Prime
Can malaria vaccine pass hesitancy test?
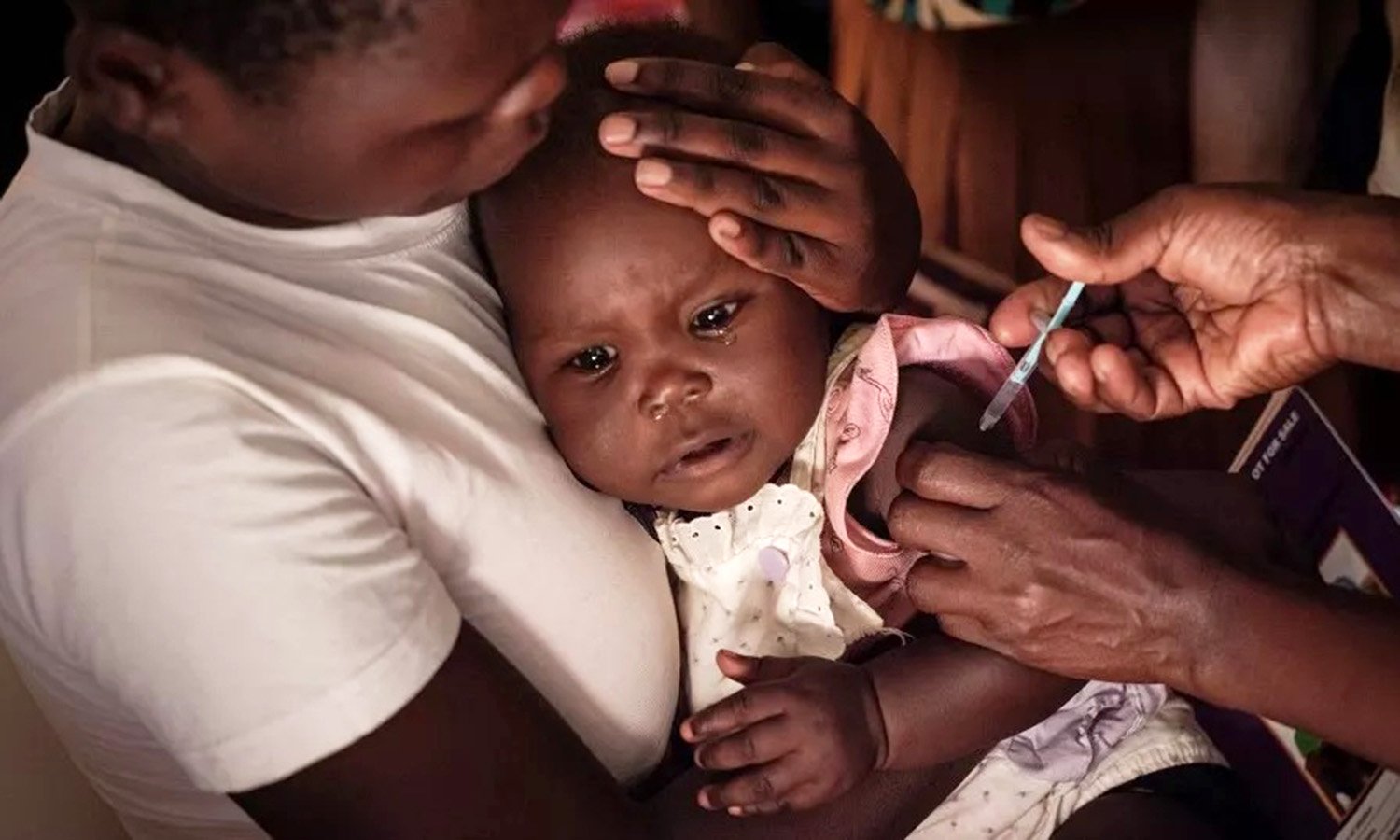
A child receives a shot during the launch of the extension of the world’s first malaria vaccine in Kimogoi Dispensary in Gisambai, Kenya on March 7. Some Ugandans are hesitant to take the vaccine. Photo/AFP
What you need to know:
- Target Malaria, a research hub focusing on the disease, estimates that Uganda loses $500 million (Shs1.9 trillion) annually on treatment and missed work.
- The treatment expenses, per the National Malaria Control Programme, include “out-of-pocket expenditure for consultation fees, drugs, transport and subsistence at a distant health facility.”
Mr Eric Yiga, a freelance journalist in Mukono District, is the breadwinner for his seven-strong family. A huge chunk of that “bread” is going to healthcare for his wife, Justine, as she recovers from a malaria episode.
“We just spent a week in the hospital where she was given different malaria treatments,” Mr Yiga said, adding, “By the time we left, our hospital bill was more than Shs150,000 on treatment alone.”
This is the fifth time a member of Yiga’s family has been struck down with malaria this year. If it is any consolation, they are not outliers. Last September, Ms Alice Nabukenya, a banking officer, spent five days being treated for malaria in a top private hospital in Kampala.
She was later discharged with a hospital bill of Shs2.5m, with health insurance paid by her employers picking up the tab.
The government says at least Shs30,000 is spent per malaria episode in public health facilities and that many people suffer from more episodes annually in a country where millions still live on less than $1 (about Shs3,700) a day.
Target Malaria, a research hub focusing on the disease, estimates that Uganda loses $500 million (Shs1.9 trillion) annually on treatment and missed work. The treatment expenses, per the National Malaria Control Programme, include “out-of-pocket expenditure for consultation fees, drugs, transport and subsistence at a distant health facility.”
Leading killer disease
Malaria, a mosquito-borne infectious disease, claims the lives of hundreds of thousands of people globally each year, particularly in sub-Saharan Africa. The World Health Organisation (WHO) says Africa accounted for approximately 95 percent of global malaria cases and 96 percent of malaria-related deaths in 2021.
Uganda’s Annual Health Sector Performance Report for 2022/2023 revealed major causes of deaths, with malaria on top, accounting for 4,245 deaths, which is 7.7 percent of total deaths.
Dr Jane Ruth Aceng, the Health minister, while addressing Parliament in July 2022, said there would be no malaria in Uganda by 2030. At that, WHO indicates that Uganda still has the world’s highest malaria incidence rate of 478 cases per 1,000 population per year.
Data from the Health ministry shows that the two yearly rainy seasons, which usually occur from March to May and from September to November, coincide with the transmission peaks.
For example, Rev Sr Alice Atayi, a nurse at Adjumani District hospital, told Saturday Monitor that “right now with the heavy rains, we are witnessing an increase in cases of malaria.” Children below five years and pregnant women are always hit the hardest.
New-found hope
The Uganda government in October announced a significant breakthrough in the fight against malaria with the emergence of another promising vaccine. The R21/Matrix-M, targeting children below five years because of their vulnerability to infection due to lower immunity, became the world’s second malaria vaccine. This followed an earlier approval of the RTS,S/AS01 by the WHO.
The RTS,S/AS01 is a four-dose vaccine administered through an injection with the first three doses delivered monthly from the fifth month and the last shot at nine months of age.
On the other hand, R21/Matrix-M is a three-dose vaccine delivered in the same period, with a booster shot one year after the completion of initial three doses.
“In areas with highly seasonal malaria transmission [where malaria transmission is largely limited to four or five months per year], the R21 vaccine was shown to reduce symptomatic cases of malaria by 75 percent during the 12 months following a three-dose series,” the WHO said in a statement.
With the second malaria vaccine in place, there is renewed hope in the battle against one of the world’s deadliest diseases for two reasons: one, demonstrated higher level of efficacy; and, two, lower cost of each malaria episode treatment compared to other interventions. But the global health body also says the choice of which vaccine to use in a particular country depends “on programmatic characteristics, vaccine supply, and vaccine affordability.”
Vaccine costs
WHO has indicated that the R21/Matrix-M vaccine costs between $2 (Shs7,500) and $4 (Shs15,000) per dose, bringing the total to Shs60,000 per individual for the prescribed three-dose plus the booster complete vaccination. The first malaria vaccine, RTS,S, costs about $10 (Shs37,000) per dose, meaning at four doses, the government would spend more than double the amount (about Shs148,000) for full vaccination on each child, which makes R21/Matrix-M a cheaper choice.
Dr Jimmy Opigo, the manager of Uganda’s malaria control programme in the Health ministry, failed to respond to our repeated calls and WhatsApp messages.
Nonetheless, in an interview with this publication in October, he said while the country had been allocated 800,000 doses of the RTS,S/AS01 free of charge, fully covering only 230,000 of Uganda’s children, under the Global Alliance for Vaccines and Immunisation, no commitment had been made in respect to R21/Matrix-M vaccine.
But Dr Diana Atwine, the Health ministry’s permanent secretary, said the government intends to roll out the vaccination early next year.
Vaccine hesitancy
Nevertheless, like it was during the vaccination drive against Covid-19, the malaria vaccine is not immune to hesitancy. Mr Yiga, for example, prefers treating each malaria episode as opposed to vaccination.
“We have seen many vaccines introduced, but people end up being affected negatively,” Mr Yiga said, adding, “Just look at reports on the side effects of Covid-19 vaccines such as blood clots resulting from AstraZeneca that most Ugandans received, tell me why I should trust this one. The least the government and manufacturers do is to apologise and life goes on.”
Ms Nabukenya’s views on the malaria vaccine are not any different. She does not trust the vaccine and is not willing “to risk my three-year-old daughter for it.”
Mr Samuel Masaba, a nutritionist in Mbale City, said: “These vaccines are always developed in Europe and America, only to be tested in Africa. Why?”
While Mr Masaba stated that every vaccine is tested in Africa, available data from WHO indicates that Covid-19 vaccine clinical trials were conducted in China, USA, and Europe, with only two percent done in Africa as of May 2021. Clinical trials for malaria vaccines, however, were largely conducted in Africa because it is where most malaria infections are found.
Even when Uganda has tried all available interventions to curb malaria and the disease has persisted, Mr Yiga said it is better for the government to “continue sensitising people about malaria prevention and treatment, and stocking the necessary drugs in health facilities as opposed to untrusted vaccines.”
Experts’ reassurance
Dr Catherine Maiteki, the deputy manager for the malaria control programme of the Health ministry, said people do not need to fear vaccines.
“The vaccine is safe and effective in preventing severe disease. The vaccine doesn’t prevent malaria [infection], but when a child who has been vaccinated encounters malaria, their body is primed for the fight,” Dr Maiteki told this publication during the announcement of the second malaria vaccine in October.
Ms Kate O’Brien, the director of immunisation, vaccines and biologicals at WHO, also said: “Both vaccines are shown to be safe and effective in preventing malaria in children and, when implemented broadly, are expected to have a high public health impact.”
While speaking to AFP last week, Unicef chief Catherine Russell, said thus: “Introducing vaccines is like adding a star player to the pitch ... we are entering a new era in immunisation and malaria control.”
Vaccine rollout
In terms of readying the public ahead of the malaria vaccine rollout early next year, Dr Richard Kabanda, the commissioner of health promotion, education and communication in the Ministry of Health, said all preparations are underway.
“We are still in internal preparations for all required materials and content development,” he told Monitor.

Sleeping under an insecticide-treated mosquito net is the best way to prevent mosquito bites. Photo/File
To support these efforts, Uganda is—per the Global Fund—currently running two malaria grants of up to a tune of $263 million (Shs995 billion) towards the Malaria Reduction and Elimination Strategy, which targets to reduce the disease infections “by 50 percent, morbidity by 50 percent and malaria-related mortality by 75 percent by 2025.”
As the country awaits the malaria vaccine rollout, part of the Global Fund money is being used in distribution of insecticide treated mosquito nets, indoor residual spraying and campaigns against malaria, according to information from the Health ministry.
Mr Linden Morrison, the Global Fund’s head of High Impact Africa, said their commitment in the fight against malaria is “unwavering” and that they are “dedicated to making a lasting impact.”
Malaria burden
Almost half the world’s population lives in a malaria high-risk area, with the vast majority of cases and deaths occurring in Africa. Africa accounted for approximately 95 percent of global malaria cases and 96 percent of related deaths from the mosquito-borne disease in 2021.
Yearly, global malaria deaths fell dramatically between 2000 and 2019—when they stood at 568,000—but shot up 10 percent in 2020 to 625,000 as the Covid-19 crisis hit protection and treatment efforts. Deaths dipped slightly to 619,000 in 2021 -- of which 77 percent were children aged under five. Meanwhile, global malaria cases rose slightly to 247 million.
According to a November 2023 joint statement by the WHO, Unicef and the Global Alliance for Vaccines and Immunisation (Gavi), more than two million children have been jabbed in Ghana, Kenya and Malawi in a pilot phase since 2019, resulting in substantial reductions in severe malaria illness and hospitalisations.
More 1.7 million doses are expected in Burkina Faso, Liberia, Niger and Sierra Leone early next year.
Source: AFP




