Prime
How Gulu medics safely delivered ectopic baby

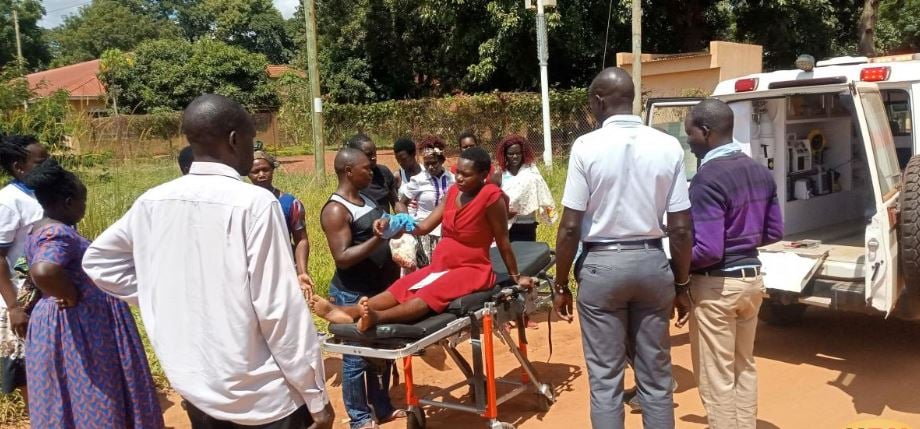
Medics attend to Ms Scovia Aciro at Gulu Regional Referral Hospital’s maternity ward. PHOTO/SIMON WOKORACH
What you need to know:
The medical team performed a caesarean section to safely deliver the baby and address the unique positioning of the foetus.
On July 28, Ms Scovia Aciro, 25, arrived at Gulu Regional Referral Hospital from Awach Health Centre IV in Awach Sub-county, Gulu District aboard a boda boda.
Ms Aciro, a resident of Ayweri Village, Paibona Sub-county, had been transferred to the hospital due to a critical condition that could not be addressed by medical professionals at both Paibona Health Centre III and Awach Health Centre.
She had been informed that her unborn baby was positioned incorrectly, and her condition could deteriorate rapidly if not promptly treated. Upon arrival at the maternity ward, Ms Rose Akumu, a midwife, welcomed her.
“When I reached the hospital, I was examined and taken through another scan but it still confirmed that the baby was outside the uterus, and they recommended me to undergo a caesarean section,” she said.
To Ms Akumu, this is the first case the hospital has handled since she qualified as a midwife in 2004.
“We received and examined her and carried out several observations and we tried to check whether she was in labour, but no result. I have never witnessed it,” Ms Akumu said.
Further examinations revealed that Ms Aciro’s pelvis was closed, and it was observed that the baby’s ribs were protruding from her abdomen.
“We became concerned when we were shown her scan results; we informed the doctor who sent her again for a fresh scan but the result was the same. On receiving the result, the doctor immediately asked the midwives to prepare the mother and take her for delivery,” Ms Akumu said.
On July 29, at about 6pm, a team of 15 medical personnel assembled for a pre-surgery briefing.
The team included an aesthetician, medical doctors and midwives, led by Dr Francis Pebalo Pebolo, a consultant obstetrician and gynaecologist, at Gulu Regional Referral Hospital.
“We received the 25-year-old mother, who was in her third pregnancy and had been referred from Awach Health Centre IV. She had some complaints of severe abdominal pain that has been disturbing her since she became pregnant,” Dr Pebalo said.
He said the pregnancy was already 38 weeks, which meant the baby was due for delivery.
“We started digging back and we realised that she did a scan at 25 weeks of pregnancy; that is about six months and 1 week. That scan showed that the baby was inside the uterus only that the lower part of the uterus is where the placenta had covered,” Dr Pebalo noted.
The team prepared and informed the surgeon to be on standby while the laboratory booked blood in case the need arose, but we realised the placenta was positioned in front of the baby and if an attempt was made to deliver the baby through the placenta, there would be terrible bleeding, he said.
“During the two-hour intense procedure, we were able to expand the incision and delivered the whole sack. The good thing was that the baby formed a sack within the omentum, this is something that hangs on the intestines like a curtain that prevents any other infectious particles from there,” Dr Pebalo said.
The operation was successful, resulting in the safe delivery of a 2.6 kg baby. Both the mother and child were reported to be in good health.
Dr Pebalo said this was a rare condition, adding, “The first pregnancy we found growing in the abdomen was in 2018 and that one, we found the baby was already dead; it tore the sack.”
Dr Pebalo expressed gratitude to the team, which he praised for having expertise.
Mother speaks
When Ms Akumu returned to the facility for a checkup on Monday, she told Daily Monitor that she experienced abnormal pressures and sickness in the first trimester.
“I tested and they said it was malaria and I took some anti-malarial drugs but the condition persisted. I was always in pain and once the sickness attacked me, I then felt terrible pain in my lower abdomen such that I am unable to stand up nor walk easily,” she said.
The doctors at Awach Health Centre IV recommended a scan and the results indicated that the foetus was positioned in the omentum, a large flat tissue layer that connects the stomach and duodenum with other abdominal organs.
At one of the private facilities, according to Ms Aciro, a medical doctor advised her to go to Gulu Referral Hospital to have the foetus removed to avoid further complications.
“I went back home and informed my family members about my condition but none of them believed me, saying it is not possible that my baby can begin to grow outside the uterus,” she said.
Ms Aciro applauded the medics for saving her life and her baby.
Ectopic pregnancy
An ectopic pregnancy occurs when a fertilised egg implants and grows outside the main cavity of the uterus.
According to World Health Organisation, this is one of the most dangerous complications of pregnancy.
In this case, the baby was growing outside the uterus, specifically within the omentum—a large flat tissue layer in the abdomen that connects the stomach and duodenum with other abdominal organs. This condition is extremely unusual and potentially life-threatening, as it can lead to severe complications for both the mother and the baby.