Prime
Man axed to death after girlfriend found him taking ARVs-police
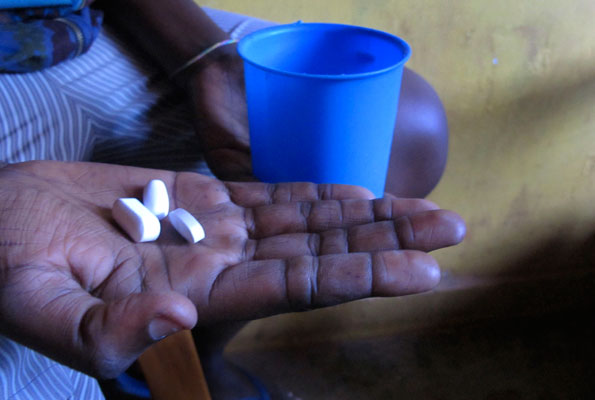
A patient prepares to take the daily dose of drugs recently. A woman in Hoima District in western Uganda has been detained for allegedly killing her boyfriend after she reportedly found him swallowing anti retrial viral drugs. File photo
What you need to know:
- The case is being investigated at Hoima Central Police Station under reference 1101/2019.
A woman in Hoima District in western Uganda has been detained for allegedly killing her boyfriend after she reportedly found him swallowing anti retrial viral drugs (ARVs).
Police said on Thursday that Emmanuel Tumusiime, 35 was hacked to death at his home in Kijumba cell in Kigorobya town council at around 6pm on Wednesday.
The Albertine regional police spokesperson, Mr Julius Hakiza said their preliminary investigations had revealed that Tumusiime was hit on the head using an axe.
"Upon realizing that the lover was dead, the suspect locked the house and jumped on a Boda boda to Hoima central police where she reported a case of murder," Mr Hakiza said.
At police, the woman reportedly confessed to killing her partner.
She reportedly claimed that she was hurt and disappointed that her partner could have infected her with HIV/AIDS.
She was arrested and detained at Hoima Central Police Station on murder charges.
Police detectives rushed to the scene and cordoned it off to conduct further investigations, Mr Hakiza said.
The case is being investigated at Hoima Central Police Station under reference 1101/2019.
"We call upon the victims of HIV Aids to always inform their partners and attend counselling centres because falling victim of HIV/Aids isn't the end of life," ASP Hakiza advised.
RELATED