Beating Covid: He asked God to forgive him while on ICU bed
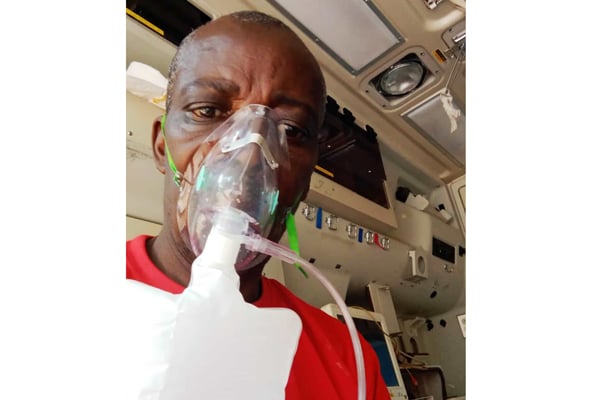
Birungi’s total hospital bill was Shs11.5million. PHOTO | COURTESY
What you need to know:
- In this series ‘Beating Covid’, we trace victims who caught the virus and overcame it. Alex Ashaba tells the story of Mr Clovis Birungi who went into coma twice before regaining his consciousness in the ICU.
Mr Clovis Birungi is a resident of Kanyadahi Village in Ruteete Sub-county, Kabarole District. He contracted Covid-19 in November last year. Mr Birungi, to this day, has no clue on how he contracted the virus, saying he was mostly home and would at times move to Fort Portal City.
In November, he started feeling unwell but did not seek medical advice.
“I thought I had malaria and that I would recover soon. I was weak for two weeks and later I developed other signs. I lost appetite, lost smell and had fatigue. I was bedridden at home for three days,” Mr Birungi says.
On a Sunday, when he was in his bed, he suddenly lost his memory and had difficulty in breathing. His family members had to call a doctor. When the doctor came, he was put on drip and started getting some medication.
Mr Birungi recalls what happened on November 30, at around 3am. He collapsed and went into coma. His oxygen levels dropped to 75. His wife made an alarm in the night alerting the other family members that all was not well. His son came, got him and rushed to Fort Portal Regional Referral Hospital. By the time he reached the hospital, his oxygen levels had reduced further to 33.
“I was in a coma all the way from home to the hospital. I was admitted the following day when I regained consciousness and my memory. But later in the evening, I went into coma again,” he says.
He was tested for Covid-19 but the results took two days to return, in the meantime, his condition was getting worse, so the doctors decided to refer him to another hospital in Kampala.
However, his family members were divided over which hospital to take him to. Some were worried that he would die before reaching Kampala, but his wife and son insisted that he needed to be transferred saying that if he died, he would die trying to get better treatment.
“My sister Margaret Muhanga (Minister of State for Primary Healthcare) immediately looked for an ambulance that took me to Kampala,” Birungi says.
They left Fort Portal at midnight and arrived in Kampala at 4am. While in the ambulance, he was on oxygen with a doctor who kept monitoring his oxygen levels. On his arrival in Kampala, the first health facility they went to had no oxygen. He was rushed to Victoria Hospital, taken to another hospital for a CT scan and returned to Victoria Hospital.
“By the time I regained consciousness, I found myself in the ICU surrounded by machines and on oxygen cylinder. That’s when I came to know that I had been diagnosed with Covid-19 and my lungs had been damaged,” he says.
On receiving this news, Birungi says he thought he was going to die because three people died on the same ward.
“At that moment, everything was about my Lord God, I started asking God to forgive me for whatever I did that was wrong to Him. I told Him if I survived, I would give testimony to Him and to other people that God is great,” Mr Birungi says.
To avoid worrying about his condition, one of the doctors advised him not to think about other things but only about his life. He also discouraged him from using the phone while in the ICU.
Mr Birungi says his family members did a great job in mobilising resources as the total hospital bill was Shs11.5million.
At Victoria Hospital, he says the management told them to first make an advance deposit of Shs5 million within two hours for the Intensive Care Unit (ICU), this was eventually paid in three days.
On the third day, they were asked to make another deposit of Shs10 million as the hospital management had estimated they would need Shs30 million for treatment in ICU.
With the hospital bills shooting up, his son and other family members requested for a transfer to Mulago National Referral Hospital.
In total, Birungi says they spent Shs6 million at Victoria hospital.
At Mulago Hospital, he was admitted in ICU on the third floor as his condition was still bad. He recalls that while at Victoria Hospital, the doctors prescribed a certain drug, for which a dose cost Shs960,000. He was supposed to take four doses.
However, at Mulago Hospital, the same drug was prescribed and costed Shs450,000 per dose.
Birungi spent 10 days on treatment and on the 8th day, he was taken off oxygen.
“When I was in ICU, I was in the hands of doctors who struggled to see that I recovered,” he says.
When he started recovering, he was removed from the third floor and taken to the High Dependence Unit on the fourth floor where he was put with other patients who were recovering.
On December 14, he was discharged with a certificate after tests indicated he was negative for Covid-19.
He thanks God that he recovered.
Ambassador
The Kabarole District Covid-19 taskforce is now using him as an ambassador in the fight against the disease. He gives his testimony and messages of hope to other patients who are suffering from Covid-19.
Mr Birungi advises that people need to avoid crowds and those who want to move should always put on their masks all the time and sanitise their hands and other items they touch.
“I have told people that Covid-19 is real. I am asking them to follow SOPs by the Ministry of Health and other guidelines,” he says.
Covid-19 study
As many as one in every two people hospitalised with severe Covid-19 go on to develop other health complications, according to comprehensive new research released last Friday.
Authors of the study said their findings showed a ‘‘profound’’ short- and long-term health impact on Covid-19 patients as well as on health and care services.
Data from more than 70,000 hospital patients across more than 300 British hospitals was collected for the research.
It found that the most common health complications were problems with patients’ kidneys and lungs, but neurological and cardiovascular conditions were also widely reported.
The rate of complications was high even among ‘‘young, previously healthy’’ patients, with 27 per cent of 19 to 29 year olds and 37 per cent of 30 to 39 year olds experiencing at least one complication after being hospitalised with Covid-19.
Authors of the research, published in The Lancet Medical Journal, said it should alert policymakers to the need to plan for long-term support for Covid survivors. ‘‘This work contradicts current narratives that Covid is only dangerous in people with existing co-morbidities and the elderly,’’ said senior author, Professor Calum Semple, from the University of Liverpool.




