Prime
Experts caution govt as Ebola cases soar
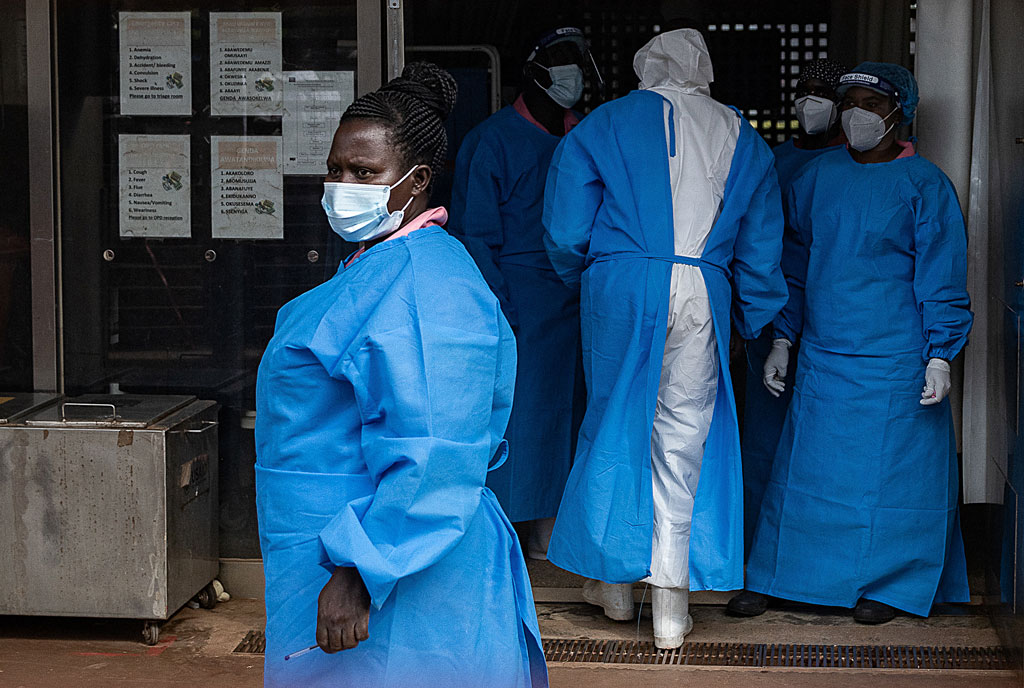
Members of the Ugandan Medical staff of the Ebola Treatment Unit stand inside the ward in Personal Protective Equipment (PPE) at Mubende Regional Referral Hospital in Uganda on September 24, 2022. PHOTO/AFP
What you need to know:
- The experts say improving Ebola diagnosis should come hand-in-hand with timely conveying of information to the public.
Health experts have asked the government to bolster access to Ebola testing, reduce turnaround time for the results and fix gaps in community engagement to curb the rising infections and deaths.
Thirty-five confirmed Ebola cases and seven confirmed deaths had been registered in the country by Saturday, representing a sharp increase from one confirmed case and death last Tuesday as per the Health ministry.
Speaking in an interview at the East Africa Healthcare Federation conference in Kampala on Thursday, Prof Khama Rogo, the former head of the World Bank Group’s Health in Africa Initiative, said improving Ebola diagnosis should come hand-in-hand with timely conveying of information to the public.
“The government must provide information, do quick and accurate tests, and inform people quickly. When tests are not done in time and information is delayed, the disease spreads,” he said.
Ebola presents with symptoms that are similar to that of other diseases such as malaria and diarrhoea. This increases the risk of giving wrong treatment to the patient, which eventually leads to death.
It also increases the risk of health workers contracting the disease whose case-fatality rate ranges from 25 to 90 percent. This is several times higher than that of Covid-19, which hovers between three and five percent.
President Museveni said on Wednesday night during a national address that mobile laboratories are also being deployed to Mubende District to enable timely diagnosis and improve care.
Currently, testing is being done at Uganda Virus Research Institute, with a turnaround time of around one day—the length of time health workers said affects decision making and care.
Dr Ian Clarke, the chairman of Uganda Healthcare Federation, the body that brings together private players in the sector, said there is also a need to train health workers on vigilance and identification of such diseases like Ebola.
“I read about one of the kids who was treated. He went and was not having malaria and then he went back and was treated for malaria and eventually they realised it was Ebola,” he said, adding, “We need to bolster training of our health workers to ensure that anywhere they work, they can detect the disease.”
Some health officials recently accused private hospitals of delaying the detection of the outbreak, an allegation Dr Clarke said is misdirected.
Dr Issa Makumbi, the deputy director of Uganda National Institute of Public Health (UNIPH) and director of the Public Health Emergency Operations Centre (PHEOC), questioned the capacity of health workers in private hospitals.
“Most of the cases were moving from one private hospital to another and the facilities were not very vigilant. They couldn’t detect it early, but also one of the problems is that the signs of Ebola are not very specific. You could think someone has malaria or diarrhoea,” Dr Makumbi argued.
Training concerns
However, Dr Clarke said: “The nurses and the doctors who practice in Mulago Hospital or IHK [International Hospital Kampala] are trained in the same universities. Our question should be: how well are our doctors trained? How quickly can they pick out a case of Ebola.”
Prof Khama said the government should also be clear about what they do with the cases and suspected cases.
“They should not be allowed to roam around. There should be a way of quarantining them. Government must be aware of the socioeconomic challenges that come with restrictions. We have seen that these challenges affect people’s livelihood and when this happens, people break the law,” he added.
The Ebola taskforce in Mubende, the epicentre, reported on September 23 that around seven suspected Ebola patients and contacts of victims disappeared from the Mubende isolation facility.
Dr Henry Mwebesa, the director general of Health Services, said on Thursday that one of the escapees who tested positive is still missing.
Sources at the facility told Saturday Monitor that there were gaps in security at the facility which the suspects took advantage of.
Suspect still at large
Dr Mwebesa, however, said they are improving contact tracing, care for the patients and information sharing to curb the spread and deaths.
“The suspected case in Kasangati [Wakiso District] was negative, even the one in Masaka. There is one escapee who had tested positive. That is worrying us. We will be updating people every day,” he said.
Dr Mwebesa said they are handling the six health workers who contracted the infection.
“They operated on a patient who was vomiting and bleeding. This was before we confirmed Ebola. One of them is in a critical condition, but the team is trying their best,” he confirmed.
Dr Herbert Luswata, the secretary general of the medical association, appealed to the Health ministry to evacuate intern doctors from Mubende hospital to safeguard them from infection, a proposal which was rejected by Dr Mwebesa.
“There is one intern doctor, and then three senior house officers (doctors who are doing their masters) and one third-year medical student who tested positive,” Dr Luswata said.
However, Dr Mwebesa said they will not move the interns from the facility.
“Those interns are in hospital to learn. Ebola is one of the medical conditions that they will treat when they graduate as doctors,” Dr Mwebesa said.
‘we are doing well’
Dr Mwebesa said the death rate from the current outbreak is far low when compared to what was seen in the past outbreaks.
“The case fatality rate is 19.4 percent. This means we are doing well. If infected people can come early, the death can be reduced,” he said.
His figures, however, don’t include people who died and were buried before the outbreak was confirmed. Those people were not tested.
Mr Museveni said on Wednesday that in the previous outbreaks, out of 100 people who got Ebola, 53 died. “The body can fight it. If you get it, you should go to the hospital quickly,” he said.
In the 2000 Ebola outbreak, 425 people contracted the disease and 224 died—partly because of the lack of experience and preparedness to handle the cases.
The Ebola outbreak in Mubende District was triggered by the Sudan Ebola virus, a strain which has no approved vaccine. Dr Mwebesa said discussions are going on to decide whether they can use a vaccine for Zaire Ebola virus, which the World Health Organisation is not supporting because of lack of evidence.
Prof Khama has meanwhile warned the country against using force.
“Government must mobilise people to protect themselves and protect each other. This is not police work but public health. It is about getting out to people and convincing them that you and I can make a difference if we do the right things,” he said.




