Prime
INVESTIGATION: How lack of oxygen, poor health sector is killing COVID-19 patients in Uganda

The new Mulago Specialised Women and Neonatal Hospital. PHOTO | RACHEL MABALA
What you need to know:
- Behind the scenes, however, the pandemic was exposing tumours in the country’s health sector. Many of these had grown malignant over time. A 2015 report by Uganda’s Gender, Labour and Social Affairs ministry, together with UN Children’s Fund, had listed the country among the top 10 countries for high maternal, new-born and child mortality.
At 2.46pm on August 7, the Ministry of Health tweeted its daily update on the coronavirus situation in the country. Thirty-one more people had tested positive for coronavirus the previous day, to bring the cumulative total to 1,254. There was also one new death, the statement noted, raising the total number of fatalities to six.
Like the others before it, the death was reported in a sanitised, statistical, matter-of-fact way: the deceased was a 70-year-old Ugandan male, a resident of Nateete, Kampala. On July 24, he had turned up at Lubaga Hospital with mild fever, cough and difficulty in breathing. He was also discovered to be diabetic, “a risk factor for Covid-19”, the ministry statement noted.
When the patient’s condition worsened, he was admitted to the Intensive Care Unit (ICU) and tests confirmed that he had Covid-19 disease. On July 28, he was transferred to the ICU at Mulago hospital.
“Unfortunately, he passed away yesterday evening,” the statement noted ruefully. “May his soul rest in eternal peace.”
The death seemed almost inevitable. At 70, the patient was in a higher-risk demographic, he had been dutifully admitted into not one but two ICUs, and he was diabetic – a co-morbidity that made him particularly vulnerable. The Health ministry statement then moved on to details of the positive samples and where they had been found. Case closed.
Only it wasn’t. An investigation by this newspaper spanning several months shows that the case of Patient Six opened the veil on a health system that appeared to be doing very well on the outside, but which was struggling to cope after a surge in the number of people with coronavirus exposed shoddy construction, defective equipment and an acute shortage of medical workers or personal protective equipment (PPE).
While top health officials basked in the oxygen of good publicity, patients were literally chocking to death.
By the time the call came in, one day in the first week of August, asking the staff at the ICU in Mulago hospital to prepare to admit another coronavirus patient, the medical workers had had enough.
The problems had been there before, but Patient Six had been the tipping point. When he was wheeled into the ICU, the health workers immediately decided to put him on a ventilator, a machine that assists in breathing, to support his lungs that had been decimated by disease.
But there was a problem. Despite hooking the patient up to the ventilator, the alarm warning the ICU staff that their patient was not receiving enough oxygen into his bloodstream refused to stop screaming. They checked the tubes and hoses, but they were all fitted correctly. Still, the alarm continued to wail. It did not make sense.
Founded in 1913, Mulago National Referral Hospital is the largest public hospital in Uganda and was, for a long time, one of the best in sub-Saharan Africa. Then stuff had happened – war, neglect, under-investment, population growth etc., – and the hospital had fallen into disrepair. Patients came, referred from smaller hospitals across the country, but they often found no beds, few doctors and often no medicine.
As soon as it took power in 1986, the new NRA/M government started looking for money to rehabilitate the hospital. The upper section received a facelift over the years, but the main lower facility remained decrepit, a hospital in need of a cure. Eventually, in mid-2011, the African Development Bank approved a $76 million (Shs280b) loan to rehabilitate the hospital.
The money was enough to build a new modern hospital. But the government decided to divert about $34 million (Shs125b) to build two smaller 170-bed referral hospitals at Kawempe and Kiruddu in the city, to decongest Mulago.
Both hospitals were built to completion but, now without enough money and a funding gap of $9.5 million (Shs35b), Mulago started falling behind schedule. The original completion date of December 2017 was pushed back to June 2018, then September 2018, then to end-July 2019, and then to end-December 2019.
Yet by January 2020, as the coronavirus disease began to spread out of China, Mulago remained incomplete. It appears that behind the delays and the funding gaps, corners were being cut.
When the ICU staff checked their equipment, they made a startling discovery. The oxygen being delivered to Patient Six had a concentration of just 25 per cent, only marginally higher than the 21 per cent in the atmosphere that humans ordinarily breathe in unassisted. Patients in ICU typically require this to be higher than 90 per cent concentration.
As part of the rehabilitation, new oxygen plants had been installed in Mulago hospital, but somewhere between the plant, the pipes that carried the oxygen and the tubes that fed it into the patient’s nasal cavity, all they were delivering was the equivalent of hot air.
The medical workers quickly switched Patient Six from the piped oxygen and onto cylinders which, at least they were sure, contained near-pure oxygen. But it was too late. With lungs unable to work on their own, and tubes pumping very little oxygen into his body, Patient Six’s brain was severely starved of oxygen. By the time he was confirmed dead on August 6, and added to the public tally the next day, Patient Six had been brain dead for more than 48 hours, officials familiar with the matter told this newspaper.
The Mulago ICU staff were upset. While the equipment in the ICU looked and smelt new, something was seriously wrong. Like their counterparts elsewhere, the health workers at Mulago were concerned about inadequate supplies of PPEs, having to work very long hours for low pay, and now, the sense that intubating patients in the ICU was more likely to kill them than to save them.

Mulago executive director Byarugaba Baterana (centre) celebrates with staff after they discharged two people who had recovered from Covid-19 at Mulago in April. PHOTO | FILE
Outside Mulago, the cases continued to inch upwards. On August 9, the ministry announced 16 new confirmed cases and one new death – a 49-year-old female resident of Wakiso District, who passed on in a private health facility. The public statement, as was custom, pointed out the extenuating circumstances – the deceased was living with HIV, and had a history of asthma and tuberculosis – that almost suggested the inevitability of the outcome.
On August 10, there were 14 new cases and two new deaths. One was a 27-year-old from Kyangwali Refugee Settlement, who had passed at Hoima Regional Referral Hospital, and a 46-year-old male, at Nsambya hospital. The public statement did not mention any pre-existing co-morbidities.
In the meantime, while the overall number of infections and fatalities remained well short of what, by comparison, Kenya was reporting, the daily report of new infections was now in double-digits. Pressure was building on Mulago ICU to admit more patients, especially those who were older or had co-morbidities. But the health workers at Mulago hospital had seen enough.
While Health ministry officials and loyal cadres were showing off the refurbished hospital on social media, inside things were less than ideal. Key pieces of equipment had either not been installed, had been installed incorrectly, or were not working. The health workers at Mulago were also overworked, under-motivated and potentially exposed to the virus.
The rebellion broke out in mid-August. On August 13, the ICU team at Mulago wrote a memo to the hospital’s deputy executive director listing conditions that had to be met before admitting another patient and, in the process, opened the veil to the problems that had been festering in the hospital.
The unit at Mulago turned over to manage Covid-19 patients has 27 ICU beds, including four isolation rooms meant to provide negative pressure ventilation. This type of ventilation works by sucking in air from outside when the door to the room is opened instead of blowing it out, helping prevent the spread of the virus in the air, in line with World Health Organisation (WHO) guidelines.
The contractor had installed the technology at Mulago but it had not been activated and the four rooms could not be used. Instead, high risk-patients were placed in the open, with two new challenges: the air conditioning units to cool the room could not be run lest they spread the virus through the ICU, where the risk of airborne transmission was already six times higher.
The alternative – opening the windows – would let in dust, which could damage the equipment, or mosquitoes and malaria to already vulnerable patients.
There were more problems. The personal protective equipment supplied to the health workers in the ICU was, in most cases, several sizes too small or simply not enough. But even when it fit the smaller staff members, something was seriously wrong. Although the contents claimed to be KN95 masks, which offer the highest protection, this was at best a misrepresentation and at worst fakes: “This product can’t be used in the isolation ward, observation ward, operating room and other areas of the hospital environment,” the packaging warned.
Frontline health workers deployed in the heart of the medical response to the coronavirus disease had been supplied with sub-standard PPE that directly put them and their lives at risk. This trend has continued across the country, forcing the closure of several hospitals as health workers were infected and forced into quarantine.
With the main plant defective, health workers turned to oxygen cylinders. But oxygen cylinders, the doctors warned in their memo, were unreliable: “In this regard, two patients died in the ICU due to low oxygen concentration in the cylinder, as well as low pressures. More patients will die due to this.”

The oxygen plant at Mulago hospital. PHOTO | COURTESY
That wasn’t all. A nurse had almost been killed when the oxygen cylinder she was moving to a patient’s bedside fell, missing her narrowly. A full cylinder can weigh more than 70kgs. Many were rusty from years of use and a potential source of infection. On a few occasions ICU health workers were unable to swap depleted oxygen cylinders because they did not have the 10-millimeter spanner to open and close the flow valve.
The petition highlighted other serious failures in the facility: crucial ICU medication for critically ill patients was unavailable or in limited supply and drug stockouts were common. Essential tests to monitor the condition of ICU patients were often not done because there were no machines to do them. Where the testing machines were available, consumables were often not available.
One key test, the blood gas analysis, was required at least every four hours for patients on mechanical ventilation in the ICU but none had received it because the test machine did not have the required cartridges.
“Mechanical ventilation without blood gas analysis is akin to driving a car at night with lights off,” the ICU health workers warned.
Other essential laboratory tests, including some stipulated in the Health ministry’s own guidelines for Covid-19 treatment and care, were missing, even at Mulago.
“These tests are not available, and none of the patients has received the results because the laboratory can’t run these tests.”
The petition created a crisis. On the face of it, the country was doing very comparatively better in containing the impact of the virus. The goodwill towards those in charge of the response was palpable: the President’s regular televised national addresses on Covid-19 were eagerly anticipated and widely watched; big business had queued up to donate to the national response to the pandemic, even as the government dragged its feet on providing a stimulus to kick-start the economy. Even the Health minister, Jane Ruth Achieng, had achieved so much celebrity status from her handling of the crisis, she had decided to run for a parliamentary seat on the back of it.
Hidden tumours
Behind the scenes, however, the pandemic was exposing tumours in the country’s health sector. Many of these had grown malignant over time. A 2015 report by Uganda’s Gender, Labour and Social Affairs ministry, together with UN Children’s Fund, had listed the country among the top 10 countries for high maternal, new-born and child mortality.
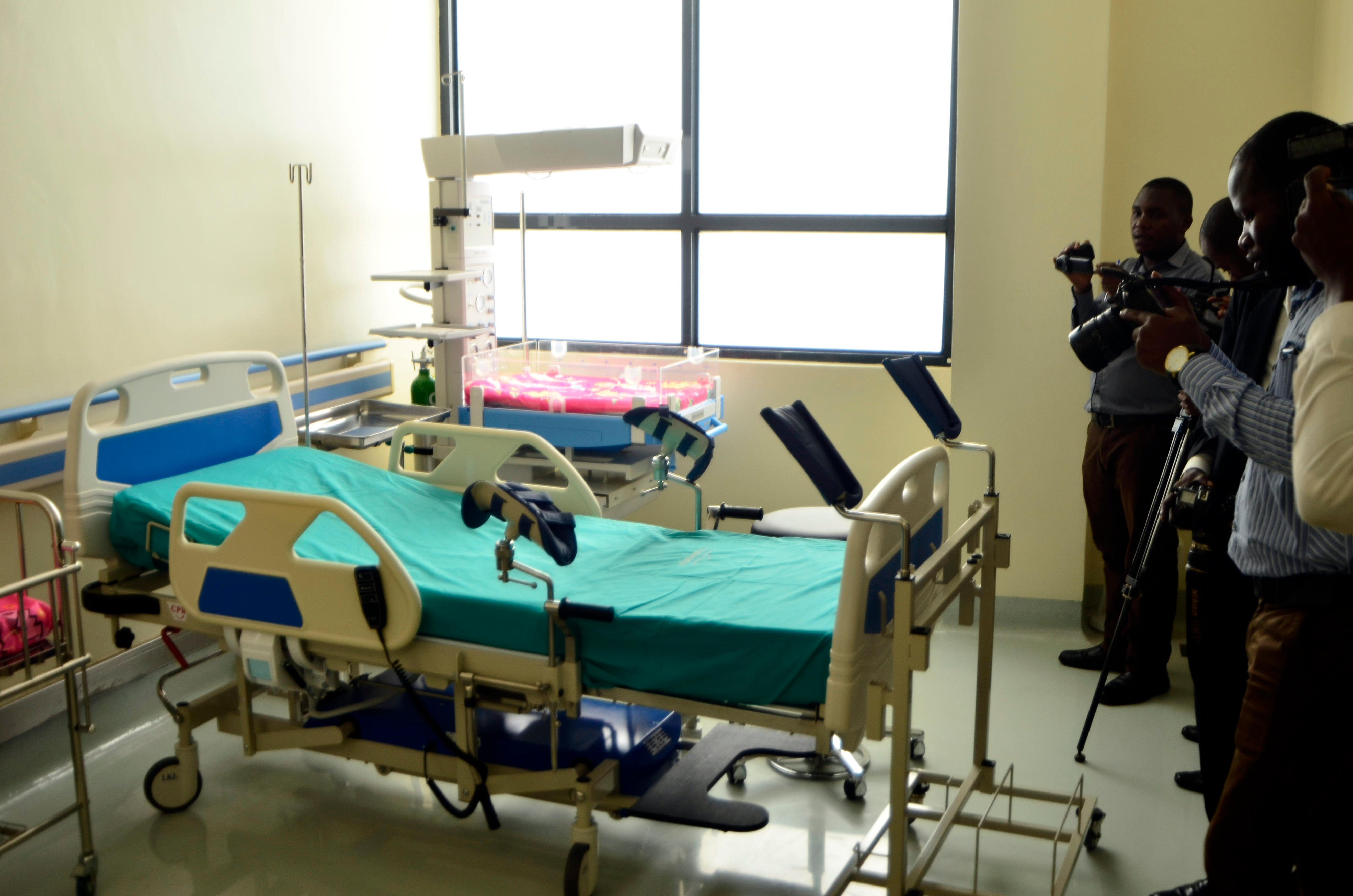
One of the ICU beds at the new Mulago Specialised Women and Neonatal Hospital. PHOTO | ALEX ESAGALA
“There is a lack of trained health workers, health centres frequently run out of drugs and only 58 per cent of births are attended by a skilled provider,” the report noted. One in three children was stunted and more than half lived in poverty.
In 2018, the World Bank noted that a child born in Uganda would only achieve 38 per cent of their productive potential in life “because of the limited investments that the country makes in developing children”.
Attention on Covid as other sectors suffer
As attention and resources shifted to coronavirus, other areas suffered. A study conducted in Busoga region found that maternal and newborn deaths increased by 33 and 35 per cent between March and August 2020, compared to the previous year.
Other indicators, including immunisations, access to anti-retroviral drugs and attendance of health facilities all fell as attention turned to coronavirus. While some recovered when lockdown measures were eased, the real death toll remains unclear.
Despite these challenges, Uganda’s initial response to the coronavirus pandemic was commendable, if rather chaotic. On March 18, without warning, the government announced a 32-day lockdown that started immediately. All mass gatherings, including restaurants, bars, churches, schools, weddings and political rallies were immediately suspended, as was public transport. Caught out by the abrupt decision, many people walked dozens of kilometres to reunite with their families.
On the afternoon of March 21, a 36-year-old businessman, who had flown to Dubai four days earlier, returned on an Emirates flight. The temperature scanners at Entebbe Airport clocked him at 38.7 degrees Celsius and he was taken into isolation. The next day, he was confirmed to have coronavirus. At least half a dozen other cases, mostly coming out of the Middle East, were later confirmed in the days that followed.
The ability to quickly identify suspected cases was a credit to Uganda’s health officials and reflected lessons learnt from dealing with epidemics, including several bouts of Ebola haemorrhagic fever, HIV, cholera, and the Zika virus.
“Within a week, you could get a sample from anywhere in Uganda delivered to the laboratory in Entebbe in a day,” says Dr Peter Waiswa, a public health expert.
This experience was crucial in marshalling a quick response to the disease. President Museveni named a scientific committee of advisers led by Dr Monica Musenero Masanza, a 55-year-old veterinary doctor who had also gained valuable experience as a microbiologist and epidemiologist working on Ebola in Uganda, DR Congo and Sierra Leone.
Yet other professionals at the School of Public Health were kept out of the response to the disease, including professors with decades of experience in dealing with HIV/Aids, including behaviour change communication.
“We made a mistake to make it a medical response,” Dr Waiswa says. “It should have focused more on behaviour change and we should have a wider debate on the response; non-medical experts need to be part of the discussion.”
Managing the crisis
Detection and prevention were one thing; managing the disease once it breached the border was another. Passengers arriving from countries with confirmed outbreaks of the disease were arbitrarily quarantined in a hotel in Entebbe that many considered pricey or overpriced, and then left to mill around and mingle once inside, potentially spreading the infection.
When this hotel filled up, at least one over-flow quarantine facility was set up in the middle of a particularly busy part of the capital, in a university student hostel whose selection was unclear.
When other well-connected people turned up at Entebbe airport, they simply refused to be quarantined and were allowed or forced their way out and away to their homes, further raising the risk of infection. When Entebbe airport was eventually shut down, some with the means and connections continued to fly in on scheduled flights arranged to repatriate foreign nationals out of the country.
Preventing and delaying the rise in cases during a pandemic is meant to buy time to prepare the population to avoid the disease, and to expand the capability and resources in the health sector for those who eventually contract it, but some of the response space created by the early lockdown was eventually lost.
Areas in need of urgent attention included testing kits, personal protective equipment, and specialist ICU equipment to deal with those who contracted Covid-19 and developed extreme symptoms.
The warning signs about Covid-19 had gone out at the end of 2019 and the beginning of the New Year, until the World Health Organisation confirmed the new aerosol-borne virus and the disease it caused, in mid-January 2020. The confirmation of the new disease and its spread outside China sparked a race for inventory of Covid-19 testing kits and PPE, even in countries with the facilities and industries to produce them.
In early April, both France and Germany accused the United States of hijacking their orders for PPE, with Paris calling it the guerre des masques, ‘the war of masks’. A senior German official accused the US of diverting 200,000 respirator masks destined for Berlin to America while they were in transit in Bangkok, Thailand.
A consignment of ventilators bought by Spain were impounded in Turkey, where they had been manufactured. The Turkish government said the treatment of its citizens was a bigger priority than export revenues.
This fight between major players was bound to suck the life out of smaller countries like Uganda. Officials declined to confirm how much PPE was already in the country before the outbreak of Covid-19 and how much had been ordered by the time the global treasure hunt broke out.
Relief came on March 24 when a consignment from Jack Ma, the billionaire owner of Chinese e-commerce giant Alibaba, landed at Entebbe airport, part of a larger donation to developing countries, including Africa, to save them from the stampede. The consignment included 20,089 test kits, 741 pieces of PPE, 1,111 face shields and 100,000 N95 face masks.
Yet, despite the donation from Jack Ma, by the time the workers at ICU at Mulago hospital rebelled in August, the country was already facing a crippling shortage of PPE. Frontline health workers were those left exposed.
On May 31, the Health ministry reported that seven health workers, including three nurses, two doctors and two senior technocrats, had tested positive for Covid-19. By nature of their jobs, the health workers were at higher risk than most of contracting the disease but an official from the Health Workers’ Union said the infections could have been prevented.
“The situation is critical, many people are working without PPE,” Dr Mukuzi Muhereza, secretary general of the Uganda Medical Association, told Reuters news agency a few days later, warning about a shortage of gloves, face masks, face shields and aprons in most hospitals. “That is hampering the fight against Covid-19, because there’s fear among health workers that any time I touch a patient, I might be a Covid-19 patient myself.”
Poorly protected from the virus and constantly exposed to it as the number of patients rose steadily, the number of health workers contracting the disease and even dying from it continued to rise. In early September, six health workers tested positive for the disease at Lira Regional Referral Hospital, leading to the death of a senior medical officer.
In an emailed response to this newspaper in October, the Ministry of Health defended its supply of PPE to health workers.
“Government has tried to provide adequate protective gear, but we have had times when stocks are low just like any other country, including developed countries,” it said in a statement provided by spokesman Emmanuel Ainebyoona. “There can be shortages as long as we consume. The shortage can come but as a government, we continue providing as and when they need protective gears.”

Emmanuel Ainebyoona, Health ministry spokesperson.
The spokesman also defended the supply of PPE to health workers at Mulago ICU, despite clear warnings that it wasn’t fit for use in hospitals:
“The KN95 was labelled ‘Not for Medical Use’ because at the time, there was a ban on export of medical masks from China because they needed them for their internal market. We did not take that for granted but also forwarded samples of the KN95 to the National Drug Authority (NDA) for testing, which was approved for medical use. It was still an uphill task to convince our health workers but now on a good note, we have started making all these supplies in the country and NDA is fully involved to ensure that we have the best products to ensure safety of our health workers.”
He added: “It is understandable when our health workers have reservations over these KN95, but to assure you these are similar to those used in other countries. We just need to allay anxiety as we make available several different types so that people make optional choices and feel safe.”
In response to some of the PPE that was too small for the health workers at Mulago ICU, the spokesman said: “The sizes are different because face shapes and sizes are also different. The masks, therefore, cannot fit all. If the health worker does not have a well-fitting mask, we do not recommend him or her to enter the Covid-19 isolation areas.”
Several health workers interviewed questioned the practicality and wisdom of this guidance.
“In a country with less than 70 specialists with very specific skills needed to work in ICUs, you don’t have the luxury of choosing whose face fits the mask,” a health worker said on condition of anonymity. “The idea is just preposterous.”
The PPE shortages have continued even after the Health ministry response and reassurances, as have infections among health workers.
On Thursday, Kamuli District was the latest to shut or scale down its hospital operations after 27 new cases were confirmed from tests done last week. Of these, 20 are medical workers.
By the time the rebellion in Mulago happened, individual and institutional donors had been lining up to donate money and assorted items to anti-Covid-19 efforts. Many donations included PPE, including face masks.
In May, President Museveni had presided over the launch of a factory in Namanve Industrial Park on the outskirts of Kampala which, the official State House statement noted, had the capacity to produce more than half-a-million face masks daily.
In its statement to this newspaper, the Health ministry blamed the delayed completion of Mulago on the pandemic.
“We started using Mulago ICU before it was fully completed due to the urgent need for ICU services for the Covid-19 pandemic because it is well equipped with state-of-the-art machines for life support. There are isolation rooms in this ICU installed with negative pressure, which was yet to be switched on and tested but the contractor could not complete commissioning them due to Covid-19,” the ministry noted.
“There is no other ICU in Uganda with a similar system. The expert ought to have come in from abroad to complete this work but due to lockdown, they could not come. The medical personnel had to devise safe ways of working within the prevailing situation.
“The air conditioning was switched off because air conditioning increases the spread of the virus into the air and thus would increase risk of infection. Natural air flow was used because it is safer than the air conditioning without the negative pressure. All this was done to ensure safety of the health workers. The use of air conditioning can be moderated by the health workers, depending on whether it is deemed safe. The AC systems are all fully functional.”
However, a project completion report from the Africa Development Bank in December 2019, said the hospital would be “operational” by the end of that year, more than three months before the airport and borders were shut due to the pandemic.
The banks report is generally positive about the project. It notes that the funding, which resulted in two new 170-bed referral hospitals at Kiruddu and Kawempe, as well as the renovation of Mulago, had “succeeded in contributing to the improvement of access to quality and affordable health care services for the population of the Kampala Metropolitan Area.”
But the report is critical of the decision to turn Kawempe into a specialised obstetrics and gynaecology hospital and Kiruddu into one specialising in medicine and surgery. This means a pregnant woman living close to Kiruddu has to cross the city to Kawempe, 10 kilometres away.
A new 400-bed specialised women and neonatal hospital had also been built at Mulago, with a $30 million (Shs110b) loan from the Islamic Development Bank. But the charges at the new hospital, which range from UShs50,000 for consultation to Shs2 million for C-section deliveries, are out of reach for many in a country where more than 20 per cent of the population lives on less than Shs7,400 a day.
The delay at Mulago could be traced to extra civil engineering works, which had created a funding gap of $9.5 million, which the government was required to meet. While the government was slow to find this money, it had quickly mobilised a sovereign guarantee of $350 million (Shs1.3 trillion) for a private hospital at Lubowa, on the outskirts of the city, despite vocal opposition from civil society groups, health worker associations and Members of Parliament.
The second problem was with the cost and quality of the building, including of key components of the national referral hospital, like the oxygen plant. According to the Ministry of Health, “all the 900 beds in this newly-renovated lower Mulago have a port for piped oxygen and other medical gasses, therefore, there was need for replacement with a new and more powerful oxygen plant to service this need.
“The house to accommodate this new plant is almost complete and the equipment arrived in the country recently, ready for installation. But in the meantime, there is a steady oxygen supply for the patients from the upper Mulago oxygen plant and this is supplemented with oxygen cylinders. A total of 50 new oxygen cylinders were procured to supplement the existing 27. There is a dedicated new truck that transports these cylinders for refilling to avoid any shortfall.”
Specifically, the ministry said: “The allegation that two people died because of lack of oxygen is not true. Even where there is oxygen, someone can still succumb so we cannot attribute death to only lack of oxygen.”
However, this newspaper has seen evidence from inside the ICU at Mulago hospital showing low levels of oxygen delivered to patients. Frontline health workers confirmed to this newspaper that oxygen levels from the new plants at Mulago dropped from above 90 per cent to as low as 24 per cent by the time it reached patients.
Another patient, a 72-year-old man, was referred to Mulago from Rubaga Hospital, put on oxygen, but continued to deteriorate. He was eventually placed on an oxygen cylinder but by then, it was too late. He had died, without oxygen. “He might have survived in Rubaga,” a health worker told this newspaper.
The oxygen plant at Mulago was installed by BHL Healthcare, a Chinese-owned firm based in Kampala. Incorporated in 2011, the firm has supplied medical equipment to several major hospitals in the country, including oxygen plants at Mulago, Kiruddu, Kawempe, Mengo and the International Hospital Kampala (IHK).
The same company installed an oxygen plant at Mengo Hospital at a cost of Shs187 million. Another one installed by the same company at the IHK on a pay-as-you-use model cost Shs53 million for three-phase electricity and building a filling house, with each oxygen cylinder filled at about Shs20,000.
A Health ministry official who spoke on condition of anonymity because they are not authorised to speak to the media, put the cost of a similar oxygen plant installed at Mulago hospital by the same company at “just over a million US dollars”.
Theft?
Not all donated masks were medical grade, but many were KN95 fit for use in hospitals, including the country’s largest and highest ICU at Mulago hospital. The Chinese embassy had donated 2,000, on top of the 100,000 from Jack Ma’s foundation. Yet months later, many citizens are yet to receive their government-issued face masks and medical workers remain exposed. Where have the masks gone?
One day, in early or mid-April, officials attended a meeting at the Health ministry headquarters, a stone’s throw away from Mulago hospital, which had been designated the admission centre for Covid-19 patients. The discussion moved to PPE, Jack Ma’s donation, and other masks bought by the government. The tally, according to sources familiar with the matter, should have been 500,000 masks. A call was placed to the National Medical Stores, where the PPE had been taken for safe custody. The ministry officials wanted to know how many were in the warehouse.
“Five thousand,” the NMS official said.
‘Did you say 50,000?’ the Health ministry official checked.
“No, one-two-three, five thousand. We have five thousand masks,” the NMS official confirmed.
The news was greeted with disbelief and a team of officials from the ministry, including a minister, drove across town to the NMS warehouse to see for themselves. It was true, there were 5,000 in store and the rest could not be traced.
An official who had been designated as part of the anti-Covid operation were so distressed by the missing PPE, he asked to be reassigned.
It is not clear where the face masks ended up. Next door, in Kenya, of the 100,000 face masks donated by Jack Ma, only 20,000 were delivered to the country’s national medical stores. The rest were diverted and sold onto the open market; an official investigation later revealed. In Uganda, there is no evidence of an official investigation into the missing masks.
Dying with dignity
After months of suppressing the virus, the infection rate began inching upwards with the start of the election season, starting with the NRM party parliamentary primaries and has continued to rise as the wider campaigns started. So has the death rate.
In the third week of November, there were 1,931 new confirmed cases and 15 deaths. In the past week, infections rose by 14 per cent to 2,215, but while deaths more than doubled to 39.
ICU beds across the country are full, with patients waiting for others ahead of them in the queue to recover or die. A consultant cardiologist recently contracted the disease and needed an ICU bed. It took the intervention of the Health ministry permanent secretary Diana Atwine to find him one.
Dr Waiswa of the School of Public Health says a long-standing debate over whether to prioritise primary health care (prevention) or also invest in clinical capacity (treatment and cure) needs to be revisited.
“You cannot avoid investing in hospitals,” he says. Where ICUs have been built, they either lack equipment or the trained specialists to operate them.
Yet even where it has been built and manned, such as at Mulago, defects and deficiencies lurk around the corner. After the health workers protested in August, senior Health ministry officials worked the telephones to try and convince them to return to work.
“But what do you want us to do when you bring them here and things aren’t working?” one health worker reportedly asked.
“At least let them come and die with dignity,” the senior official on the other end of the line reportedly said.
Additional reporting by Patience Ahimbisibwe



