Don’t work without protection, UMA tells health workers
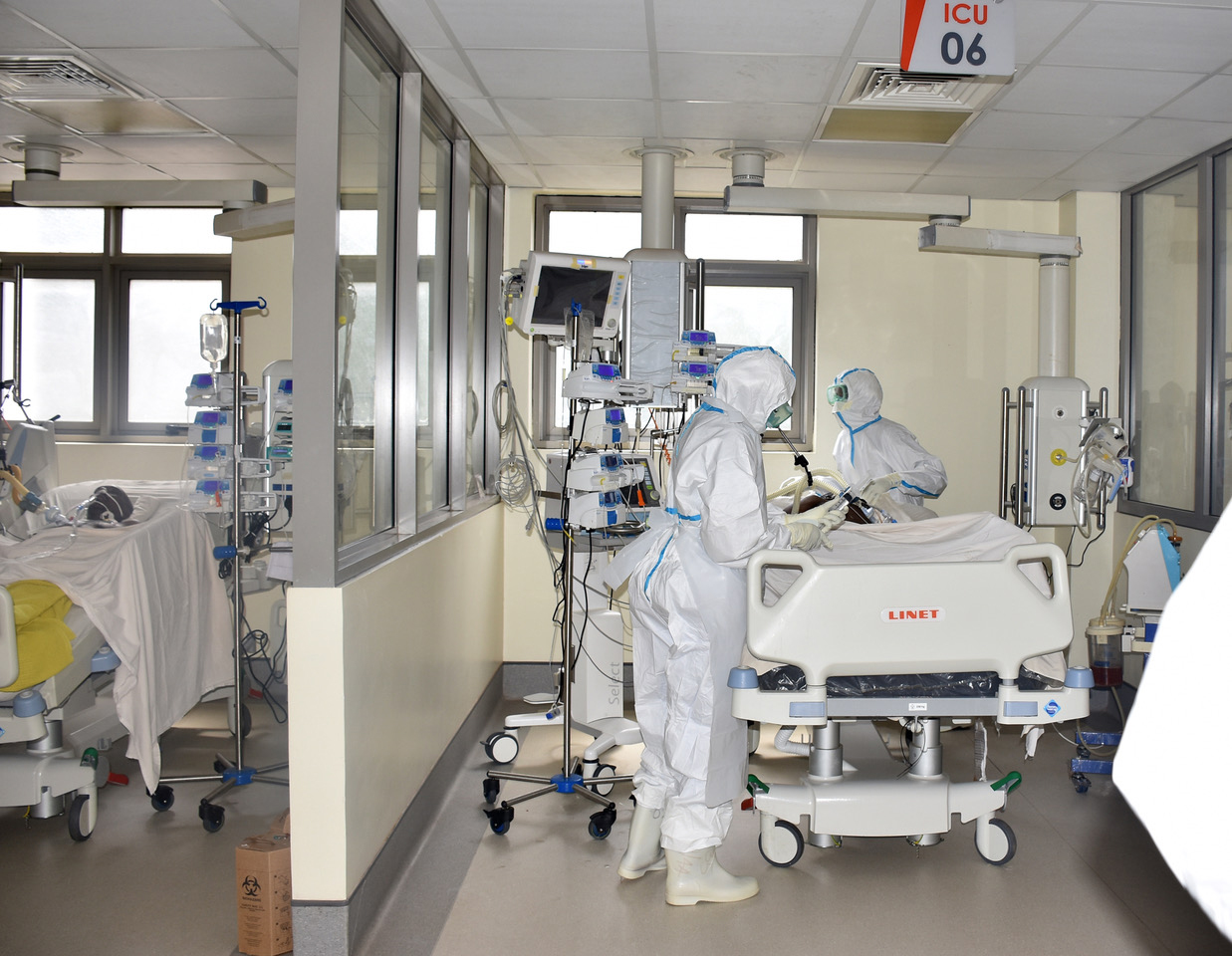
Medics attend to Covid-19 patients in the High Dependency Unit at Mulago Referral Hospital recently. PHOTO/PROMISE TWINAMUKYE
What you need to know:
- UMA suggested decongesting outpatient clinics to not more than 20 patients and also increase intervals between follow ups.
In a bid to enhance protection and care of health workers, doctors under their umbrella Uganda Medical Association (UMA), have urged health workers not to work without appropriate protection.
Dr Richard Idro, the president of UMA, said Covid-19 has exposed the vulnerability of health workers in the country, with a number of them getting infected in the line of duty while others have died.
“The cost of care is enormous and unaffordable by nearly all. Those dying in Intensive Care Unit (ICU) have left behind huge hospital bills that will cripple their families for long. It is very sad that doctors who provided such care when they were well may be unable to access it when they are ill,” Dr Idro said.
Since March last year when the country confirmed its first Covid-19 case, more than 3,000 health workers have been infected with Covid-19, according to UMA.
Many of these were registered in the second wave that the country started experiencing since May.
In June, the country lost 16 doctors to Covid-19 whereas several others are still fighting for their lives in High Dependency Units (HDU) and ICUs and many more are still getting infected, according to UMA.
Some health workers say the biggest problem causing the rise in the number of infections among health workers is shortage of personal protective equipment (PPEs) despite the government saying it provided the equipment.
As of July 18, Uganda had registered a total of 90,910 Covid cases, with 6 9,377 recoveries and 2,412 deaths.
Most of the health workers that the country has lost were senior doctors, with comorbidities. UMA has called upon all stakeholders to immediately take pregnant staff and health workers with comorbidities off routine and direct patient contact.
Dr Idro says such staff should be away from acute or emergency areas where the possibility of contact with patients with unknown Covid-19 status is higher.
“We can consult our seniors by telemedicine and reduce their contact with patients to a minimum,” Dr Idro said.
Health workers have been urged to postpone all elective (non- emergency) cases whenever possible as a way to decongest health facilities.
UMA suggested decongesting outpatient clinics to not more than 20 patients and also increase intervals between follow ups.
“For instance a clinic nurse may use telephone consults where possible until this Covid wave reduces. In the wards, have no more than one attendant per patient and all must wear masks,” the UMA statement reads in part.
Health workers have been advised to re-arrange duty work shifts.
Hopeful
Recommendations
•Every health worker should ensure they urgently receive the Covid vaccine.
•Use appropriate PPEs and always.
•Observe Infection and Prevention Control (IPC) measures.
•Assist poor health workers facing behaviour, attitude, and structural challenges to access health care (address the issue of stigma, dedicate ward space for health workers with Covid-19, among others).
•Urgently decongest outpatient clinics.
•Encourage health workers to rest enough, exercise for self-care and mental health.
•Create a doctors Covid-19 emergency fund.
•Severely ill health workers should be transfered to better facilities for advanced care.





