Prime
Govt to spend Shs900 on drugs a month per citizen
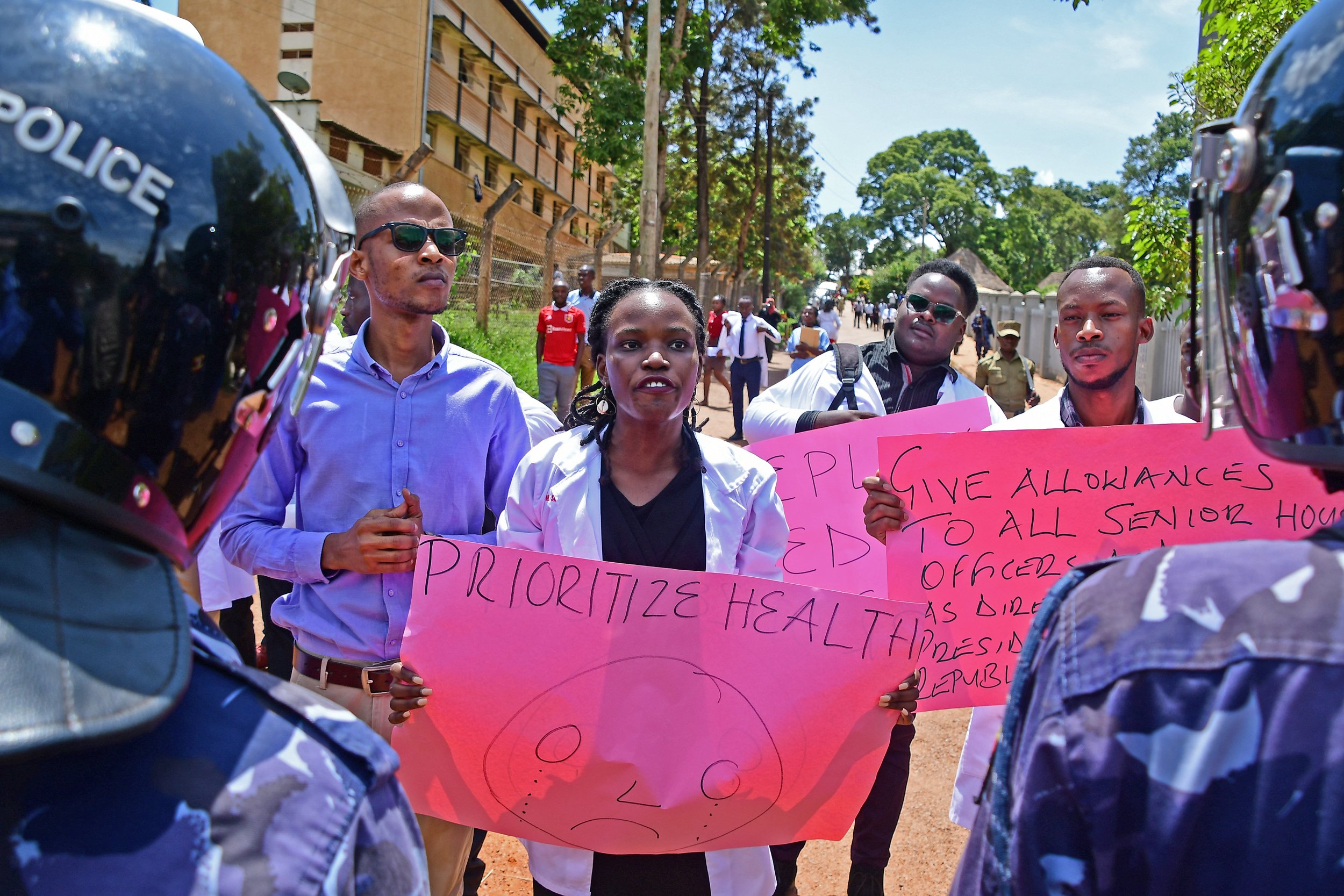
Medical interns hold a peaceful protest at the College of Health Sciences in Mulago on June 7. Their planned march to the President’s offices in Kampala to deliver a petition over their delayed deployment was stopped by police. PHOTO / ABUBAKER LUBOWA
What you need to know:
- The Shs900 figure is an average computation based on population, but actual drugs and commodities available to patients may be more because not all Ugandans will over the next twelve months fall sick or require the medicines budgeted to be procured.
The government has increased the budget for procurement of drugs and health supplies in the next financial year, which starts on July 1, by Shs69b.
The 2023/2024 Budget was increased from Shs431b to Shs500b.
The allocation means the government will on average spend Shs11,000 on medicines and health commodities over the next 12 months, or Shs917 a month, per each of the 45.6 million citizens --- an allocation health and civil society sector players decry as paltry.
Uganda Bureau of Statistics (Ubos) in its report titled, National Mid-Year Population Projections of Uganda released on May 26, 2022, projects the country’s population will gross 45.6 million by this month, the eve of the operation of the new budget.
At least thirty percent of the Shs500b, according to Ministry of Health, is expected to be used to buy a portion of anti-retroviral drugs (ARVs) that annually cost Shs1 trillion to treat 1.4 million HIV-positive Ugandans.
The questionable allocation for drugs and medical supplies in the new budget comes on the back of reduction of donor support to Health sector over the years, most notably contribution to HIV/Aids care that went down by $9.9m (Shs36.4b) between 2020 and 2022. $6m (Shs22b) out of this was Global Fund contribution, raising questions about sustainability of support to HIV/Aids treatment at a time a main funder such as the United States is threatening to cut financing over the new anti-gay law.
Health ministry declined to comment on the implication of the allocation of Shs900 for drugs and medical supplies per citizen per month on the eventual quality of curative care, referring our inquiries to the National Medical Stores (NMS) that we were unable to reach by press time.
The Shs900 figure is an average computation based on population, but actual drugs and commodities available to patients may be more because not all Ugandans will over the next twelve months fall sick or require the medicines budgeted to be procured.
The overall allocation to the health in the Shs52.7 trillion programme-based budget read yesterday, like the sector allocations in the past, is below the commitment that Uganda, like other African countries, made in the April 2001 Abuja Declaration to dedicate 15 percent of national Budget to Health.
The Initiative for Social and Economic Rights (ISER), a non-profit organisation, in a position paper noted that “despite the existing gaps in health service delivery, the budget towards the health sub-programme is being slashed by 11.8 percent in the [the new budget]”.
“Provisional allocations towards health in the Financial Year 2023/2024 stand at Shs4.1 trillion down from the 4.7 trillion approved for the Financial Year 2022/2023,” ISER wrote.
The health sub-programme has many institutions, each with their own vote and other allocations are jointly implemented by other sub-programmes.
This Shs4.1 trillion, represents around 7.8 percent of the national budget, contrary to Abuja Declaration signing on resourcing required for equitable and universal access to healthcare.
Ms Noor Musisi, the deputy executive director for programmes at the Centre for Health, Human Rights and Development (CEHURD), said the government should commit more domestic resources to the health sub-programme.
“What we have been provided as health is not the amount that we want to actually receive. I have been attending [health] facilities and you already know that we have challenges in remuneration of health service providers, we have challenges with availability of essential commodities like drugs and blood,” she said.
Ms Musisi added: “We know much of this money is coming from development partners. What we need to do, as the government, is commit more money into the health sector and the money should come from domestic sources.”
Our analysis of the expenditure estimates show that Uganda Blood Transfusion Services will roughly get Shs21.8 billion, less than the 23.6b it was allocated in the ending financial year, prompting some activists to warn that the reduction spells danger for children, expectant women and accident victims who need transfusion most.
Ms Musisi said beside issues of corruption and reported drug thefts, there are also challenges in the distribution of medicines and other health commodities.
“So we are not performing that well [as health sub-programme],” she said.
However, Finance minister Matia Kasaija, while presenting the budget yesterday, said the government takes health services delivery – which on paper is one of the principal anchors of the budget focused on human capital development - as important and outcomes are improving.
“Access to healthcare by Ugandans remains a key priority. Consequently, 381 health centre IIs have been upgraded to health centre IIIs,” he said, adding that 250 health centre IIIs have also been upgraded to health centre IVs and equipped, and are now functional.
“Construction and equipping of 31 new Health Centre IIIs in sub counties without any health facility is 90 percent complete. The health referral system has also been enhanced by fully functionalising 143 Intensive Care Units (ICUs) and 5 High Dependency Units (HDUs) in National and Regional Referral Hospitals across the country,” he added.
Next year, Mr Kasaija said, the Mulago Super Specialised Hospital and the new state-of-the-art Intensive Care Unit at the Uganda Cancer Institute will be fully operational.
“They will provide specialised care to all Ugandans and reduce medical referrals abroad. In addition, all existing health centre IVs and health centre IIIs will be facilitated to offer quality healthcare to all Ugandans,” the minister added.
In this respect, he noted, health worker supervision and management will be strengthened to reduce absenteeism.
“After the ongoing audit of the payroll, the ban on health worker recruitment will be lifted. Government will in the next few weeks resolve the plight of medical interns and doctors designated as senior house officers, in view of their important role in supporting the healthcare system,” Mr Kasaija said.
He added: “In the meantime, I have provided Shs22.6 billion to clear outstanding arrears for medical interns and senior house officers for the financial year ending June 2023.”
However, the Health ministry said they need Shs80 billion committed by Finance Ministry for paying medical interns before medical graduates can be deployed for mandatory internship.
Finance did not pronounce itself on how the funding deficit will be covered.
Time frame
The health sub-programme, according to the national budget strategy, will, in the next 12 months, focus, among others, on the mobilisation of resources for immunisation and sustainability of maternal testing and maternal anti-retroviral therapy coverage at over 95 percent.
Other areas of focus include increased retention on the treatment of positive pregnant and lactating women, prevention of new infections among young previously HIV-negative women and improving adolescent health services and fast-tracking of the approval and implementation of the adolescent health policy.
The country has around 1.4 million people infected with HIV, with a large chunk of their medicines (around 80 percent) bought by the US President’s Emergency Plan for Aids Relief (PEPFAR). PEPFAR gives Uganda around $400 (Shs1 trillion) annually to combat the disease and support people affected by HIV/Aids.
Uganda, according to information from the government, is contributing Shs150 billion in the next financial year, up from Shs100 billion in the previous years, for life-saving ARVs.
Dr John Kamili, a pharmacist who has worked with Cipla Quality Chemicals, a local pharmaceutical, said donors like PEPFAR buy medicines locally available from foreign industries, leaving Ugandan manufacturers such as CIPLA in the cold.
“We have approved products, but access to the market is still a problem. Procurement programmes by [donors] do not harness the regional manufacturing process. They [donors] still protect their manufacturers as we are locked out,” he said.
Dr Charles Ayume, the head of the Parliament Committee on Health, said the country is consistently increasing its budget for ARVs.
“This year there has been an increment of Shs50 billion towards anti-retroviral medicines. That money is not enough, but the government is committed to increasing the budget for HIV/Aids response,” he added.
However, Dr Gerald Mutungi, the assistant commissioner for Non-Communicable Diseases (NCDs) Control at the Health ministry, said drugs for common diseases like hypertension and diabetes are not being provided in sufficient quantities due to limited funds.
“Medicines for these diseases are very expensive and are for life in most cases. Quite often, you (a patient) go to a health facility and you find that they are out of stock. They give you a prescription to go and buy from outside,” he said, adding: “The population should screen for NCDs and be physically active to prevent these diseases.”
Dr Mutungi, however, said the budget for NCDs is slowly increasing.
Activists have in recent weeks been urging the government to expedite plans for the National Health Insurance Scheme to promote universal access to care.
Besides HIV/Aids and NCDS, the health sub-programme, according to the information from the Finance Ministry, will also continue training health workers on integrated management of childhood illness.
The programme will maintain medical equipment and recruitment of biomedical engineers and improve infrastructure including staff accommodation.
Biomedical engineers are meant to work on medical equipment. The country has had issues with non-functional machines in hospitals and 40 essential machines at Mulago Hospital are dead, the Auditor General report and other government officials reported.
The hospital management said the beak-downs are periodic and the machines are being repaired.




