Prime
ICU bed capacity in Uganda
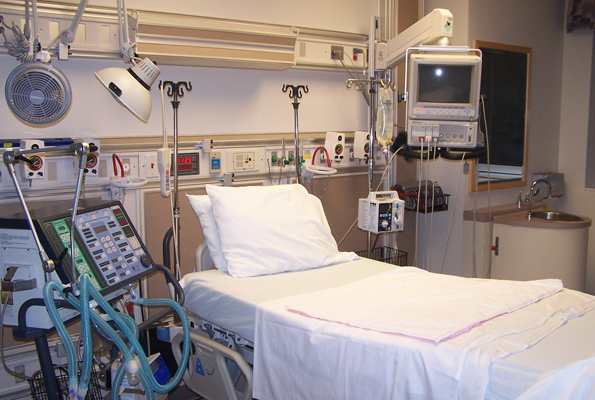
A bed in an Intensive Care Unit. The equipment in ICUs are generally costly but because they save lives - at least every hospital should have one.
A research titled “Assessment of the current capacity of Intensive Care Units (ICU) in Uganda; a descriptive study,” by Patience Atumanya, Cornelius Sendagire, Agnes Wabule, John Mukisa, Lameck Ssemogerere, Arthur Kwizera, Peter K Agaba shows that the country has 55 functional intensive care beds in the 12 ICUs that are operational.
The research was conducted in 2019 and results released in January.
The report indicates that of 14 ICUs in the country, 12 are operational and two are non-functional due to wlack of human resource. Only a quarter of the 12 are in public hospitals.
An additional 20 beds had no ventilatory capacity. Majority of ICUs are anaesthesiologist-led, run a closed model, and have variable nurse-patient ratios.
READ:
ICU staffing levels
Anesthesiologist-led ICUs constitute the majority (75 per cent). Those that are internist-led are supported by anesthesiologist residents (anaesthesia and internal medicine) and medical officers. Ancillary staff are present in most of the ICUs. The average nurse-patient ratio is 1:2 and in one public ICU at 1:8. A total of 171 nurses, of whom 13 (7.6 per cent) have some formal training.
ICU structure and equipment
The 55 ICU beds make up a ratio of 1.3 ICU beds per million population. About 20 extra non-ventilated beds are found in the ICUs used for High Dependency Unit (HDU) care. Of the 12 ICUs, 10 have pipeline oxygen, with 70 per cent of them having one port per bed
Other organ support and physiological monitoring facilities
Renal replacement therapy is available in most ICUs (58.3 per cent), with Intermittent Hemodialysis being the only modality. It was discovered that blood gas monitoring in most of the public units is not always available due to the inconsistent supply of consumables despite the presence of the machine in the ICUs
The study concluded that although the Intensive Care Unit service in Uganda has improved, there is limited access to them. There is need to train ICU personnel to increase accessibility.