Prime
How VHTs have eased access to health services in lockdown
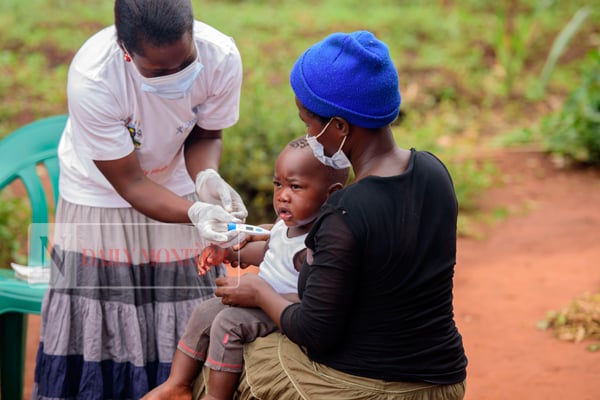
Hasifa (right) has her baby’s temperatured measured by a VHT. PHOTOS /LYDIA AINOMUGISHA
What you need to know:
- Community health workers locally known as Village Health Teams (VHTs), play a critical role in extending essential health services, especially in hard-to-reach areas. During this Covid-19 pandemic, Lydia Ainomugisha writes that VHTs’ roles couldn’t have been brought to the fore any better.
Before the Covid-19 pandemic, life was as normal as it could be for 20-year-old Bridget Nasasira, a resident of Kalerwe, a Kampala suburb.
She was pregnant and would access antenatal care from a nearby government health facility and was actually due for her final visit.
Her life suddenly changed in March 2020 after the government announced a lockdown to contain further spread of Covid-19 that was ravaging the globe. Her husband lost his job and left her. Bridget had to relocate back to her mother’s house in the same neighbourhood because she could not afford to pay rent.
Luckily for her, Sarah Nakyambadde, 49, a member of the Village Health Team (VHT), was always at hand encouraging her to go for antenatal care.
Nakyambadde ensured Nasasira went to the health facility for a safe delivery and has since been attending to her son, who is now one year old.
“I don’t know how my child and I would have survived this season without Nakyambadde services. She cares a lot and even calls to check on how my son is doing,” Nasasira says.
Nakyambadde has been a VHT for the last 12 years. She owns a stationery shop. When she is not making counter books for sale, you will find her in the community educating and sensitising households about their health, and offering reproductive, maternal and child health services.

Sarah Nakyambadde, a VHT in Kalerwe, Kampala.
“Before the pandemic, my clients used to come to my house for treatment. But when the pandemic broke out, they were afraid to leave their homes so I had to instead go to them—moving door-to-door—because the children were sick and their parents would call me to attend to them. I was able to help them because I had personal protective equipment (PPEs) to keep me and my clients safe,” Nakyambadde explains.
Hasifa’s story
Another woman with similar experience is Hasifa. She lives in a village near the shores of Lake Victoria in Buikwe District, one of the border districts that were severely affected by Covid-19. The nearest health centre is quite far from her home. There are clinics within a walkable distance, but their services are expensive. When her children fall sick, Hasifa calls Shamidan Kakisuyi, a VHT who lives a few houses away.
“Kakisuyi used to check on me almost daily when I was pregnant and ensured I accessed the necessary antenatal care. Towards my delivery date, I got some complications and she rushed me to the hospital. Without her, the situation would have been dire. I also rely on her to treat my children. There would be a big gap without these VHTs in our community,” Hasifa says.
“Hasifa came knocking on my door at about 2am, holding her four-year-old child, who had a high temperature and was convulsing. She was crying inconsolably. I quickly gave the child some paracetamol to cool the temperate as I tested for malaria with a rapid diagnostic test. I gave the mother a referral but she was too scared to go in the night, so I gave the child treatment (she had malaria ++) and took care of her throughout the night. By morning, the baby was feeling better and was out of danger,” Kakisuyi narrates. She is linked to the government health facility in her sub-county, and is supported to conduct outreach activities for routine immunisation.
Linking people to health services
For some families, VHTs are the easiest and preferred option of accessing basic health services for children in the face of Covid-19 that has got many health facilities stretched.
For instance, Eve Nalwoga from Mityana says she has been relying on Maria Kabeega, a VHT, for more than two years.
“I use her services because they are reliable and she always has quality medicines. Why would I, a physically disabled person, inconvenience myself by going to health facilities when there are readily available services for my children in my community?” she wonders
Demand for community-based services
A recent review of government data in Uganda, conducted by Living Goods, a non-profit non-governmental organisation (NGO) that focuses on strengthening and digitally enabling community health programmes, revealed that there was 35 per cent decline in the number of people who sought facility-based care and treatment for common childhood diseases, due to the Covid-19 pandemic. Living Goods has been giving VHTs in more than 20 districts free essential medicines for children under five years to ensure they would not go untreated.
Similarly, a December 2020 survey by Twaweza, an NGO, found that nearly half of women (49 per cent) point to inadequate health facilities and disease as some of the biggest problems facing the country.
Even worse, 79 per cent of Ugandans, according to the survey, say teen pregnancy has become a bigger problem during the coronavirus pandemic.
Mothers turn to VHTs first not only because of their close proximity but because they offer personalised care that enables unparalleled trust when it matters most: changing public health behaviours amid an evolving crisis.
“Community health provides a gold standard of personal, affordable and accessible health care close to home, while enabling facilities to focus on those who need them most,” Christine Namayanja, Living Goods Uganda’s country director, says.
She adds that when digitally enabled, equipped with medicines, appropriately supervised and incentivised, VHTs have proven more than capable of filling vital gaps in essential health service delivery.
Uganda’s doctor to patient ratio is estimated at 1:25,000—way above the World Health Oraganisation (WHO) recommendation of 1:1,000. In these current circumstances, VHTs are a resource in the rollout of the Covid-19 vaccination campaign to the general population. The trust they have engendered in their communities will be essential for ensuring families understand the potential side effects and that vaccines reach the last mile.
Who are Village Health Teams (VHTs)?
Uganda has more than 180,000 VHTs spread across the country, supported by the government and other development partners. Since VHTs were introduced in Uganda in 2001, they act as the first point of contact and create linkages between households and the formal health system. Their services are even more essential in remote areas where access to health facilities is limited by such barriers as long distances, lack of transport, long waiting time, and unavailability of medicines/supplies.
“Because of the curfew measures put in place to curb the spread of Covid-19, I worked with the local authorities to acquire travel permits for sick and expectant mothers to go to referral hospitals for further treatment,” says Peruth Namanda, a VHT in Namirembe Village, a landing site in Masaka District.
Among other things, VHTs are trained to treat malaria (leading cause of death in Uganda), diarrhoea (second leading cause of deaths of children under age five globally), and pneumonia (the single largest cause of infectious disease death for children worldwide) in children under five. With early detection, these diseases are highly preventable and treatable. Some pneumonia symptoms also mimic Covid-19, so assessing and treating it early helps ensure sick children receive the right treatment and doing so at the community level reduces the burden on health facilities. VHTs also play an essential role in reinforcing messages about hygiene and sanitation, while simultaneously providing households with inexpensive or free life-saving treatments and referrals.
Because of their proximity with the households they serve, VHTs are able to provide services at any time of day or night.



