Prime
Ugandan doctor behind revolutionary Ebola diagnostic kit
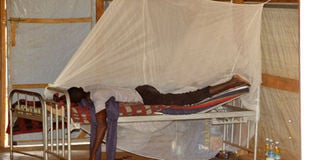
Infected. An Ebola patient lies in an isolation centre in western Uganda in 2012. FILE PHOTO
What you need to know:
Revolutionary. After failing to get funding from the government in 2013, Dr Misaki Wayengera, a researcher attached to the Department of Pathology at Makerere University’s College of Health Sciences, won a $100,000 grant from Grand Challenges Canada to create the Pan-Filovirus Rapid Diagnostic Test, a paper-strip test used in detecting Ebola and Marburg viruses. Dr Wayengera spoke to Sunday Monitor’s Joan Salmon about the journey and the fight against Ebola.
In a way, we consider ourselves as revolutionaries because we bring change, good one at that, to our societies through the knowledge we have gathered over the years. Nonetheless, achieving the full potential of that impact – including inspiring the younger generations and garnering the necessary resources and partnerships needed for moving our ideas from the laboratory to something that can be practicalised to help the public, is something only possible if we partner with the media,” says Dr Misaki Wayengera, a researcher and inventor of the Pan-Filovirus Rapid Diagnostic Test (Pan-filo-V RDT).
In 2014, when the Ebola epidemic broke out in West Africa, Dr Wayengera and his team were very pivotal in its control and he believes “as Africans, we can do more to solve our issues”.
This senior lecturer from the Departments of Pathology, Immunology and Molecular Biology at the College of Health sciences, Makerere University, is also a clinician in charge of the Unit of Genetics and Genomics where he caters for children with genetic disorders.
“As a medical doctor, I believe I should apply my knowledge for the betterment of my community. There is a sense in which we should appreciate that as doctors, we are merely custodians of medical knowledge for society,” he adds.
“To that effect, currently my team and I are developing the next generation of tuberculosis diagnostic tests, a potential HIV/Aids cure and the Ebola diagnostic kit.”
Gulu outbreak
In 2000, Dr Wayengera was in his second year as a medical student when Ebola broke out in Gulu and Masindi districts.
Over time, he has learnt that Ebola can be easily controlled through a quarantine. However, most outbreaks start in remote areas that lack laboratories and hospitals.
In its early stages, he says, Ebola presents symptoms such as high temperature, body weakness, muscle and joint pains, and vomiting that are similar to other illnesses. And yet, specific diagnosis requires techniques of high sophistication which were not available within the village settings, putting both health workers and other community members at risk.

Dr Misaki Wayengera, a researcher and inventor of the Pan-Filovirus Rapid Diagnostic Test. PHOTO BY JOAN SALMON
Ebola is a very high-risk pathogen (denoted class A) and at that time, samples were taken to laboratories in South Africa or the Centres for Disease Control (CDC) in the US and it took a minimum of two weeks before test results were returned, delays that lent opportunity to the spread of the epidemic.
“It was the first indicator of how an Ebola outbreak could socio-economically paralyse and render vulnerable an entire population. Dr Matthew Lukwiya along with many others died of something preventable,” says Dr Wayengera.
The need for speedy diagnostic got him thinking of what could help do the tests in a simple, affordable and yet rapid way.
“There were other such test kits like that of HIV and pregnancy. I knew we could do the same for Ebola. Nonetheless, we needed funding and the necessary skills. We also required partnerships with a biosafety level 4 facility.”
Although Dr Wayengera says a biosafety level 3 laboratory has since been built at the Uganda Virus Research Institute (UVRI) to help with such diagnosis tests, he emphasises that the appropriate laboratory needed for the study of such high-risk pathogens is a biosafety laboratory level 4 of which there are only two in Africa, and only one dedicated for such cases which is in South Africa.
Following completion of his medical studies in 2004, Dr Wayengera got the opportunity to go for a bio-entrepreneurship training at the Medical and Related Sciences (MaRs) Discovery District at the University of Toronto.
“It was this training that exposed me to the expertise of studying the entire set of the pathogen DNA (genomes) and in 2007 I was able to identify the unique targets we are developing into an Ebola detector,” he says.
In 2008, in light of the frequent outbreaks of Ebola and Marburg in Uganda, and his awareness that these kinds of pathogens could be weaponised and used for bioterror, he reached out to President Museveni and relayed the need to prepare for any future outbreaks, including the need for funding to get the detectors ready.
Meeting President
Whereas the President promptly and enthusiastically responded, pledging to support this frontier, no funds came through.
“We believe that if we had got funding as had been promised then, we would have been more than ready for the West Africa Ebola outbreak in 2013,” Dr Wayengera says.
“It’s the one example of how missed opportunities at developing the necessary technologies and or solutions, can cost an entire people. We lost more than 11,000 people in West Africa and those countries were socio-economically debilitated to immeasurable levels.”
In search for an alternate avenue to keep the ball rolling, Dr Wayengera learnt of the Rising Stars in Global Health, a Grand Challenges Canada programme by Sandra Rotman Centre for Global Health where one would apply with an idea with the hope of getting a $100,000 (Shs370m) grant to test it.
He applied for it in 2012 and got the seed funding in 2013. To aid his work, Dr Wayengera approached Dr Julius J Lutwama, who had spear-headed the laboratory interventions for the 2000 Ebola outbreak, and Dr Robert Downing, the then CDC/WHO country liaison officer at the UVRI, asking to be availed with the 2001 Ebola samples.
“I want to thank Dr Edward Katongole-Mbidde, the then UVRI director, who trusted us on recommendation of the former team, to use the gamma-irradiated samples. These samples aided in the ‘proof of concept stage’ which was critical for securing further funding and was due to be finalised by December 2014,” he says.
But as luck would have it, in October 2014 the programme officers at Grand Challenges Canada called to see if Dr Wayengera and his team had data regarding their findings.
“We had data and a team of two R&D [research and development] experts from Halters Associates LLC, California were sent to evaluate it. After a presentation, they liked what they saw.”
This inquisition into their findings was because West Africa had been hit by the Ebola virus that as of June 2014 declared a public health emergence of international concern by WHO.
“As a result of this rapid review process, in November 2014 we were scaled up to receive an extra $1m (Shs3.7b) as a transition to scale grant, to enable us fast-track the development and deployment of our kit in the Ebola-hit countries,” Dr Wayengera says.
The transition grants are, however, only given on condition that the recipients have another matching funder. As luck would have it, he was able to have a face-to-face meeting with the President again when he needed expert advice of a geneticist on the anti-homosexuality Bill.
“Two letters were written to the College of Health Sciences, and the Ministry of Health, seeking the advice of a genetics expert, and they both ended up on my desk – being the only practicing clinical geneticist in the country. Disappointingly, that funding also never came through,” Dr Wayengera says.
“Maybe it is because, as scientists, we were busy with experiments to keep on the run for monies promised by the President. This was perhaps the one time I was tempted to give up on my country. But given the commitment of the head of State to scientists, I kept my patriotism.”
During that time, Dr Wayengera started working on producing diagnostic kit prototypes and went to Dr Vinand Nantulya of Astel Diagnostics (U) LTD, another Ugandan biotech producing tests for malaria, HIV and other infections.
“Prof Nantulya has more than 50 years of expertise in diagnostic research and development and his team is a key partner in our pursuit to make these detectors a reality.”
They also went to South Africa to start performing tests on live samples in the bio-safety level 4 laboratory with the help of Prof Dr Janusz Tadeusz Paweska at the Centres for Emerging Zoonotic and Parasitic Infections of the National Institute for Communicable Disease, Johannesburg.
“We realised that while the tests were working well with artificial or recombinant Ebola proteins, they were not working with the live samples. It is clear to us now that this happened because targets were masked with extra protein, glycans and folding which needed to be removed before testing,” says Dr Wayengera. However, with funds running out they were stuck.

A health worker screens flight crew at Entebbe International Airport in 2014.
“As a scientist, this is the one point when one gets frustrated to the core; failing to deliver a solution. Unlike academic research, R&D is a resource-intensive endeavour riddled with many failures, re-strategising and repletion of experiments. This is the stage when one needs an open cheque,” he says.
Additional funds
It was not until June 2018 that they got additional funds from the European Union through the European Developing Countries Clinical Trials Partnership (EDCTP).
“Throughout this, we continue working with our key established partners, namely Astel Diagnostics (U) LTD and the BSL_IV Laboratory at the NICD, SA. I want to specifically thank the Office of the Sierra Leonean Ethics and Scientific Research Review Committee, Ministry of Health, for allowing us to use the samples of the patients of the EVD outbreak,” he says.
Shortly after this award, the EDCTP announced another round of emergency response grants to respond to the on-going outbreak of Ebola in North Kivu, DR Congo, to which Dr Wayengera applied and in September 2018, got communication that they had been awarded the grant.
“This is supposed to help in developing a buffer to remove the protein off the virus in the blood to aid rapid diagnostic testing,” he says.
The project involves researchers from four European countries – Poland, Sweden, Greece, and Netherlands – alongside South Africa, with the team in Uganda heading and coordinating its implementation.
The ball continues to roll for this scientist because in November 2018, when WHO called out for Africans with solutions through WHO Innovation Challenge, the team applied and they were shortlisted.
“They were looking for solutions that were almost ready to go to the market and out of the over 2,400 people who applied, only 30 made it to the finals and I am one of them,” he says.
Where detector can be used
• Outbreak scenario: Initial screening for cases and triage at the point of care. The Pan-Filo-V RTD® presents the ideal solution for remote equatorial village settings because it is affordable, requires minimal expertise, does not need electricity or a laboratory.
• Clinical suspicion and exposure-prevention: Given that many tropical infectious disease present similarly to the early symptom of viral haemorrhagic fevers, any patient presenting with fever and unexplained bleeding should be screened. This can help prevent primary exposure by health-workers and other contacts.
• Community, border and or port control: The Pan filo-V RDT® is designed to increase border and port screening for persons potentially exposed to filovirus disease, as would be necessary for travellers coming from an active epidemic-zone.
• Bioterror attack: Although the prospects for a bio-terror attack involving filoviruses is minimised by need for a living career or vector, the same is possible. Filoviruses are classified as Class A pathogens, with potential for bioterroristic weaponisation.
• Vaccine B cell response studies: Given that many trail vaccines are based on a live-attenuated vector carrying the GP protein, qualitative studies of antibody responses are possible using the Pan-filo-V RDT®.
• Population exposure studies: Many persons within equatorial Africa (including long-staying visitors) may have unknowingly been exposed to floviruses in the past.
In order to recruit these subjects, one needs to confirm their previous exposure by presence of IgG antibody.



