggs from her uterus and sperms from her husband using the Intra Cytoplasmic Sperm Injection and left to fertilise to form an embryo.”
The process
The intra cytoplasmic sperm injection is part of an IVF treatment cycle where a single sperm is injected into each egg to assist fertilisation using very fine micro-manipulation equipment. After three days, six embryos had developed which were then transferred through a
catheter in the cervix using an ultrasound for accuracy into the womb.
For 33 weeks, 50 toes, 50 fingers and six hearts have been beating in one body until September 9, when Nakato went into labour.
The Ndeeba Senior Secondary School teacher from Kayunga finally had her prayer answered after 22 years of childlessness, after suffering a miscarriage immediately after she got married. After she suffered a miscarriage, she failed to conceive again and had tried endless options, including going to several doctors in vain.
Nakato now wears a smile of excitement about the first miracle babies in East and Central Africa after an in-vitro fertilisation (IVF).
The transfer of the embryo was done on February 9, 2018 and they were all transferred bearing in mind that sometimes the embryos shrink. On March 6, when a scan was done, the doctors noticed that she had five babies.
In multiple pregnancies, Dr Ssali says, some foetuses shrink from the womb and a few remain but in Nakato’s case, they all continued.
“In the medical school, we are taught that you can reduce the number of foetuses for fear of the mother miscarrying but being a Christian, I refused to terminate a baby. I left them to live,” Dr Ssali says.
Risks involved
He adds: “If the uterus becomes overloaded, the cervix opens so the mother is at risk of losing the babies. We usually recommend a stitch to close the cervix but this was not the case with Nakato. Hers remained closed despite the five babies.”
When she was first told that she had five babies, Nakato says: “I was very shocked because I had not heard of such a thing. I heard women having quadruplets but not five. I feared I would not be able to carry them but with the counselling from the doctors, I learnt to accept it.”
After conception, she went back and continued teaching.
“I followed the advice from the doctors and not even once did I fall sick during pregnancy. I stopped working at week 27 because the doctors recommended bed rest,” she says.
Nakato, unwilling to mention the amount of money it cost her to have this particular IVF treatment, Dr Ssali highlights that the cost of undertaking an IVF depends on a number of factors but the whole process may cost about $5,000 (about Shs18.5 million). A couple may pay less or more, depending on the complexity of their cases.
On September 9, Nakato gave birth to normal quintuplets; three girls and two boys by C-section. Her twin sister Babirye also has five children but not through the IVF. Nakato’s right breast that remained can still produce some breast milk but it is not enough considering the number of her babies. She now has about three breast milk donors one of whom is her sister with a three months old baby.
“My sister comes here at the hospital every morning and evening to express the milk. She is the only reliable donor that I have for now. The other people still have little milk and it may not be enough for all the five babies. I still need more breast milk donors,” she pleads.
2004 IVF baby
In 2004, Dr Ssali Tamale delivered his first IVF baby. Since the inception of the Women’s Hospital International and Fertility Centre, more than 10,000 children have been born from these assisted reproductive techniques. Before 2004, there were fertility centres in Kenya, Tanzania and Uganda but none had made a baby.
The hospital started in his own flat in Bukoto and in the first year, he had 12 patients four of whom conceived, two miscarried and two carried on. One went to deliver in Mulago, the biggest national referral hospital because Dr Ssali did not have enough space.
IVF expectant mothers need no special treatment but she was tossed around and rejected because the midwives there said they did not know how to handle her. “This motivated me to expand and start a complete hospital,” he said.




