Artificial eyes giving recipients a new outlook on life
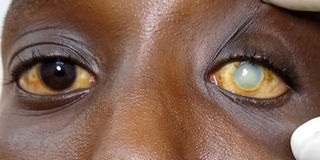
A patient with a problem in their right eye. Photos by Esther Oluka
On a Friday afternoon, Dr Franklin Wasswa, 34, engages with Micheal Kihumuro, a patient, about artificial eyes. At one point, he stands up, removes the bandage covering Kihumuro’s right eye socket and closely examines it before carefully placing it back.
Kihumuro, a student, had an operation performed on his right eye in 2019. This was after previously suffering from a tumour in the eye’s orbit. The problem started in 2018 after the eye began itching and was sensitive to bright light.
Overtime, the same eye began swelling and evetually lost vision. So, doctors advised Kihumuro to undergo surgery so that the eye is removed. After the operation, Kihumuro was eventually referred to Dr Wasswa who specialises in making and fitting custom-made ocular prosthetics (artificial eyes) for any condition that has led to eye loss.
He is referred to as an ocularist.
And on this day, Kihumuro was here for a consultative visit to get more details on the particular artificial eye Dr Wasswa was planning to make for him.
Besides patients who have lost eyes to tumours, Dr Wasswa also makes artificial eyes for those who have blind and disfigured eye balls, those who have lost eyes as a result of cancer as well as individuals whose eyes have been affected by other kinds of trauma.
How are they made?
Usually, the process of making prosthetics involves taking an impression of the affected eye’s socket using delicate material such as alginate. The artificial eye is then made using high quality materials while following precise measurements.
The process involves painting and corresponding colours to look like that of the natural eye.
In the end, once the artificial eyes are completed, they is fitted onto the eyes. Where needed, adjustments are made.
The most important thing to note is that the artificial eyes are visionless, meaning one will still not be able to see once they are fitted. “Like other ocularists, I make the eyes for my patients in order to help them fight stigma that comes with eye loss,” Dr Wasswa says.
Overall, the prosthetics help reduce tendencies of defining victims by the loss of their eyes. For example, Kihumuro says people constantly stare at him. Sometimes, they discriminate against him, which has left him with psychological trauma.

After. The patient after an artificial one has been fixed inside their socket.
“I feel terrible at times when people treat me differently,” he says. And that is why he cannot wait to wear his artificial eye. At least then, it will create the illusion of having a real eye.
Inspiration
From a tender age, Dr Wasswa dreamed of studying medicine and in 2006 after enrolling for a Bachelor of Science Technology, he dropped out after one semester and embarked on chasing his dream.
With financial support from his parents, he left for the United States in 2007. In the US, his Senior Four and Six results were weighed according to the American education system and he was advised to enroll for a few courses to boost his already acquired Ugandan academic credentials. Afterwards, he sat pre-entry examinations before finally being accepted to Washington University for a doctorate of medicine.
“The programme introduces students to the different facets of human medicine,” he says, adding,
“I later learnt that the American course I had enrolled for was an equivalent of Bachelor of Medicine and Bachelor of Surgery in Uganda.”
While studying, he met a doctor who said he was an ocularist. “I remember him briefing me about his profession and immediately becoming fascinated,” Dr Wasswa says.
Days later, Dr Wasswa paid a visit to the doctor’s workplace where he got to see first-hand what the profession entails. “And that is how I became interested in making artificial eyes.
Besides, there were very few ocularists in Uganda so I knew becoming one would bridge the gap,” he says.
Another source of inspiration for the profession came while growing up, when he was still staying with his parents.
“I recall reading a book that had a story of a baseball player, a child with an artificial eye. I was moved by that story,” he says, adding “I kept telling myself that when I grew up I would end up helping patients with eye problems and that included making for some of them artificial eyes.”
Upon finishing medical school in 2017, he returned to Uganda to put into practice his acquired knowledge and skills. Now, he works as an ocularist based in Entebbe town and at Kisiizi Hospital, a community healthcare facility in Rukungiri District.
Rewards
Dr Wasswa gets satisfaction knowing that he is part of boosting a patient’s self-esteem, especially children.
Why children?
“Adults cope better than children when it comes to disability. Children are traumatised because of the bullying they encounter in school and overall, they are too young to understand certain issues,” he says, adding, “Artificial eyes reduce the challenges children face, especially discrimination and stigma in schools.”
Cost
The eyes are reasonably priced costing less than Shs1m. For some special cases, the artificial eye is made and then given to the patient who then makes payment at a later date. This is mostly in cases where patients are facing financial difficulties.
Dr Wasswa’s care tips
Cleaning the surface of the artificial eye varies at intervals from daily removal to once a year. This depends on some factors including individual requirements and the advice of one’s ophthalmologist.
Once inserted into the eye, the average removal of the prosthesis is once every two to three months. Patients who are able to wear artificial eyes for longer periods of time without removal, usually have the least amount of trouble.
Never touch the prosthetic eye with your fingers unless yu have thoroughly washed your hands with soap and water as bacteria and germs may cause conjunctivitis and socket infections.
How to insert eye
Wash the prosthesis using hot water and non-scented soap.
Then, hold the eye between your thumb and middle finger.
Lift the upper lid with the other hand.
Gently, slide the top of the prosthesis under the upper lid.
Finally, hold the eye in place with your index finger as you pull down the lower lid with your other hand.
Removing the eye
Without the suction cup ( pull down the lower lid with your index finger, look up and allow the eye to slide out over the lower lid).
With a suction cup (wet the cup, squeeze the stem, and press it against the eye. Relax the squeeze and confirm the cup grips. Hold down the lower lid as you tilt the eye out and over the lower lid).




